Keywords: Latissimus dorsi flap, upper limb trauma, soft tissue reconstruction, vascular injury, degloving injury
Authors: Sumaira Sattar, FCPS (Plastic Surgery), Institution: SMBB Institute of Trauma, Karachi, Pakistan
Abstract
A 20-year-old female presented with a severe traumatic injury to the right upper limb following a road traffic accident involving a pedestrian–motorbike collision with subsequent run-over injury. The trauma resulted in extensive soft tissue loss, degloving injury, and associated vascular compromise. Initial management followed advanced trauma protocols, after which the patient was referred for vascular and reconstructive assessment. Imaging revealed brachial artery thrombosis with segmental radial artery injury; however, hand perfusion was maintained through collateral circulation. Following stabilization and vascular reconstruction using a reverse great saphenous vein graft, soft tissue coverage was achieved with an ipsilateral myocutaneous latissimus dorsi flapThe flap provided durable coverage of exposed vital structures and the elbow joint without the need for microsurgical anastomosis. At three-month follow-up, the patient demonstrated excellent functional recovery with satisfactory aesthetic outcome. This case highlights the reliability of the latissimus dorsi flap in complex traumatic upper limb reconstruction.
Patient medical history
A 20-year-old unmarried female, with no known comorbidities, presented to the emergency department five hours after a road traffic accident involving a bike-versus-pedestrian collision. Following the initial fall, the patient sustained a secondary run-over injury to the right upper limb. There was no history of loss of consciousness, head injury, or trauma to other body regions. Initial assessment and stabilization were performed according to trauma protocols, following which the patient was referred to the plastic and vascular surgery teams for definitive management of the limb injury.
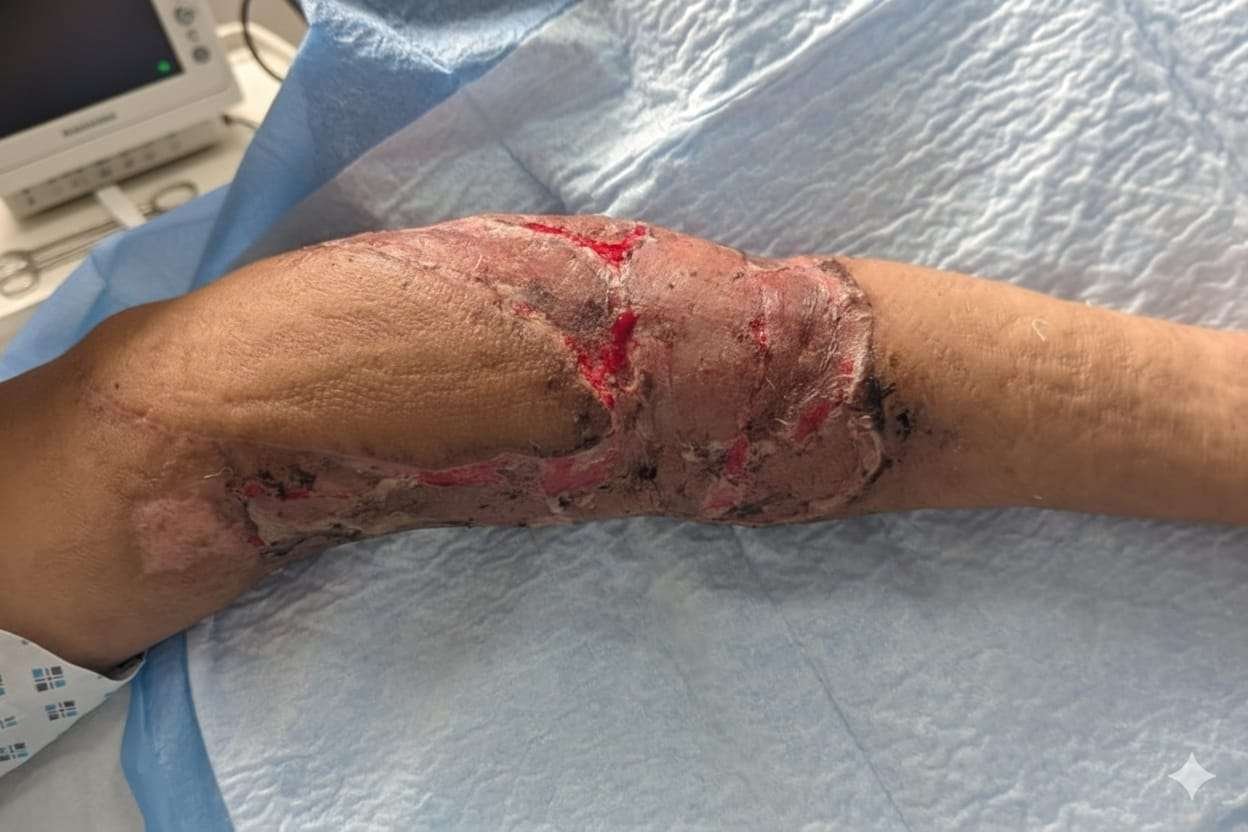
