Keywords: fibrosarcoma; Soft tissue sarcoma; Abdominal wall tumor; Wide local excision; Keystone flap; Uganda
Authors: Abdirahman Abdifatah Mohamed, MD Final Year PRS Trainee 1, Numan Omar Ibrahim, MD PRS Trainee 2, Rose Alenyo, MD Consultant Plastic Surgeon 3, Kalanzi Edris, MD Senior Consultant Plastic Surgeon 4. Kiruddu National Referral Hospital Kampala, Uganda.
Abstract
Fibrosarcoma is a rare soft tissue sarcoma with aggressive local infiltration and high recurrence risk. We present a 71-year-old Ugandan man with a giant epigastric fibrosarcoma causing a complex abdominal wall defect. Imaging showed invasion of subcutaneous tissue and rectus muscle without metastasis. The patient underwent wide local excision with 5 cm margins, followed by reconstruction using Prolene mesh and a modified keystone flap with skin grafting. Recovery was uneventful, demonstrating effective surgical and reconstructive management in a resource-limited setting.
Patient medical history
a 71-year-old male who presented with a two-year history of a progressively enlarging anterior abdominal wall mass. The lesion initially appeared as a small, firm nodule and gradually increased in size, eventually becoming a large, fungating tumor associated with ulceration, necrosis, and intermittent bleeding. There was no history of distant symptoms suggestive of metastasis. Imaging confirmed a locally invasive epigastric mass involving the subcutaneous tissue and rectus abdominis muscle, without visceral or distant spread.
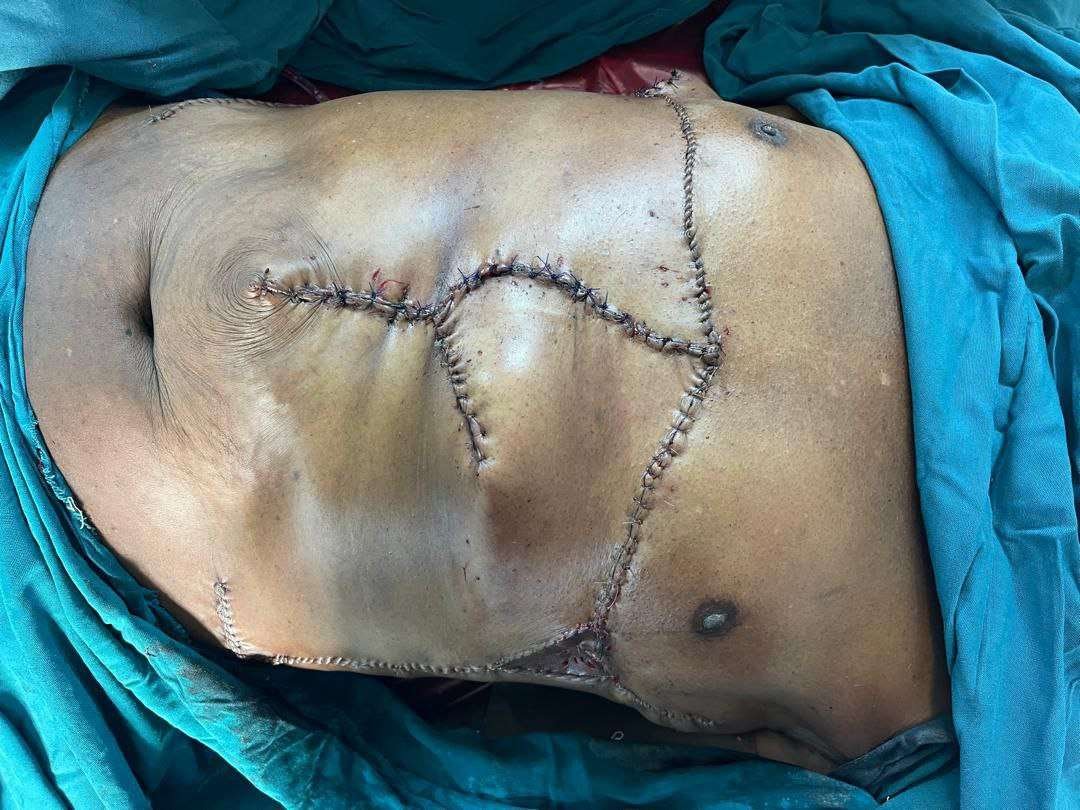
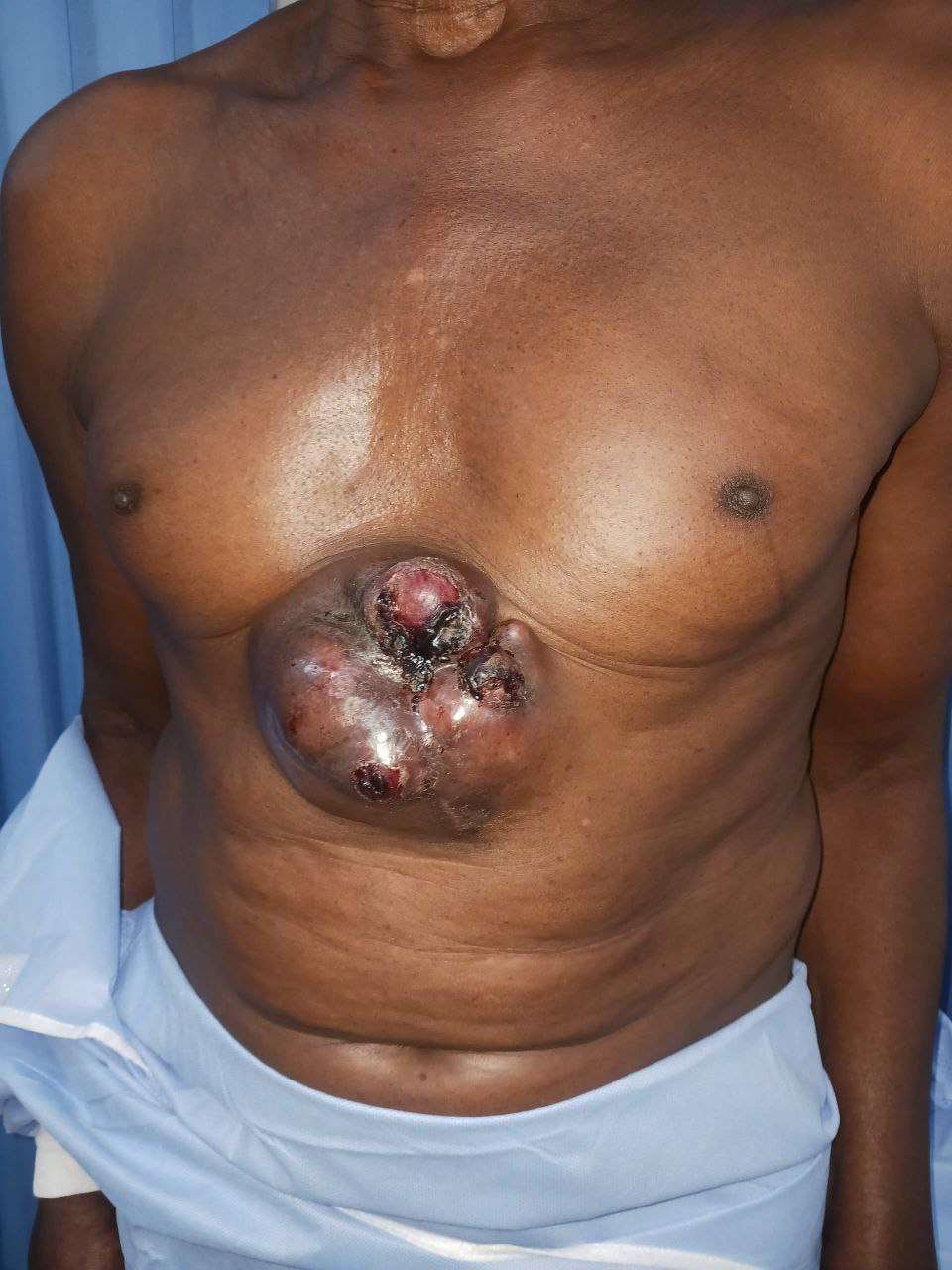
Before and After
Patient examination
On physical examination, the patient had a large, exophytic, fungating mass located in the supraumbilical (epigastric) region of the anterior abdominal wall. The lesion was deeply invasive with irregular margins and was associated with ulceration, areas of necrosis, and active bleeding. The overlying skin was stretched, tense, and partially ulcerated. The mass appeared fixed to the underlying abdominal wall musculature, suggesting muscle involvement. There were no clinical signs of peritoneal involvement, distant metastasis, or regional lymphadenopathy.
