Keywords: Squamous cell carcinoma; finger amputation; volar flap; local reconstruction; traction neurectomy; hand surgery.
Authors: Claes Hannibal Killerich and Nikolaj Warming. Department of Plastic & Breast surgery, Aarhus University Hospital, Denmark
Abstract
A 93-year-old woman presented with a chronic non-healing dorsal finger wound initially diagnosed as actinic keratosis. Repeat biopsy revealed invasive squamous cell carcinoma with joint and bone involvement. Due to the extent of invasion, distal amputation of the third finger was required. Reconstruction was performed using a volar “toilet seat” flap under digital nerve block to minimize surgical burden. The procedure achieved clear margins, preserved stump length, and avoided donor-site morbidity. This case highlights the importance of early re-biopsy of non-healing lesions and adapting surgical strategy to patient age, function, and comorbidity.
Patient medical history
A 93-year-old woman presented with a wound on the dorsal aspect of the proximal phalanx of the left third finger. A primary biopsy revealed actinic keratosis, and the lesion was treated several times with curettage and electrodesiccation by a private dermatologist. Despite repeated treatments under professional supervision, the wound failed to heal.Due to the persistent non-healing nature of the lesion, a repeat biopsy was performed, confirming the diagnosis of squamous cell carcinoma (SCC). The patient was referred to the Department of Plastic Surgery, Aalborg University Hospital, where a primary excision was performed with a 7 mm surgical margin. Histopathological examination demonstrated invasive tumor growth involving both joint and bone. The defect was subsequently reconstructed using a full-thickness skin graft.
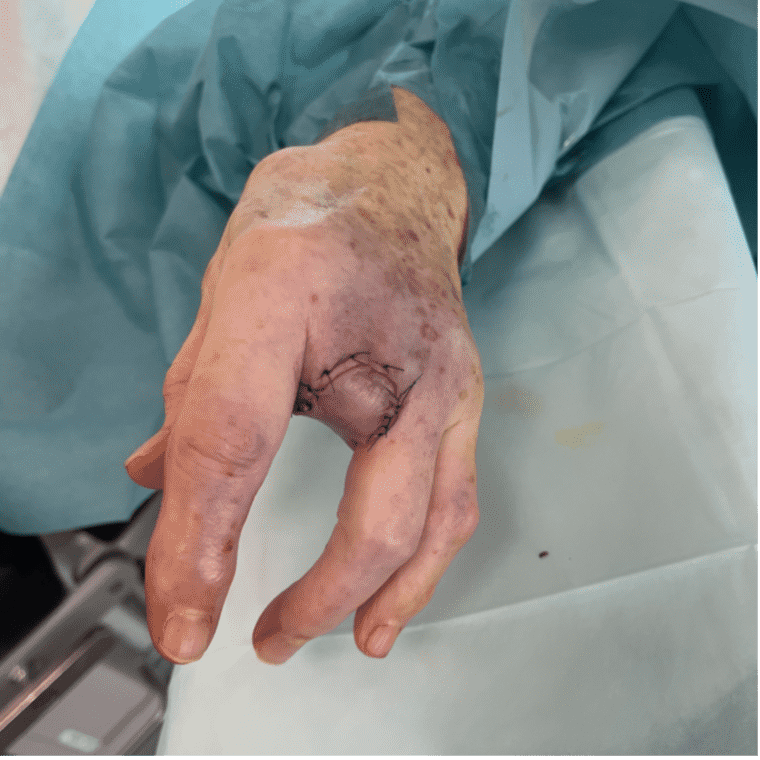
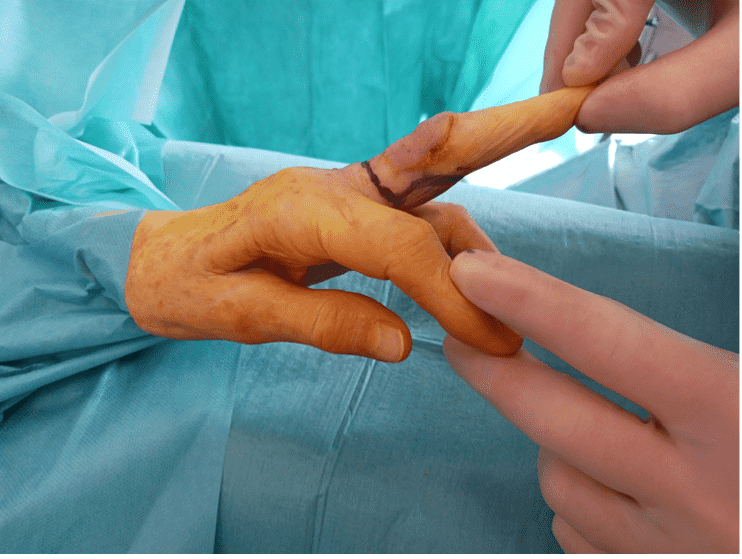
Before and After
Patient examination
The left third finger showed a healed full-thickness skin graft on the dorsal aspect of the proximal phalanx, covering the proximal interphalangeal (PIP) joint. There was no visible residual tumor, and no palpable lymphadenopathy in the left cubital fossa or axillary region.
