Keywords: Gorlin-Goltz Syndrome, Recurrent Basal Cell Carcinoma, Radial Forearm Free Flap, Hard Palate Graft, Oncology, Plastic Surgery, Ophthalmology, Dermatology, Complex Eyelid Reconstruction
Authors: Miss Ketki Kaushal & Mr Oliver Bassett. James Cook University Hospital, Middlesbrough, England, United Kingdom.
Abstract
Gorlin-Goltz syndrome, also known as Nevoid Basal Cell Carcinoma Syndrome, is a rare autosomal dominant condition associated with pathogenic variants in the PTCH1 gene and dysregulation of the Hedgehog signaling pathway. A patient with longstanding disease presented with recurrent periocular basal cell carcinoma requiring Mohs excision, resulting in a large full-thickness lower eyelid defect. Reconstruction was performed using a hard palate graft for posterior lamella replacement and a radial forearm free flap with palmaris longus tendon sling for anterior lamella and structural support. Microvascular anastomosis to facial vessels was performed. This case highlights the reconstructive challenges of periocular defects in NBCCS and emphasises multidisciplinary management.
Patient medical history
A 59-year-old male with a longstanding history of Gorlin–Goltz syndrome (Nevoid Basal Cell Carcinoma Syndrome) diagnosed in 1997 has been under multidisciplinary care involving dermatology, plastic surgery, oncology, and ophthalmology for multiple recurrent basal cell carcinomas. His medical history includes hypertension, iron deficiency anaemia secondary to diverticulosis, chronic gastritis with duodenal ulcer disease, and melanoma in situ of the right knee excised in 2016. He has undergone numerous treatments for cutaneous malignancies including repeated surgical excisions, Mohs micrographic surgery, topical therapies (5-fluorouracil and imiquimod), and reconstructive procedures. In 2012 he underwent Mohs surgery for an infiltrative basal cell carcinoma of the left lower eyelid. Over subsequent years, multiple lesions were treated across the face, temples, ears, forearm, and calf. Since April 2016 he has been managed with the Hedgehog pathway inhibitor Vismodegib with intermittent dosing. He later developed cicatricial ectropion of the right lower eyelid following prior tumour excisions, previously managed with a Hughes flap. In 2024 he underwent Mohs excision for recurrent basal cell carcinoma of the right lower eyelid, leaving a large full-thickness defect that required complex reconstruction with a radial forearm free flap. He continues long-term surveillance due to ongoing risk of tumour recurrence.
Patient examination
Clinical examination revealed a large post-Mohs full-thickness defect of the right lower eyelid involving:
1) Loss of anterior and posterior lamella
2) Extension to the conjunctival fornix
3) Involvement of the lateral canthus
4) Partial involvement of the medial canthal ligament
Additional findings included:
1) Periocular scarring from previous excisions and reconstructive procedures
2) Evidence of prior eyelid reconstruction including Hughes flap
3) Multiple healed scars across the facial region consistent with repeated treatment of basal cell carcinomas
Ocular examination confirmed:
1) Adequate globe protection
2) No obvious corneal exposure or ulceration
3) Intact extra-ocular movements
4) Acceptable visual acuity
The defect involved greater than 75% of the lower eyelid, requiring reconstruction of both lamellae and restoration of eyelid suspension.
Pre-operative considerations
Key factors considered during operative planning included:
1. Defect size and lamellar loss – Large full-thickness eyelid defects require separate reconstruction of anterior and posterior lamellae.
2. Previous surgery and scarring – Prior procedures limited local reconstructive options and increased the need for vascularised tissue transfer.
3. Structural support – Loss of tarsus and canthal support required tendon-based suspension to prevent postoperative ectropion.
4. Oncological clearance – Complete tumour removal using Mohs micrographic surgery was essential before reconstruction.
5. Donor site suitability – The radial forearm free flap was selected due to its: Thin pliable tissue, reliable vascular pedicle, ability to include palmaris longus tendon.
