Keywords: Rheumatic Heart Disease, Embolism, Gangrene, Limb Salvage, Vessel-Depleted Extremity, Cross Leg Free Flap
Authors: DR RAHUL KAPOOR. MANIPAL HOSPITALS, DWARKA, NEW DELHI, INDIA – 110075.
Abstract
Limb salvage in a vessel-depleted extremity remains a formidable reconstructive challenge. We report a case of extensive lower limb gangrene following popliteal artery embolism in a patient with rheumatic heart disease and mitral stenosis. The defect involved exposed bone, necrotic tendons, and absent distal perfusion, with ipsilateral recipient vessels unsuitable for microvascular anastomosis. A cross-leg free flap with external fixation was performed using contralateral posterior tibial vessels. Venous congestion required supercharging with great saphenous vein anastomosis. The postoperative course was uneventful. Flap division at eight weeks demonstrated successful neovascularization, achieving durable limb salvage with progressive sensory and perfusion recovery at 18 months follow-up.
Patient medical history
Known case of Rheumatic Heart Disease with Mitral Stenosis. Patient developed complain of pain in left leg and foot, in June, 2024. Peripheral Angiography showed 80-90% occluded left external iliac artery & left popliteal artery and 100% left posterior tibial artery. Thrombolysis and plain old balloon Angioplasty done after 3 days of development of pain. Revascularization procedure was followed by development of compartment syndrome in left leg and foot and fever, with progressive discoloration of skin over lower half of leg, ankle and dorsum of foot. Discolouration turned into open wound with complete loss of skin cover, necrosed tendons and exposed bones of lower half of leg, ankle joint and proximal half of dorsum of foot. wound was heavily infected with pus discharge and foul smell.
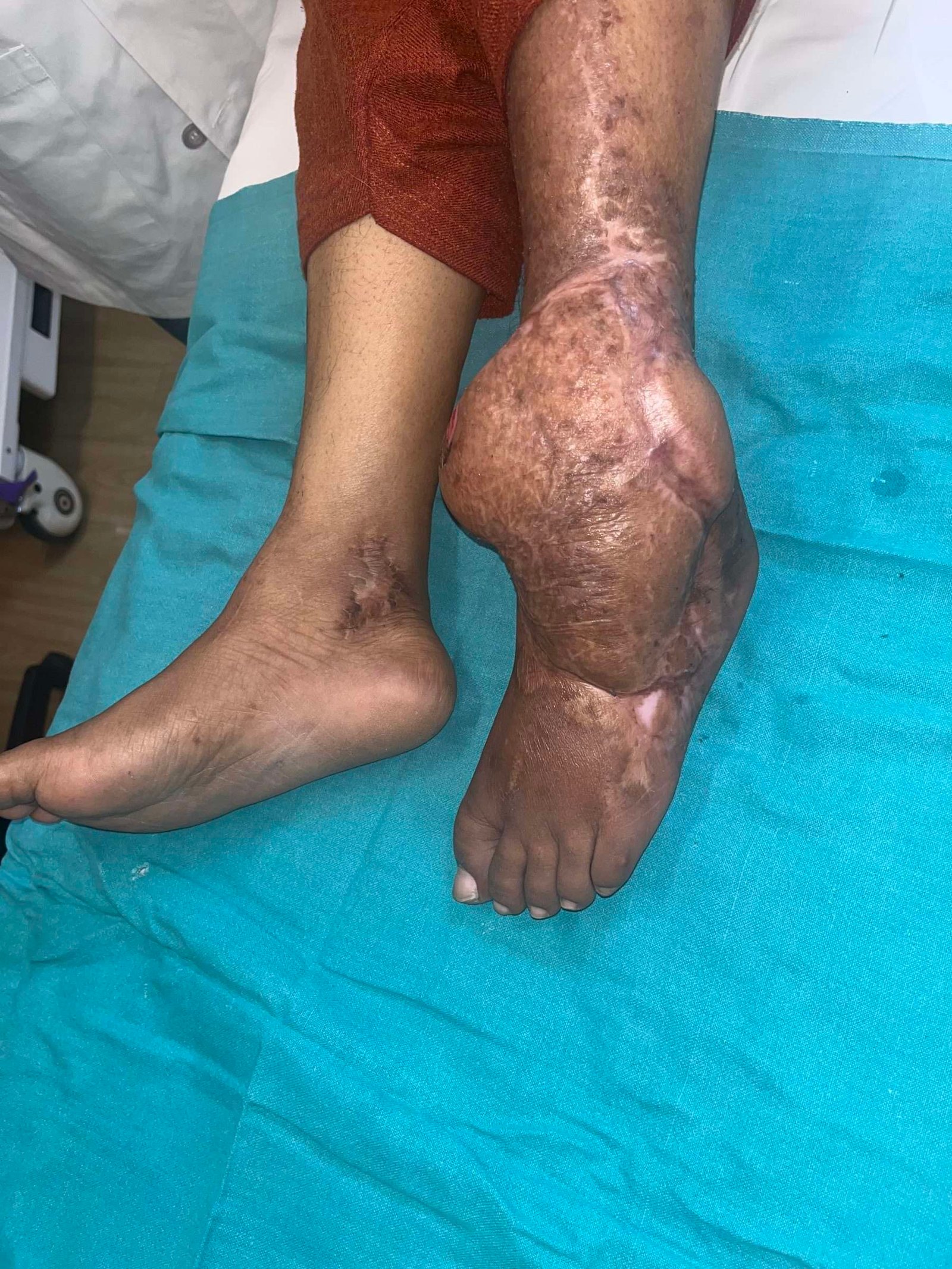
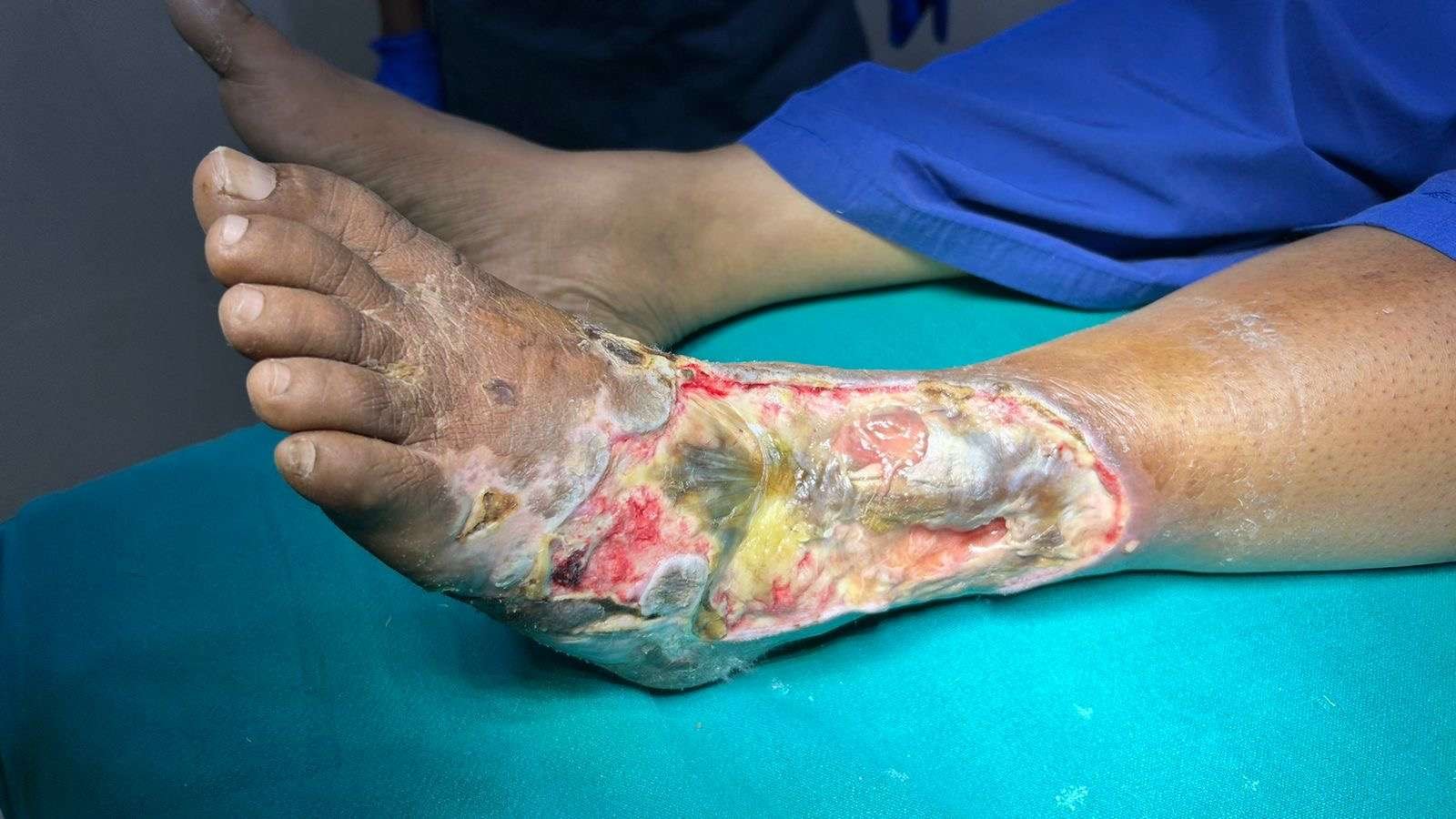
Before and After
Patient examination
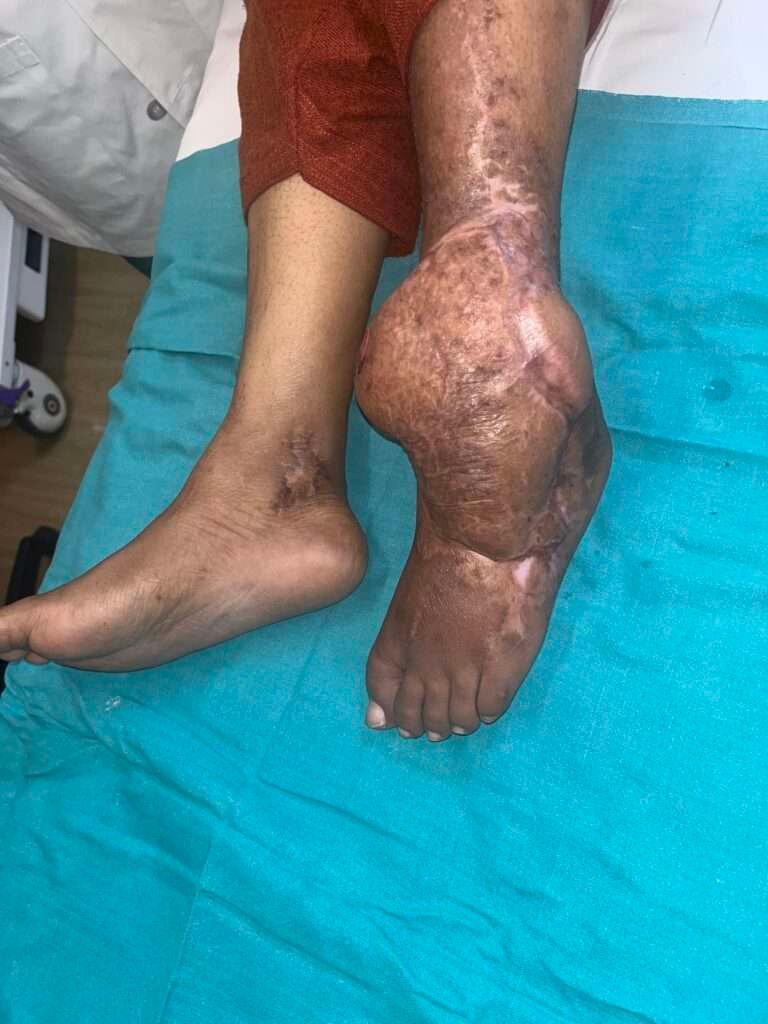
there was progressive discoloration of skin over lower half of leg, ankle and dorsum of foot.
Discoloration turned into open wound with complete loss of skin cover, necrosed tendons and exposed bones of lower half of leg, ankle joint and proximal half of dorsum of foot. wound was heavily infected with pus discharge and foul smell.
Ankle joint stiff with foot and all five toes in planter flexion. passive dorsiflexion incomplete u0026 difficult. There was loss of sensation in whole of foot and lower 2/3rd of leg with gross sensation of touch and decreased pain in upper 1/3 rd of leg. there was edema in whole of leg and foot. Pulsations could not be appreciated on examination in anterior tibial, dorsalis pedis and posterior tibial artery. Color doppler study showed
absence of flow in popliteal, posterior tibial artery stent and distally. Monophasic waveform in left anterior tibial artery. Colour doppler study right lower limb was normal. CT Angio showed The left CFA and SFA show normal course, caliber, and contrast enhancement. There was eccentric filling defect involving the proximal aspect of the left profunda femoris for a length of approximately 5 mm causing luminal narrowing by 50%-60%. The proximal left popliteal artery show good caliber and contrast enhancement. Distally, it show filling defect with near complete segmental occlusion. The origin of left anterior tibial artery as well as tibioperoneal trunk not visualized and re-formation of the posterior tibial and peroneal arteries with presence of multiple small collaterals. Dorsalis pedis artery is also not well visualised.