Pre-operative considerations
Pre-operative evaluation focused on accurate staging operability and reconstructive planning.
A contrast enhanced CT scan of the abdomen was performed to assess tumor size depth and involvement of the abdominal wall confirming invasion of the subcutaneous tissue and rectus abdominis muscle without peritoneal visceral bony or distant metastatic disease.
Histological diagnosis of fibrosarcoma was established.
The case was reviewed by a multidisciplinary team to determine oncologic margins and reconstruction strategy.
The patient age
nutritional status
comorbidities
and anesthetic fitness were assessed.
Given the anticipated full thickness abdominal wall defect availability of prosthetic mesh and local flap options suitable for a resource limited setting
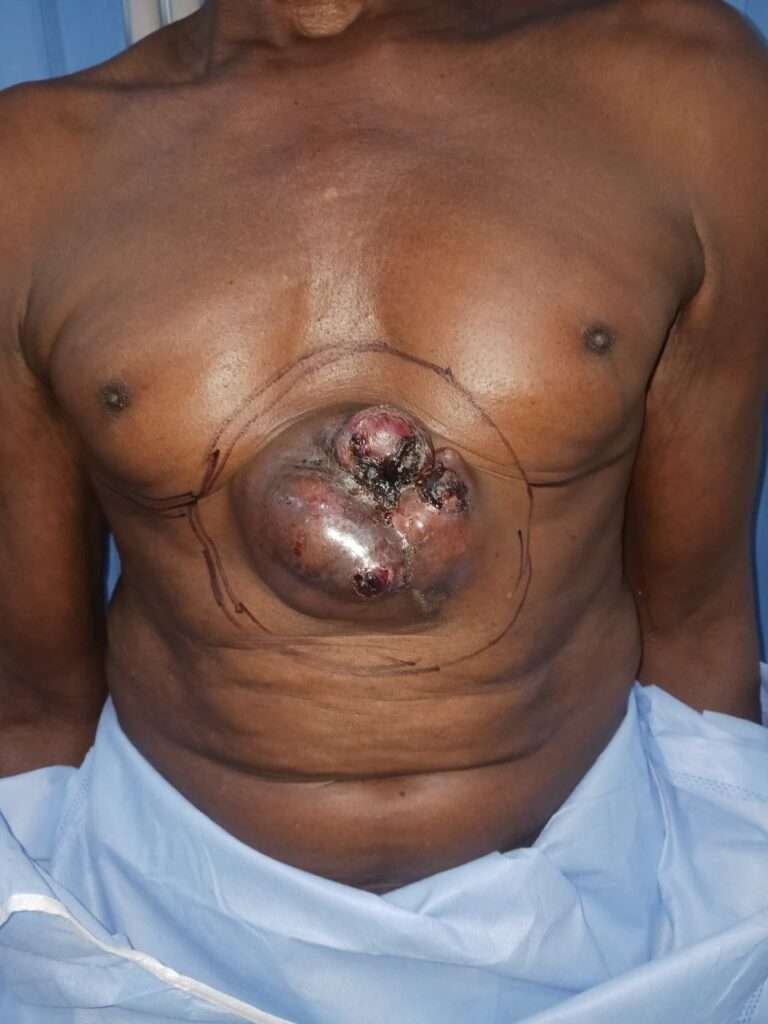
preop excision margins
Fibrosarcoma is recommended 2 to 3cm excision margins due to lack of intraop frozen section we marked 5cm margins to be in safe side
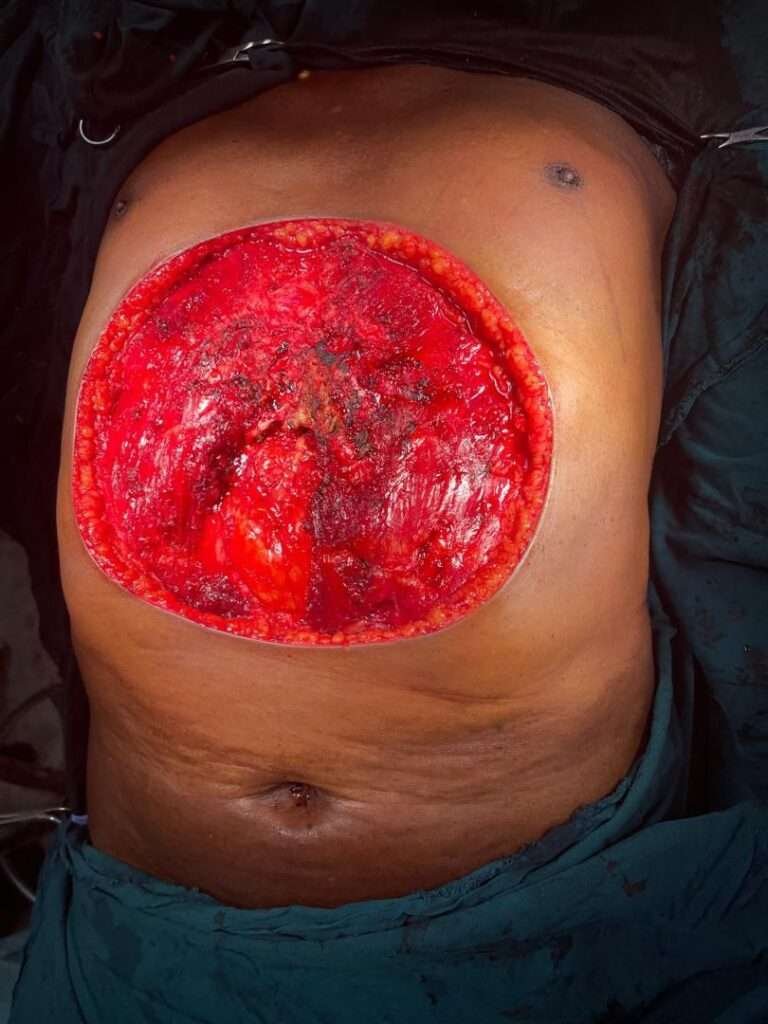