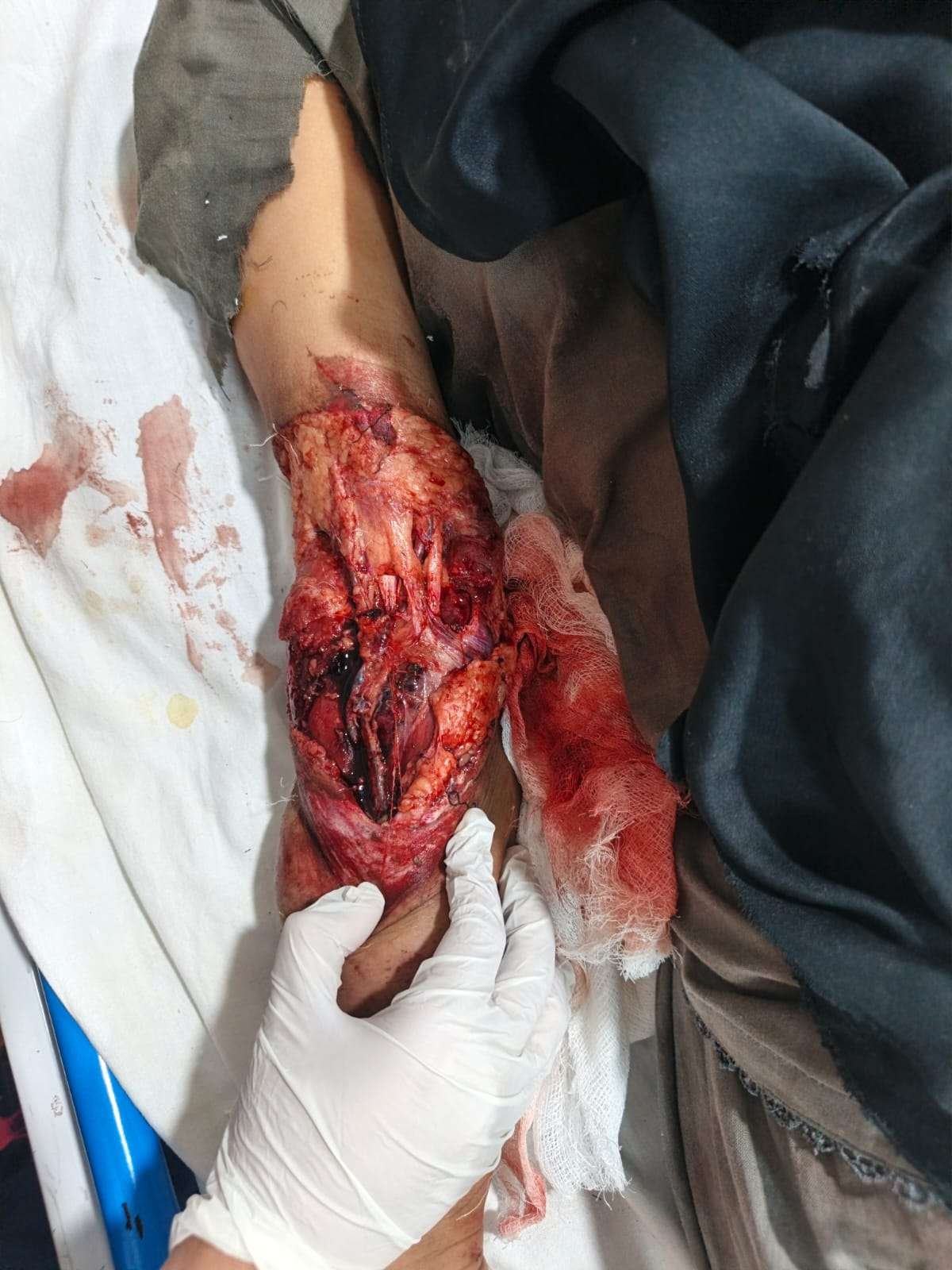
Before and After
Patient examination
Examination of the right upper limb revealed extensive soft tissue loss involving the distal arm,elbow and proximal forearm, associated with a circumferential degloving injury. The degloved skin flap extended proximally to the mid-arm and posteriorly involved the elbow region, while distally it extended to the mid-forearm. The biceps tendon, median nerve, and brachial artery were exposed. Sensory and motor examination was limited due to severe pain; however, no gross neurological deficit was appreciable. Radial and ulnar artery pulses were not palpable, and the limb was relatively cold compared to the contralateral side. Capillary refill was preserved, and pinprick testing over the fingers produced bright red bleeding, suggesting maintained distal perfusion.
Pre-operative considerations
1.Preparation of the Recipient Site