6. Multidisciplinary planning – Close collaboration between dermatology, oncology, ophthalmology, and plastic surgery teams was required.
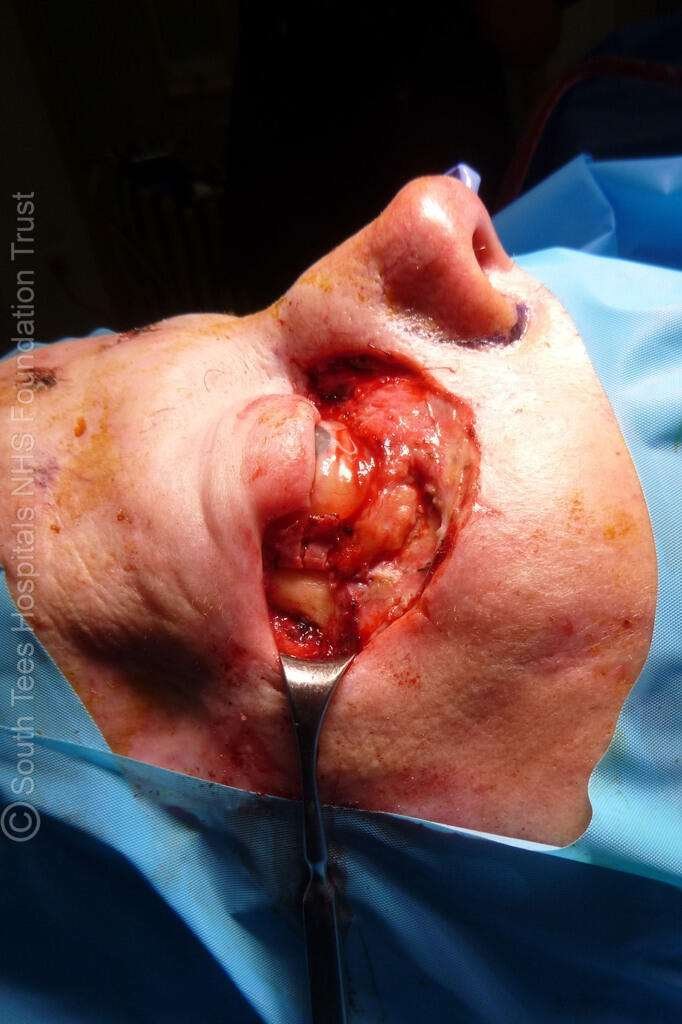
Defect of The Right Lower Eyelid After Debridement.
The defect includes loss of both the anterior and posterior lamellae, with involvement of the lateral canthus and medial canthal ligament, and extends to the conjunctival fornix. After confirmation of clear margins, the wound was debrided and margins freshened, removing devitalised tissue and creating a well-vascularised wound bed with exposed conjunctiva and periocular tissues, ready for definitive reconstruction.