Intraop post excision
Excised full thickness skin up to parts of rectus abdomens creating defect about 25 to 30cm of lower chest wall exposing lower sternum lower ribs and upper abdominal wall exposing intraabdominal organs.
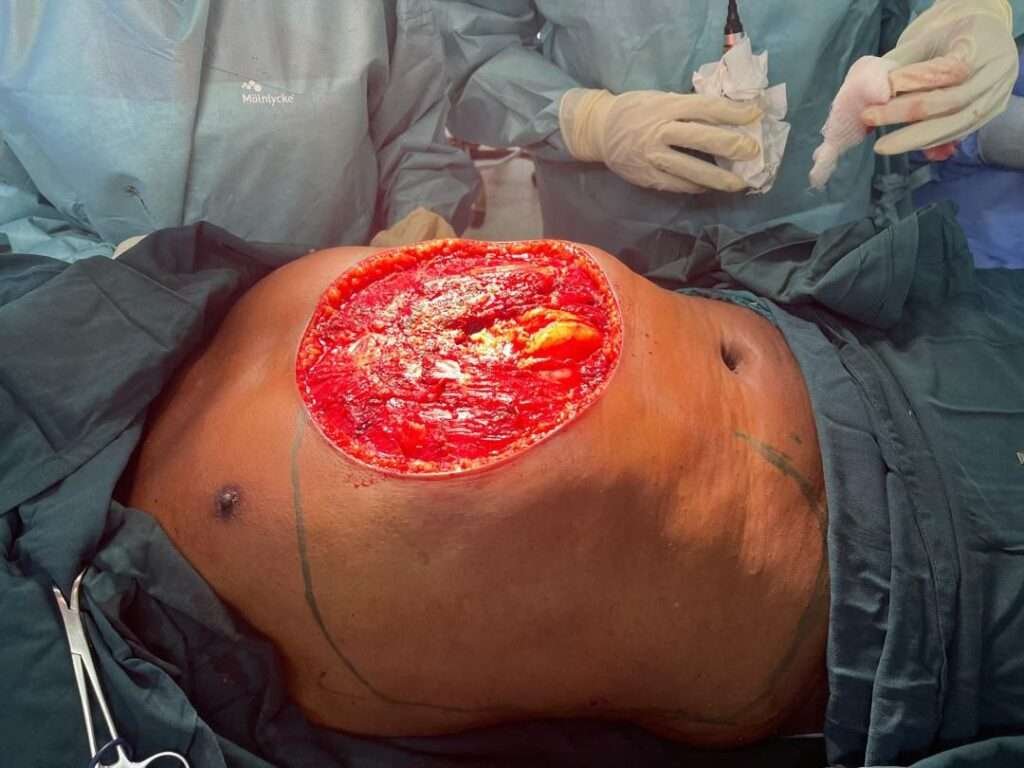
Intraop Flap markings
such a large defect free flap option will be one of the best options in developed settings due to lack of microsurgery in our settings we planned available loco regional option which is robust reliable can cover the defect and tolerate post op adjuvant radiotherapy
so Modified Keystone flap marked and this is one of the limbs of flap marking
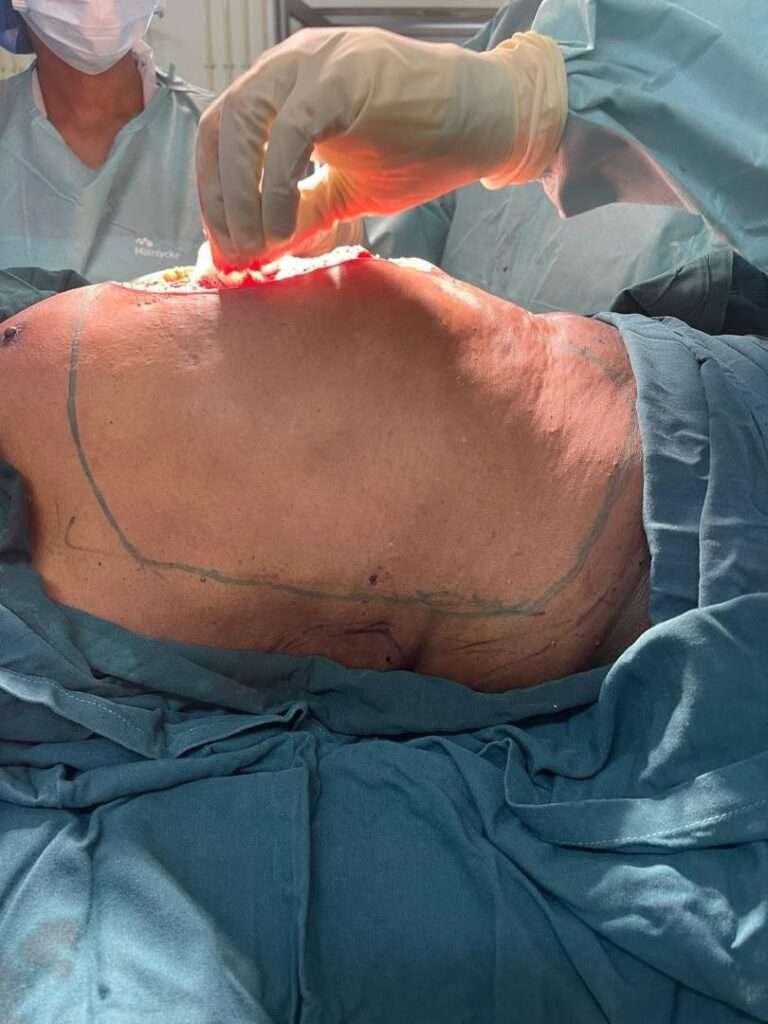
Intraop Flap markings
The other side limb of keystone marking
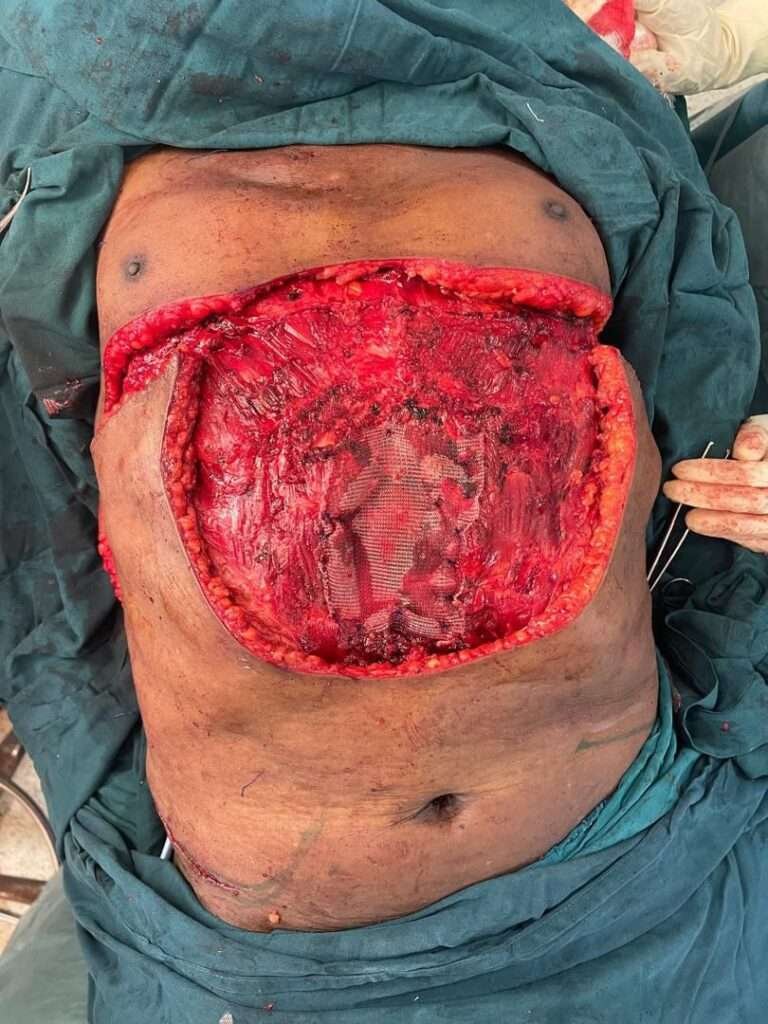
Intraop Raising Flap and Mesh Insertion
Before rising the flap we inserted synthetic Proline mesh patient could not afford Biologic one then raised the flap limbs and advanced a central incision and back cut added(Modified) in order to release and minimize the tension on one side and small areas remained which we grafted STSG