Plain radiographs of the upper limb demonstrated no bony injury. Computed tomography angiography revealed thrombosis of the brachial artery with absent flow, along with a segmental defect of the radial artery. Despite this, distal hand perfusion was maintained via collateral circulation. Given the concern for possible micro-intimal injury distal to the trauma zone, the vascular surgery team opted for close observation with systemic anticoagulation using weight-adjusted heparin therapy. After overnight monitoring, the patient was shifted to the operating theatre the following morning for definitive surgical management.
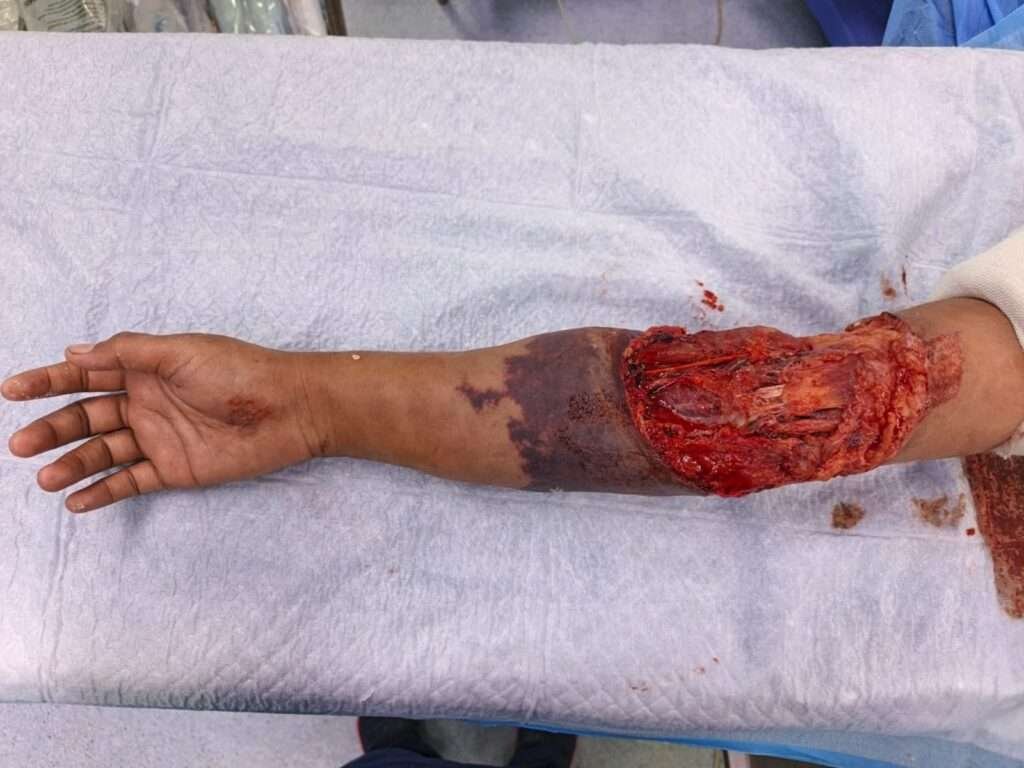
Post debridement
Under general anesthesia, thorough surgical debridement of devitalized tissue was performed
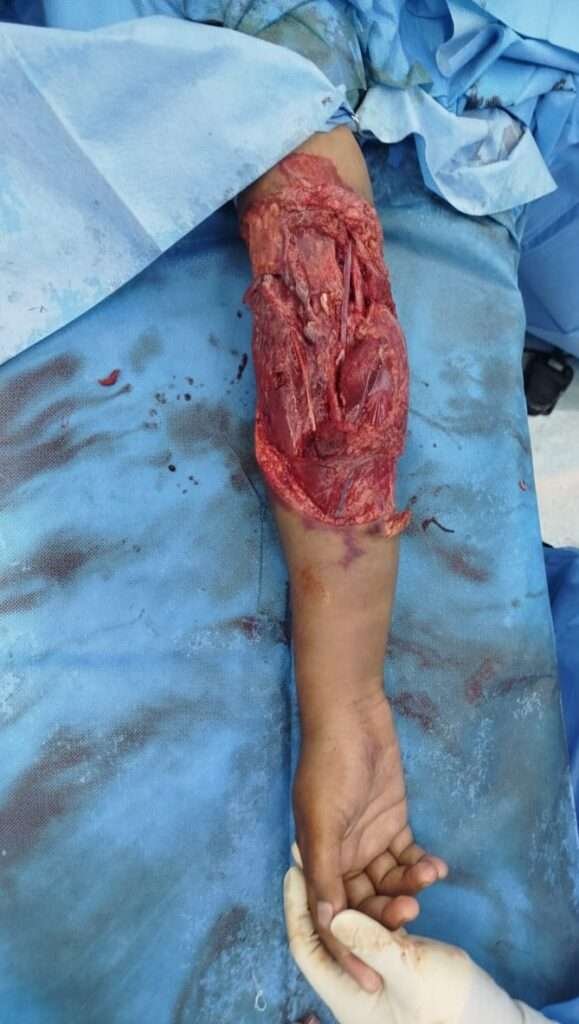
Vascular recontruction of brachial artery
The vascular surgery team reconstructed the brachial artery using an approximately 8-cm reverse great saphenous vein graft, restoring arterial continuity. Exploration of the median and ulnar nerves revealed them to be intact.