Pre-operative considerations
1. Patient willingness to save the limb, despite knowing all pros u0026 cons of undergoing surgery for limb salvage.
2. Ipsilateral side anastomoses not feasible for two reasons.
A.Pulsation in posterior tibial artery on palpation could not be appreciated due to edema. On doppler study, posterior tibial not visualised. The posterior tibial artery was collapsed without any pulsations.
B.Proximally, the tissue was edematous and scarred and popliteal artery was too proximal to achieve suffficient lenght after vein loop anastomoses, to ensure availibility of flap for adequate wound cover.
So, decision to plan anastomosis of flap to unaffected limb was taken, with due consideration for external fixator application, immobilization of both limbs in one position, micro movement and shearing in anastomosis with high risk of bleeding and flap loss, along with ongoing high dose of anticoagulation regime. there was also risk of thrombosis in posterior tibial donor vessel with associated complications. chances of pressure sore at dependent heel area was always there. Despite all complications explained to patient, she was willing for Surgery.
Planned flap – Due consideration was given for Free latissimus dorsi muscle flap with split skin graft. LD flap is broad flap with adequate length of pedicle and proximal muscle cuff to cover the pedicle and prevent its shear.
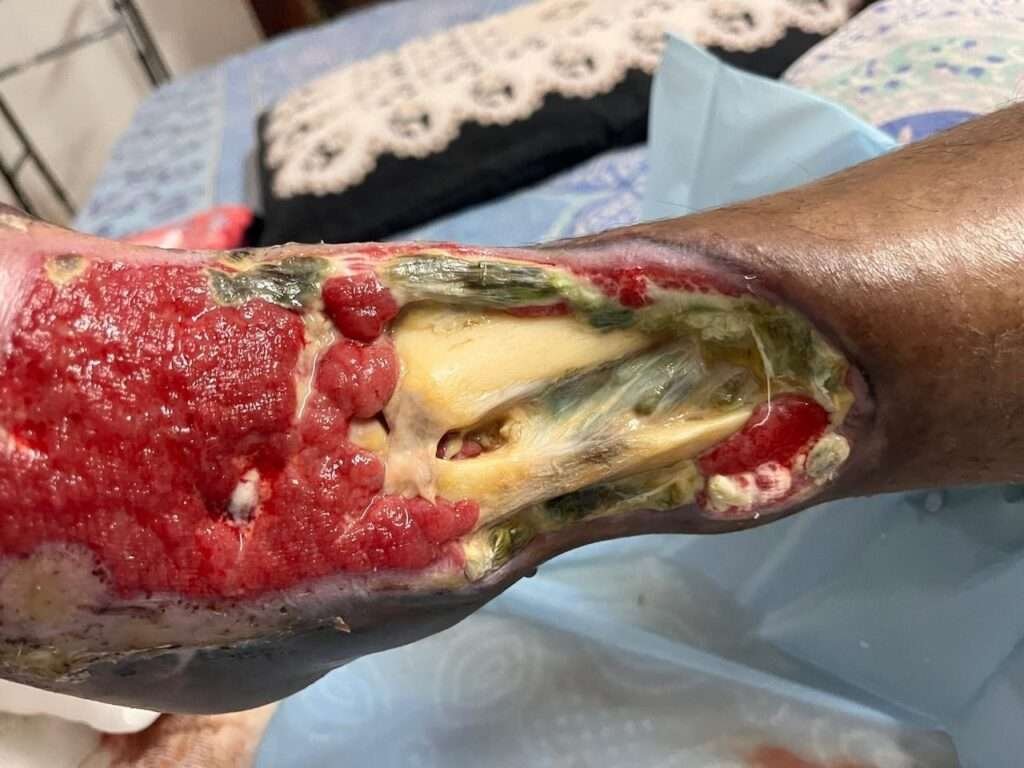
After serial debridement and VAC dressing
Serial debridement of infected and dead tendons and necrotic tissue before each successive VAC application under proper antibiotic cover and splintage
After 4 to 5 sittings of VAC dressings, patient was planned for final debridement under GA u0026amp; flap cover
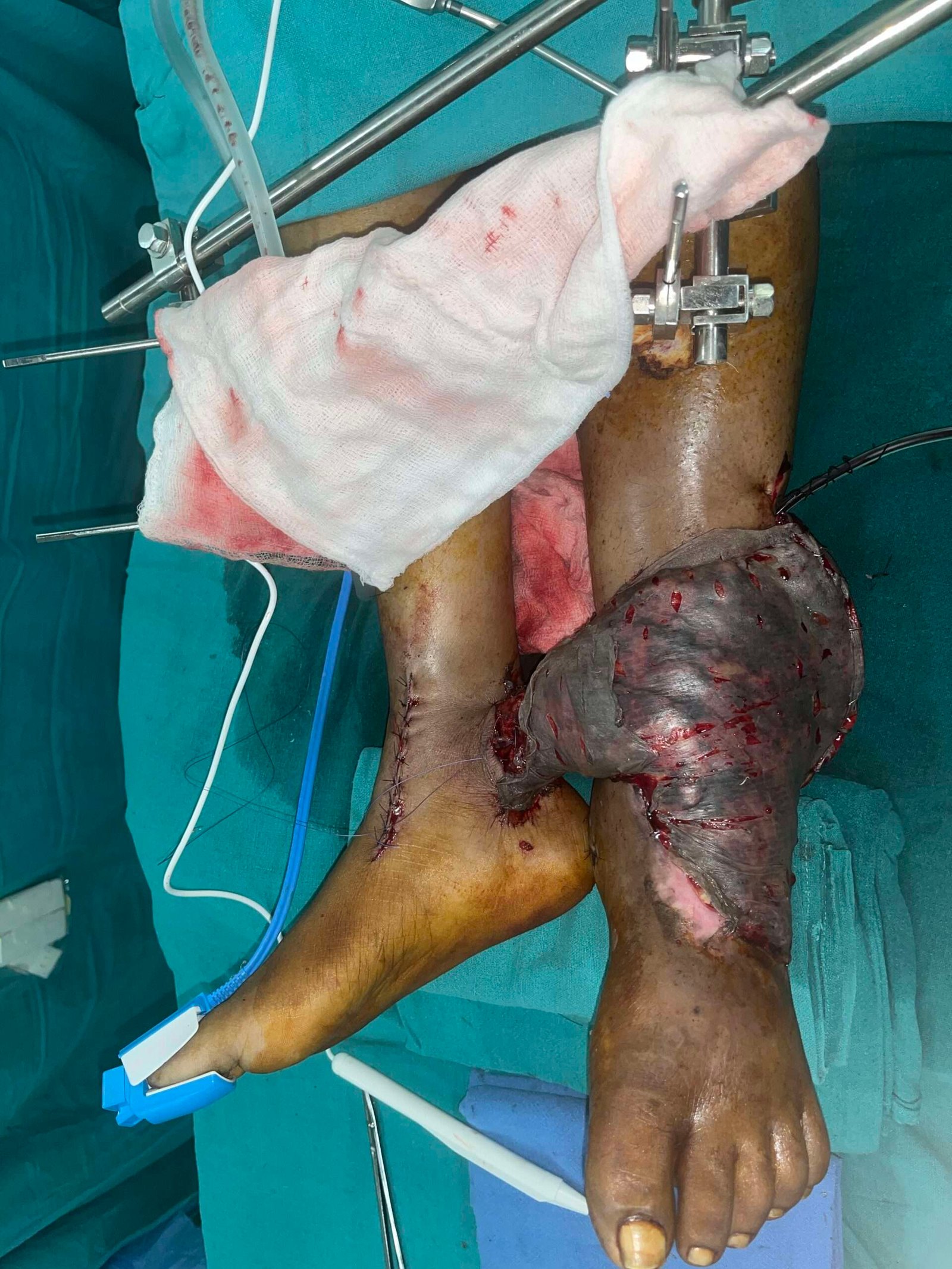
Cross leg Free latissimus dorsi muscle flap with split skin graft and limb fixed with external fixator
Due consideration was given for Free latissimus dorsi muscle flap with split skin graft. LD flap is broad flap with adequate length of pedicle and proximal muscle cuff to cover the pedicle and prevent its shear. Skin incision extended proximally to the junction of the proximal and middle thirds of the leg with debridement of dead and infected tissue – tendons and muscles under the covered area was done without tourniquet. Flap insetting was performed with two limbs of 18 G romovac drains placed from either side for wound irrigation and flap insetting done. Fixator application followed by vessel anastomosis
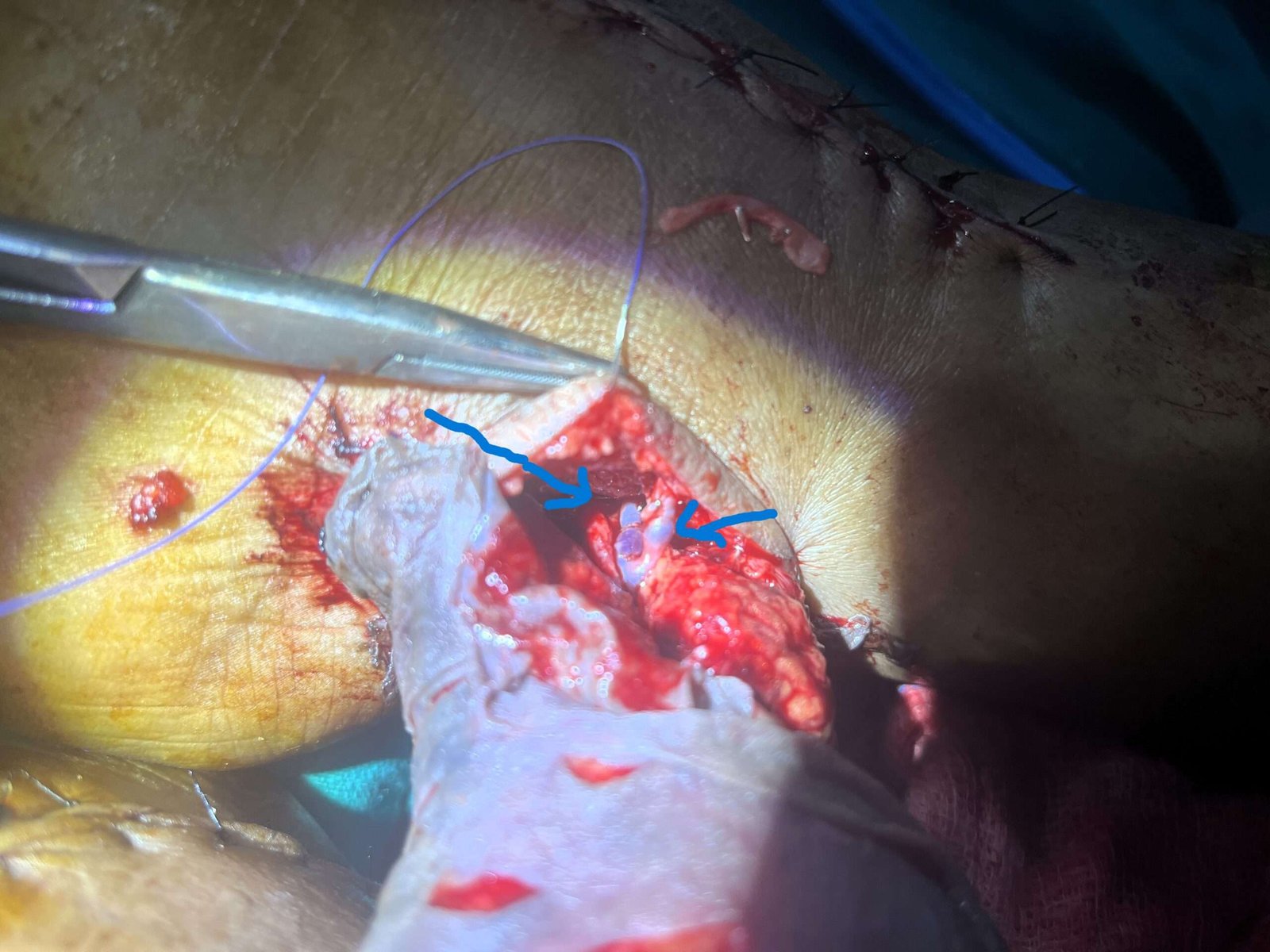
ETE Anastomoses of the thoracodorsal vein to the vena comitantes and ETS anastomoses of the GSV to the thoracodorsal vein
The thoracodorsal artery end-to-end anastomoses are performed on the posterior tibial artery, and thoracodorsal vein end-to-end anastomoses are performed on the vena comitantes.
The flap started showing signs of venous congestion; therefore, an additional anastomosis, the end of the great saphenous vein, was dissected out and delivered through the same anastomotic (posterior tibial) area and was anastomosed to the side of the thoracodorsal vein in an end-to-end fashion (proximal to end-to-end anastomoses with vena comitantes)
Flap detachment- 8 weeks post op after repeated conditioning with rubber tourniquet
Recovery – uneventful
Anticoagulation regimen – to maintain an INR between 1.5 – 2.5
wound bed irrigation done through – Romovac drain , which was continued for 3 weeks after surgery
Flap detachment was planned after 6 weeks, with intermittent compression was applied to the pedicle
ICG showed signs of vascularization from the wound bed with a tourniquet around the pedicle.
The patient did not show signs of flap ischemia, even at the distal end, suggesting good perfusion from the wound bed
The patient was discharged on the advice of physiotherapy, partial weight-bearing, and compression garments.