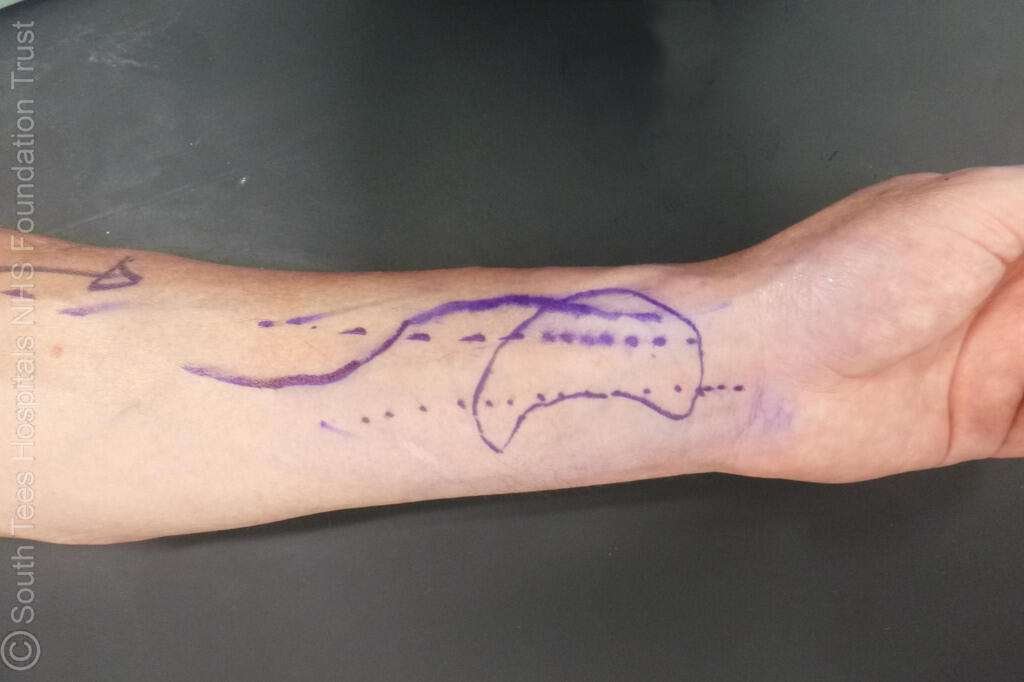
Preoperative Planning and Marking for Radial Forearm Free Flap Harvest
A radial forearm free flap was designed over the radial artery territory on the volar forearm, with the skin paddle tailored to the size of the anterior lamellar defect. The radial artery and venae comitantes were dissected to obtain an adequate pedicle for microvascular anastomosis.
The palmaris longus tendon was identified and harvested with the flap to be used as a suspensory sling for eyelid support, providing structural stability similar to the tarsoligamentous system.
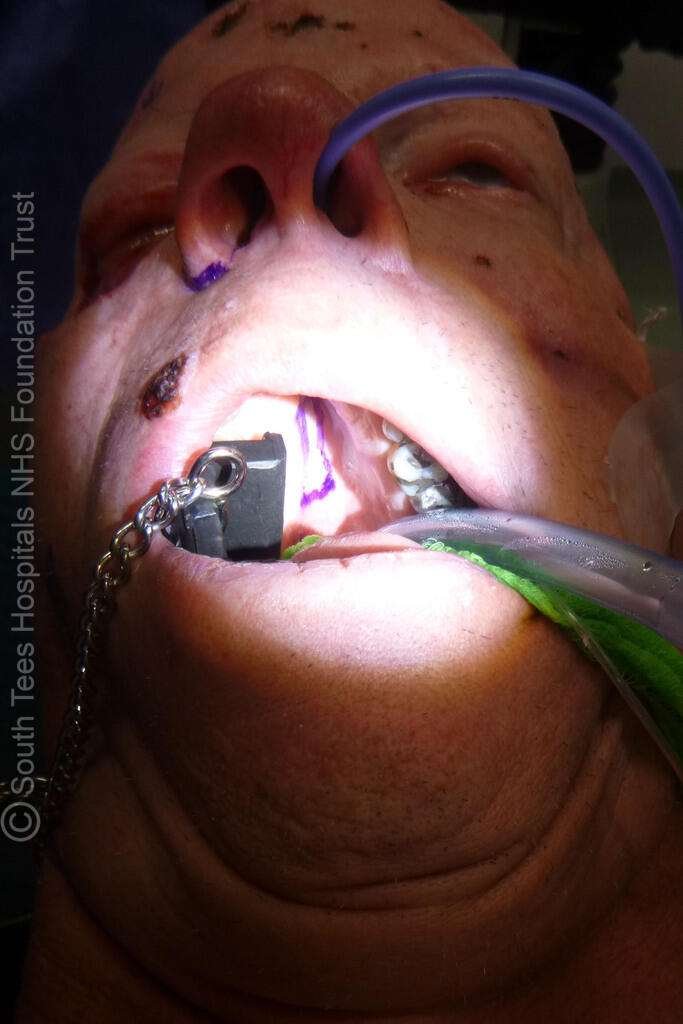
Pre-harvest Marking of The Hard Palate
For this complex defect, a composite reconstruction was planned:
Posterior lamella: harvested hard palate graft to provide structural support and mucosal lining.