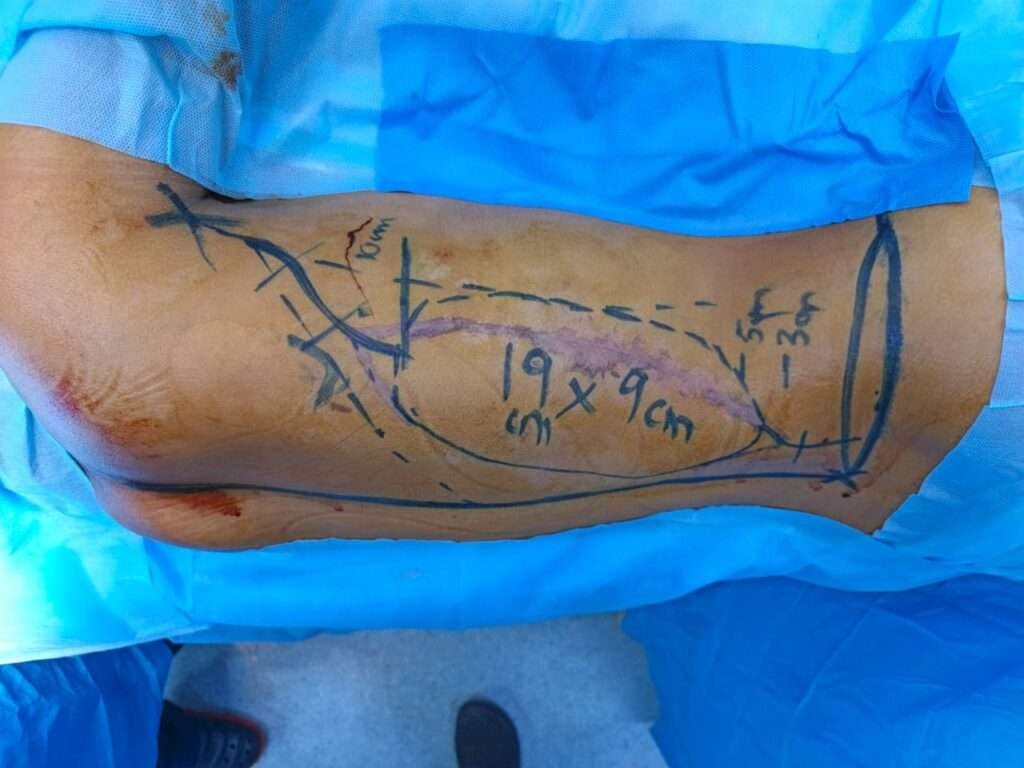
Marking of Latissimus dorsi flap
A myocutaneous latissimus dorsi flap measuring approximately 19 × 9 cm was designed on the ipsilateral side. Distally, the skin paddle was extended till 4 cmabove the posterior superior iliac crest to maximize coverage.