Pre-operative considerations
The patient expressed a wish for the least invasive surgical approach possible, while ensuring complete tumor excision with clear margins. However, due to the invasive growth pattern of the squamous cell carcinoma (SCC), amputation of the finger was ultimately unavoidable. Alternative reconstructive options for dorsal finger defects, such as the Quaba flap or propeller flap, were therefore not feasible in this case.
Amputation at the most distal level that allows for clear oncologic margins is considered the gold standard in finger amputation for malignancy. This approach preserves maximum finger length and function, maintaining as much hand utility as possible (1).
In this case, the primary tumor was located on the dorsal aspect of the proximal phalanx, which allowed the volar soft tissue of the finger to be used for reconstruction following excision.
Excision of the flexor tendons and the neurovascular bundle as proximally as possible, enabling these structures to retract into healthy tissue. This technique helps to prevent adhesion formation, functional impairment, and painful neuroma development (2–3).
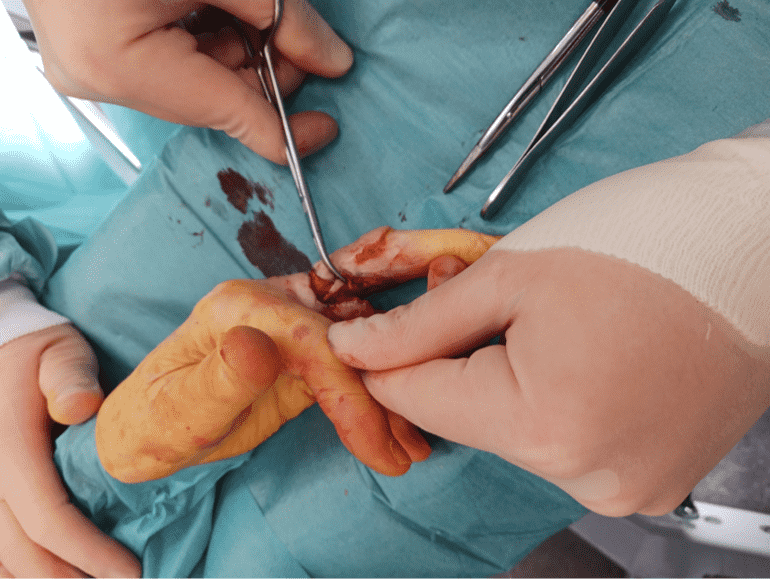
Excision and dissection of the digital nerve bundles
The finger was excised with a 5 mm safety margin. Dissection of the digital nerve bundles allowed for bilateral traction neurectomy, enabling the nerve ends to retract proximally into healthy tissue.
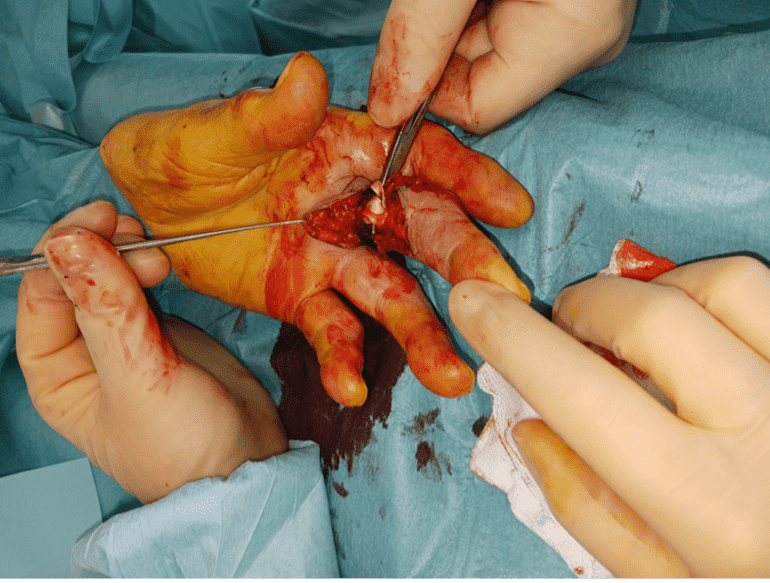
Dissection of the flexor tendons
Dissection of the flexor tendons prior to proximal tenotomy.