Anterior lamella: radial forearm free flap for skin coverage.
Eyelid support: palmaris longus tendon sling integrated into the flap for dynamic support.
Pre-harvest marking of the hard palate is critical to define graft dimensions while preserving the mucoperiosteum and avoiding injury to the greater palatine artery. The flap and tendon dimensions are calculated to match the defect and ensure proper eyelid contour and function post-reconstruction.
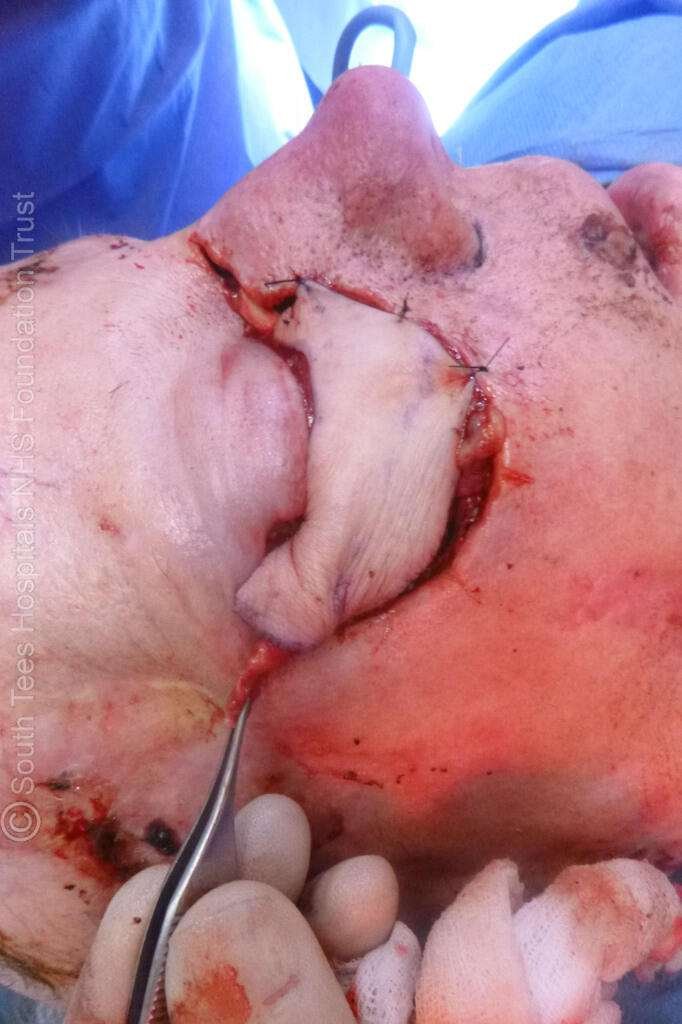
Inset Of Radial Forearm Free Flap Into The Defect
The radial forearm free flap was inset into the periocular defect to reconstruct the anterior lamella and provide soft-tissue coverage of the lower eyelid. The flap was carefully contoured to match the shape and size of the defect and secured to the surrounding eyelid margins using fine interrupted sutures (5-0 Monocryl and 5-0 Ethilon) to achieve precise alignment.
The palmaris longus tendon sling was positioned to support the reconstructed eyelid and was anchored to the periosteum of the medial and lateral orbital rim using 5-0 Vicryl, restoring eyelid suspension and maintaining appropriate lid position.
Following microvascular anastomosis of the radial artery to the facial artery and venous drainage to the facial vein using a 2.5-mm coupler, the flap demonstrated good perfusion, and the reconstruction was completed with layered closure.