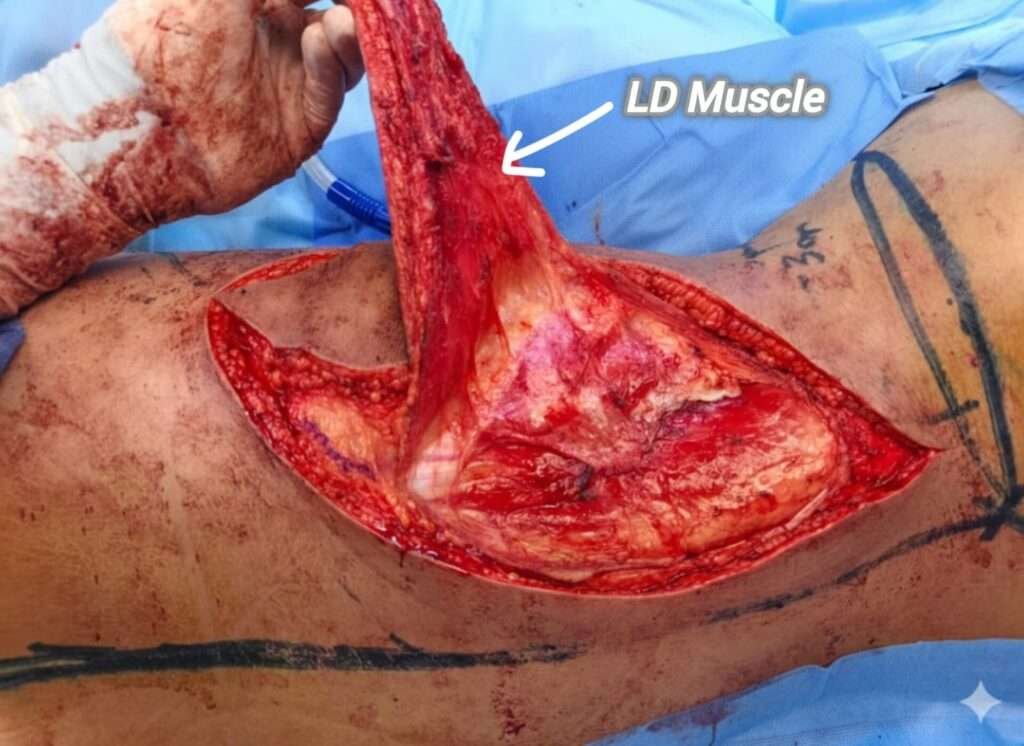
dissection
The flap was elevated in a standard fashion
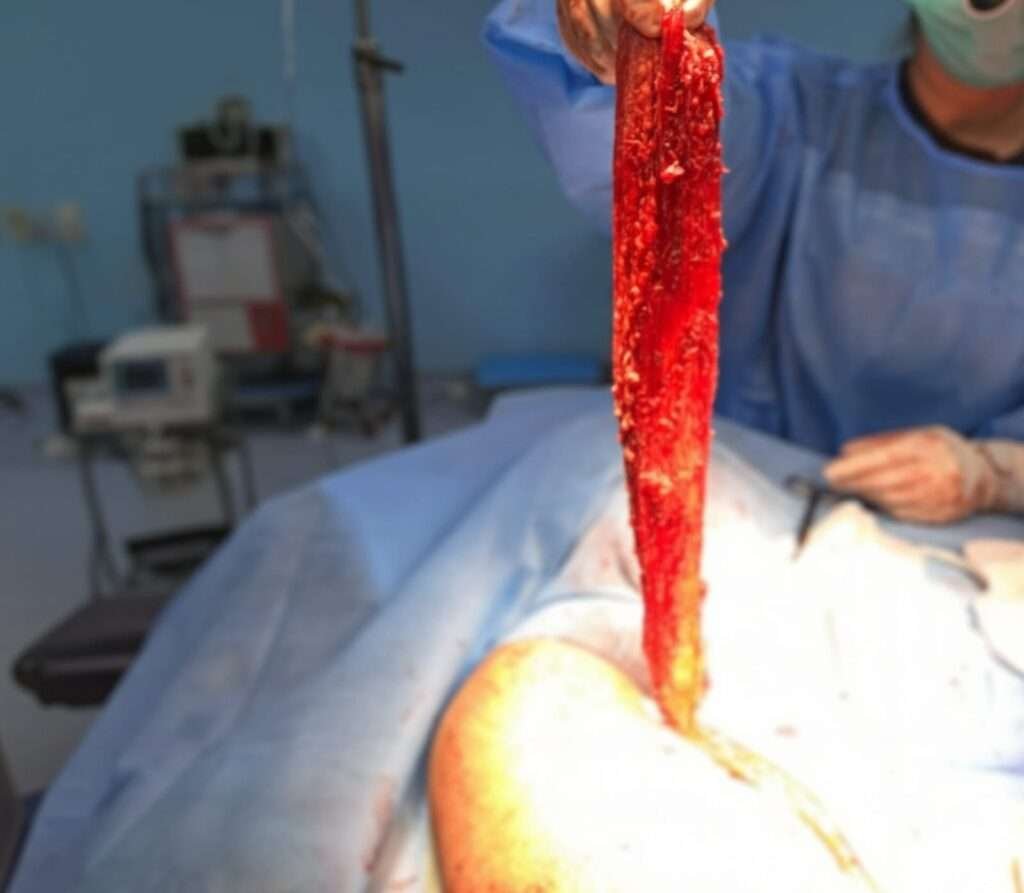
dissection of pedicle
Dissection carried out up to the thoracodorsal pedicle to increase the arc of rotation.