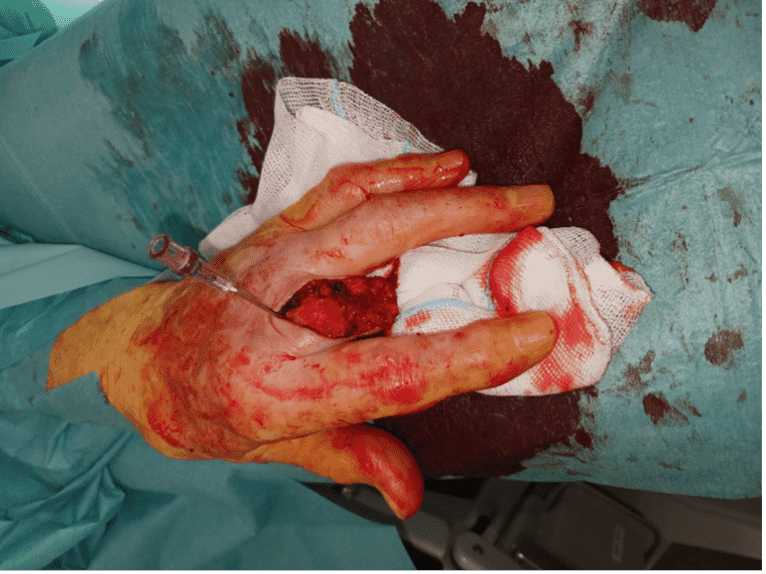
Amputation of the third finger
Amputation of the finger was performed distal to the metacarpophalangeal (MCP) joint, exposing the remaining base of the proximal phalanx along with the adjacent soft tissues. A needle was placed in the MCP joint to visualize the length of the preserved finger stump. The bony edges were smoothed with a rongeur.

The volar “toilet seat” flap
The volar “toilet seat” flap sutured into the defect using interrupted flap sutures
Pearls
The finger was amputated using digital nerve block of the third finger, and reconstruction was performed using adjacent soft tissue to minimalize the surgical load on the patient.
-tMinimal invasive procedure, avoiding general anesthesia.
-tLocal reconstruction using adjacent tissue reduces operative time, donor-site morbidity, and postoperative recovery burden — all important considerations in geriatric patients
-tBilateral traction neurectomy of digital nerves can prevent painful neuromas and improve postoperative comfort and function.
Pitfalls
Although traction neurectomy was used in this case to allow the nerve bundles to retract proximally into healthy tissue, this technique often results in neuroma formation when compared with newer, more refined methods such as:
-tIntraneural fascicular coaptation
-tDirect end-to-end neurorrhaphy of an adjacent distal nerve (3).
The patient was 93 years old and resided in a nursing home, receiving daily assistance with activities of living. Given her age and limited functional demands, a simplified, low-burden procedure was chosen to minimize surgical trauma while ensuring oncologic safety.
For a younger and more functionally active patient, particularly one dependent on hand grip strength, a different surgical strategy would have been more appropriate.
-tA ray amputation represents a more extensive procedure but offers better functional alignment and a superior cosmetic outcome for the hand.
-tThe gap created by removal of a central digit, especially the middle or ring finger, can significantly compromise hand function, leading to weakened grip strength and difficulty manipulating small objects due to malalignment (4).
Post-operative plan
Removal of flap sutures seven days postoperatively.
References
1. Reconstruction After Wide Excision of Primary Cutaneous Melanomas: Part IIu002du002dthe Extremities. Moncrieff MD, Thompson JF, Quinn MJ, Stretch JR. The Lancet. Oncology. 2009;10(8):810-5. doi:10.1016/S1470-2045(09)70121-4.
2. Treatment of tendons in finger amputations and description of a new instrument. Webster, George V. Surgery, Volume 17, Issue 1, 102 – 108
3. Scott BB, Winograd JM, Redmond RW. Surgical Approaches for Prevention of Neuroma at Time of Peripheral Nerve Injury. Front Surg. 2022 Jun 27;9:819608. doi: 10.3389/fsurg.2022.819608. PMID: 35832494; PMCID: PMC9271873.
4. Calderazzi F, Menozzi M, Nosenzo A, Galavotti C, Pogliacomi F, Ceccarelli F. Single ray amputation in traumatic injury of the hand: review of literature. Acta Biomed. 2018 Oct 1;90(1-S):14-23. doi: 10.23750/abm.v90i1-S.7677. PMID: 30714994; PMCID: PMC6503410.