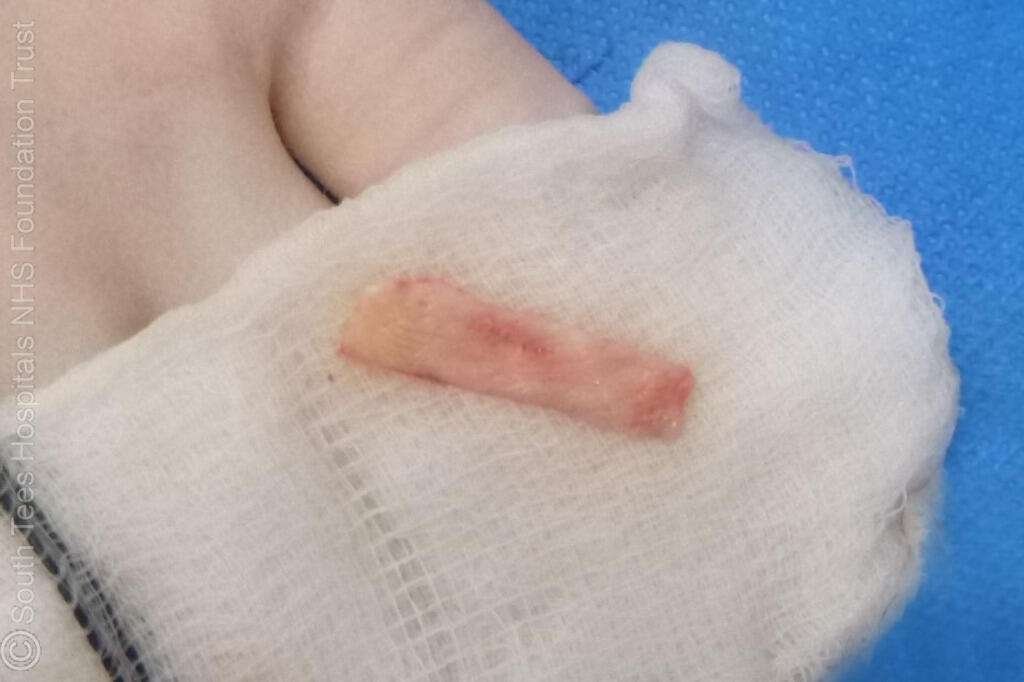
Harvested Hard Palate Graft
This intra-operative photograph demonstrates the harvested hard palate mucoperiosteal graft, obtained from the patient’s palate for use in eyelid reconstruction. The graft provides rigid mucosal tissue with structural support, making it well suited for posterior lamella reconstruction of the lower eyelid. After careful elevation from the hard palate with preservation of surrounding mucosa, the graft is trimmed to the required size and prepared for inset into the eyelid defect. The donor site is typically managed with haemostasis and allowed to heal by secondary intention or protected with a dressing plate.