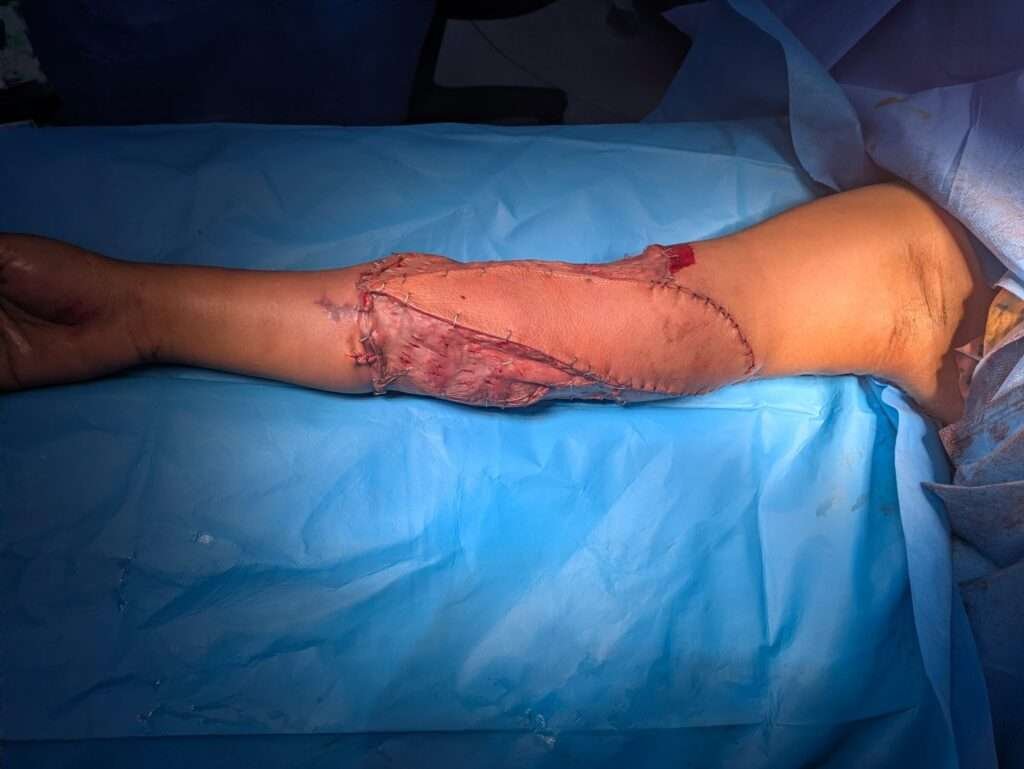
immediate post op image
The flap was tunneled through the axillary region and inset to cover the exposed neurovascular structures and elbow joint. Surrounding areas were resurfaced with split-thickness skin grafts
Pearls
The latissimus dorsi flap provides reliable, well-vascularized tissue for complex traumatic upper limb reconstruction.
– Harvesting the flap outside the zone of injury reduces the risk of flap-related vascular complications.
– This technique allows coverage of exposed vital structures without the need for microsurgical anastomosis in selected cases.
– Donor-site morbidity is minimal, particularly in young patients.
Pitfalls
Post-operative plan
The postoperative course was largely uneventful. A minor complication in the form of partial skin graft loss was observed, which was managed conservatively with wound cultures, targeted antibiotic therapy, and regular dressings. The affected area was subsequently regrafted with satisfactory take.
Follow-Up
At three months postoperatively, the patient remained under regular follow-up. The flap was healthy with stable coverage, and there was no evidence of infection or breakdown. The patient achieved excellent functional recovery of the limb with a good aesthetic outcome and minimal donor-site morbidity.