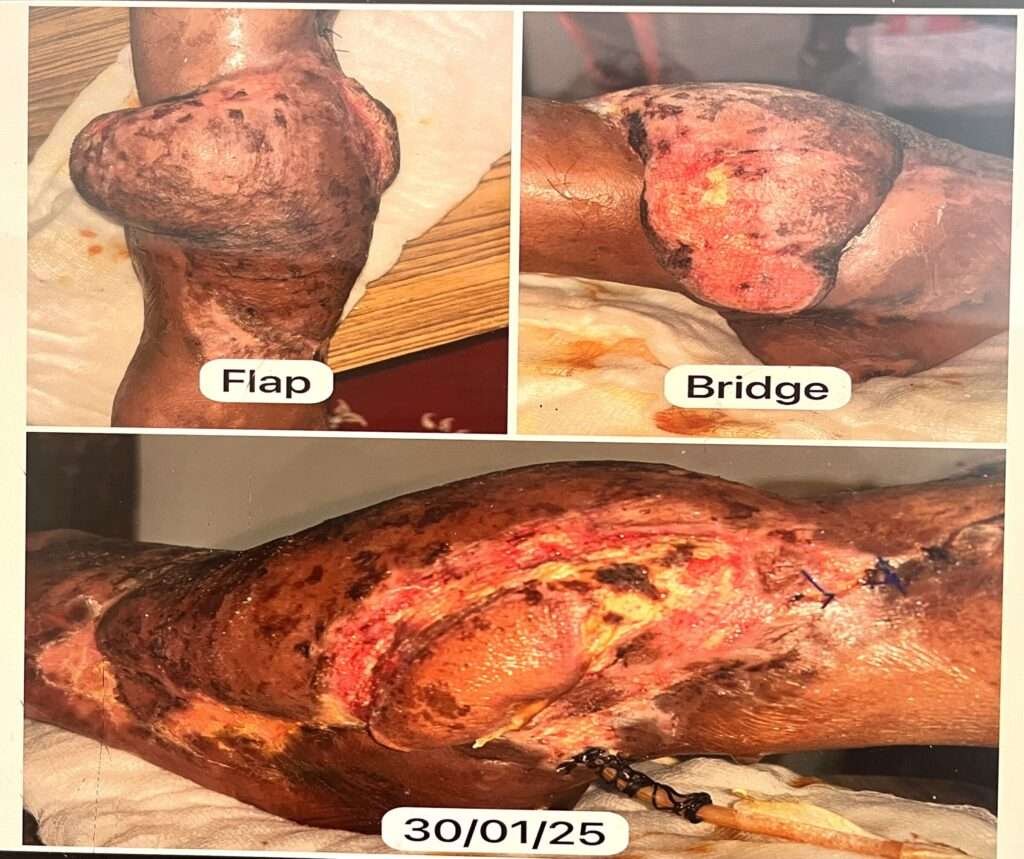
FLAP POST DETACHMENT 6WEEKS AFTER
There was uneventful healing and no necrosis either at distal most flap end or in the detached flap pedicle site. there was no flap debulking done.
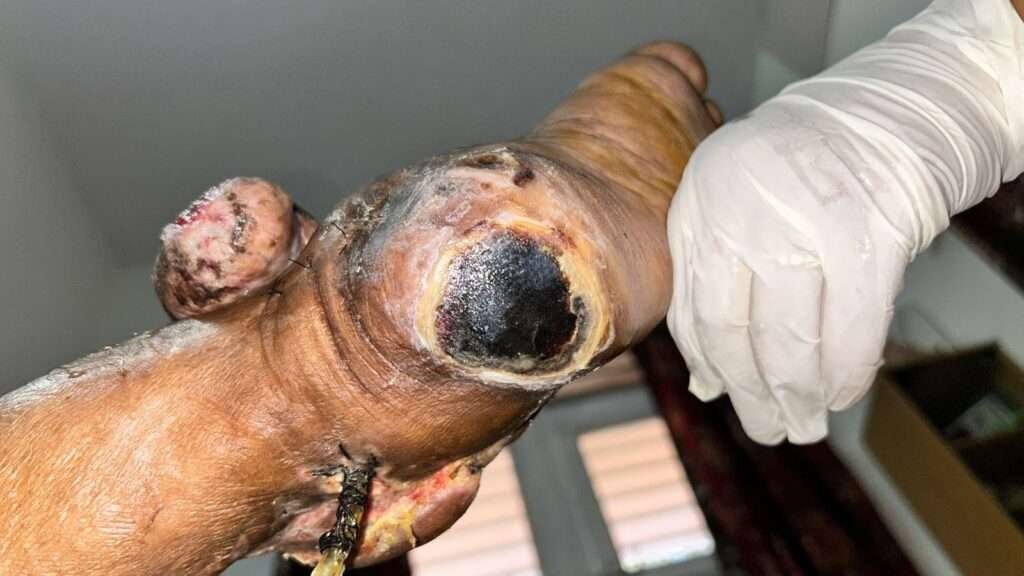
Pressure sore post detachment of cross leg free flap over left foot (affected extremity)
Pressure sore developed over heel area due to absence of any sensation.