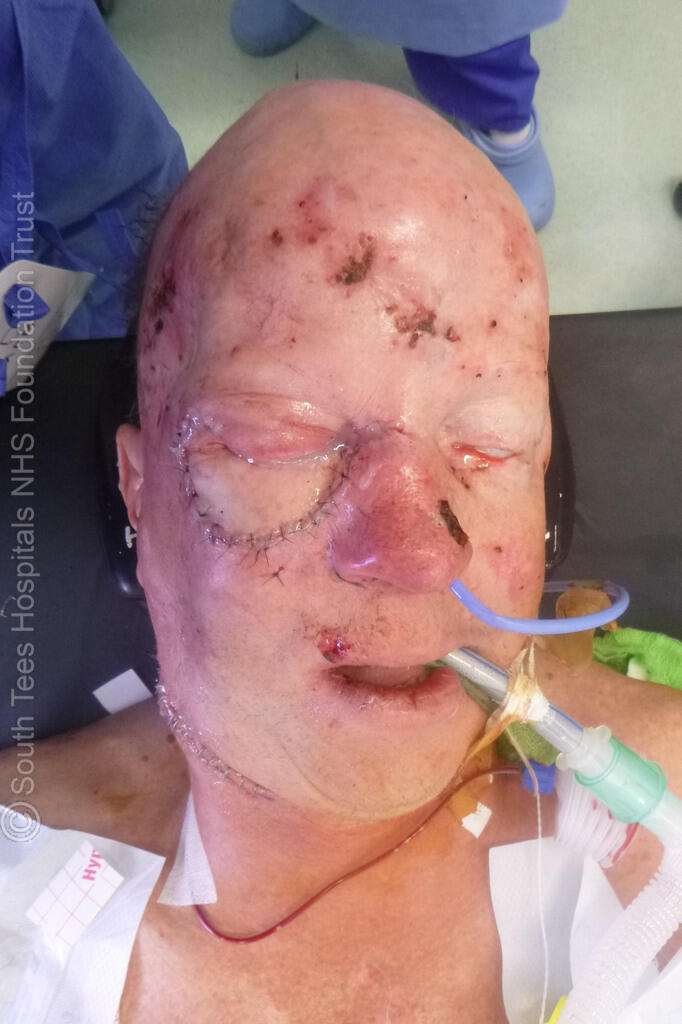
Immediate Post-operative Appearance Before Extubation
This intra-operative photograph demonstrates the final appearance following completion of the reconstruction of the right lower eyelid defect. The radial forearm free flap has been inset to recreate the anterior lamella, while the hard palate mucosal graft forms the posterior lamella. The palmaris longus tendon sling has been secured to the periosteum to provide structural eyelid support and restore lower eyelid suspension. The flap appears well perfused with satisfactory contour and alignment of the reconstructed eyelid. This image was taken at the end of the procedure prior to extubation.