Pearls
Early recognition and wide local excision reduce recurrence
Mesh with modified keystone flap offers reliable
cost effective abdominal wall reconstruction without microsurgery
meticulous flap design and postoperative care optimize outcomes
Due to Limited Fibrosarcoma cases recourses in Africa journals this will be advantage and great reference.
Pitfalls
Delayed presentation
limited imaging access
and inadequate postoperative monitoring increase risk of complications and flap failure
poor planning can compromise structural and cosmetic results.
Post-operative plan
Immediate Postoperative Care
Close monitoring of vital signs and wound status
Assessment of flap viability (color temperature capillary refill)
Adequate analgesia and prophylactic antibiotics as per protocol
Wound and Flap Care
Regular sterile wound inspections and dressing changes
Early detection of infection seroma hematoma or flap compromise
Gradual mobilization with abdominal support to reduce tension on the repair
Continued care of split thickness skin graft until full epithelialization
Functional Rehabilitation
Encouragement of early ambulation
Avoidance of heavy lifting and activities that increase intra-abdominal pressure
Use of abdominal binder during the early healing phase
Oncologic Surveillance
Postop Adjuvant Radiotherapy
Scheduled outpatient follow up visits for clinical examination
Monitoring for local recurrence at the surgical site
Imaging studies as indicated based on clinical findings
Multidisciplinary review if recurrence is suspected
Long Term Follow Up
Assessment of abdominal wall integrity and functional outcome
Evaluation of quality of life and cosmetic satisfaction
Patient education on signs of recurrence and wound complications
References
Hadley GP. Management of soft tissue sarcomas in sub Saharan Africa. S Afr J Surg.
Lukande RL Wabinga HR Tumwine LK. Soft tissue sarcomas in Uganda a histopathologic appraisal