it appeared to be full thickness in nature
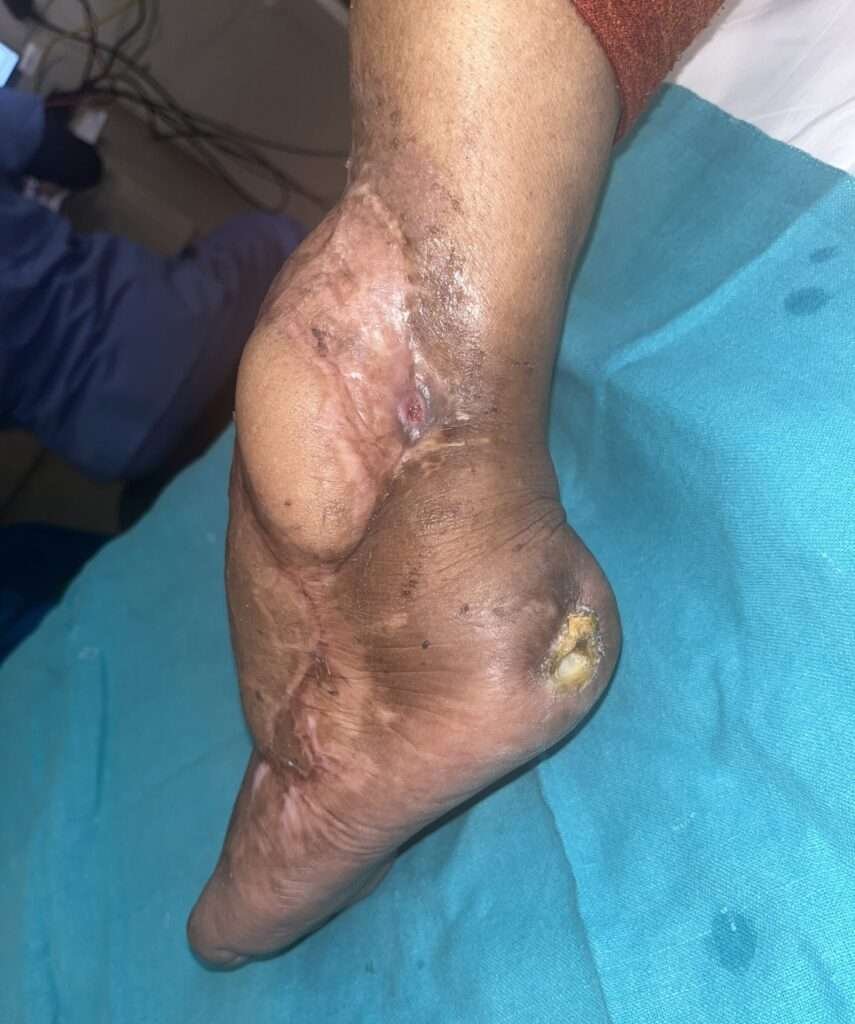
Pressure sore post detachment of cross leg free flap after 14 months managed conservatively ony with dressingd
Pressure sore developed over heel area due to absence of any sensation. With gradual returning of sensation, pressure sore healed well without any surgical intervention.
Pearls
patient willingness and appropriate counselling of all family members involved in patient care.
Adequate choice of flap.
Adequate immobilisation and anticoagulation. regular dressing to avoid pin track infection.
Proper post operative follow up to rule out development of discharging focus
Pitfalls
Development of pressure sore
Planter flexion and contracture
Development of osteoarthritis at ankle joint area.
Post-operative plan
Physiotherapy,
Massage
Ambulation and weight bearing – gradual and progressive over affected limb
References
The cross-leg free flap: A systematic review of the literature Karel-Bart Celie MD, Sarah Guo MD, Jessica Raya BS, Artur Fahradyan MD, Joseph Carey MD, Ara A. Salibian MD First published: 01 February 2024 https://doi.org/10.1002/micr.31144Digital Object Identifier (DOI)