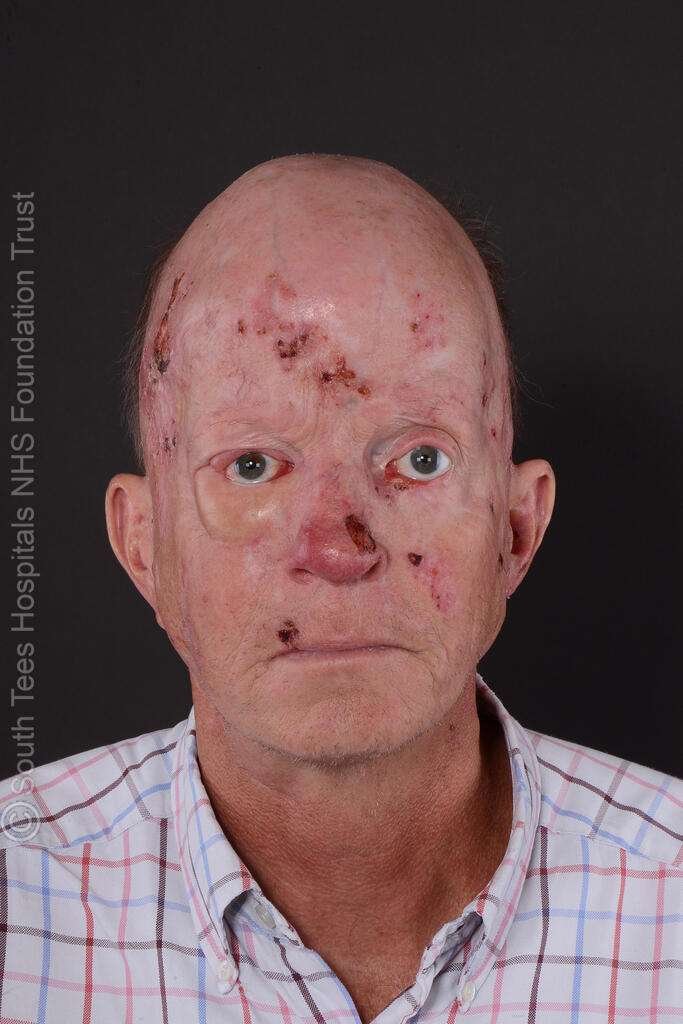
Post Op Photo
Clinic photo
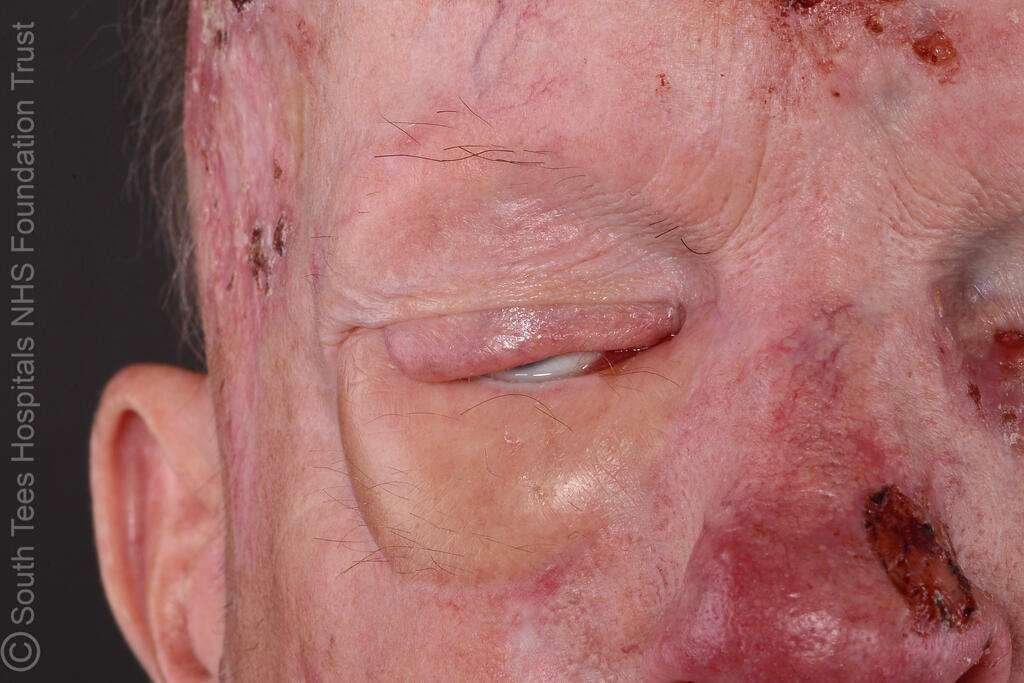
Post Op Photo
Clinic Photo – good eye closure
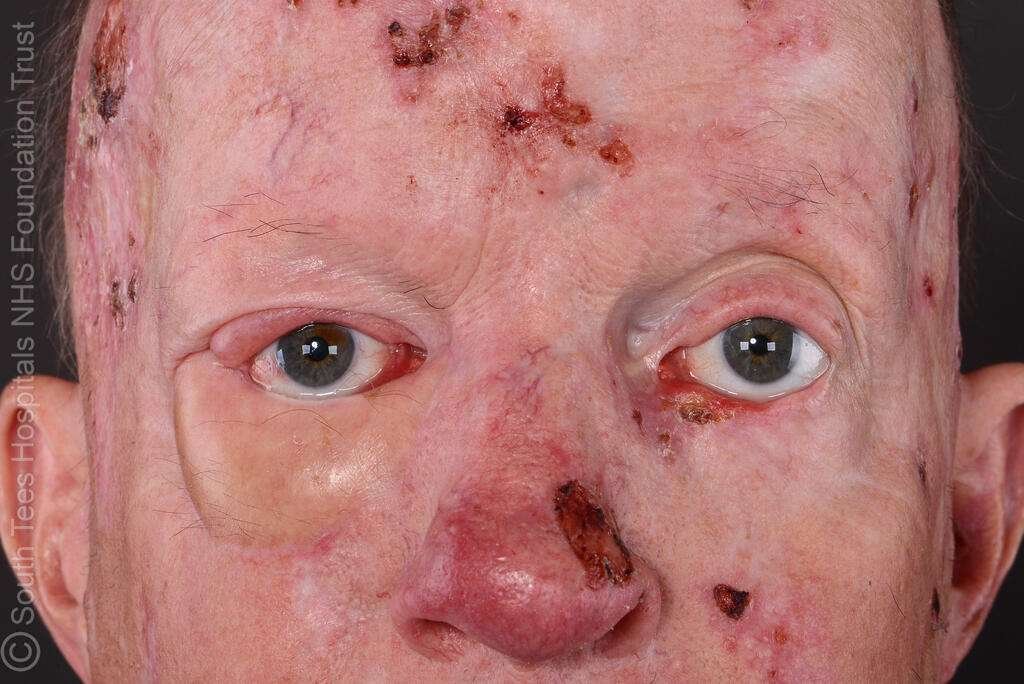
Clinic Photo
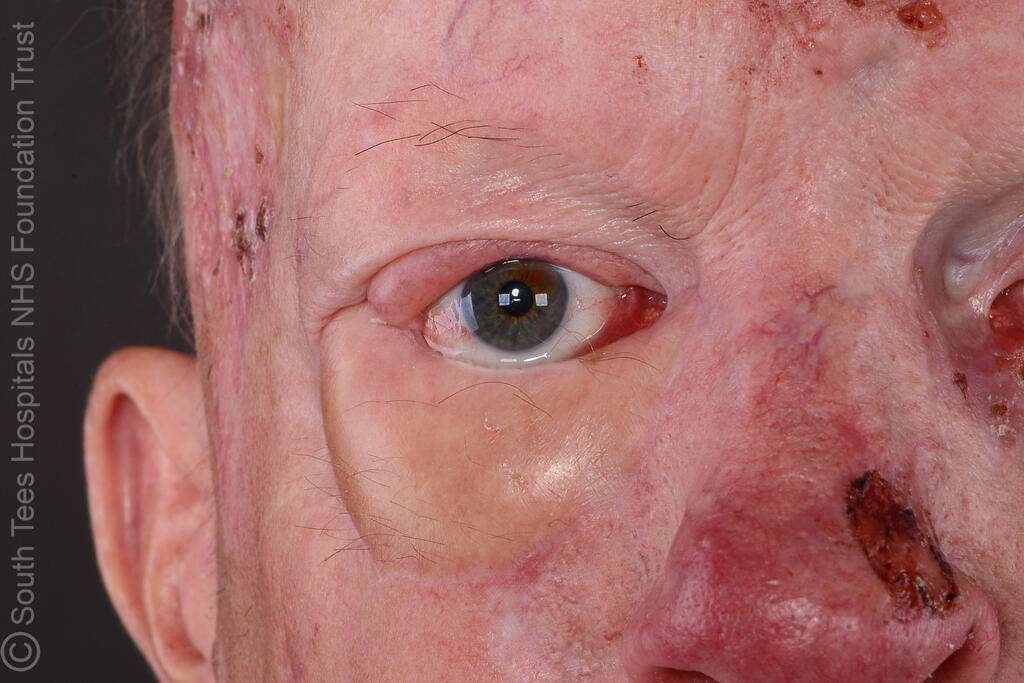
Clinic Photo
Pearls
Key technical lessons from this case include:
Always reconstruct eyelids using lamellar principles – anterior and posterior lamella must be restored separately.
Hard palate grafts provide excellent tarsal substitute due to their rigidity and mucosal lining.
Radial forearm free flaps are ideal for periocular reconstruction because of their thin, pliable tissue.
Palmaris longus tendon slings restore eyelid suspension, reducing the risk of postoperative ectropion.
Ensure precise flap inset and tension control to preserve eyelid contour and function.
Meticulous microvascular technique is essential for flap survival in delicate periocular reconstruction.
Pitfalls
Common challenges and complications include:
1) Ectropion due to inadequate eyelid suspension.
2) Flap bulkiness leading to poor eyelid contour.
3) Donor site morbidity following radial forearm flap harvest.
4) Corneal exposure and keratopathy if eyelid support is insufficient.
5) Compromised vascular anastomosis due to vessel scarring from prior surgery.
6) Recurrence of basal cell carcinoma, particularly in patients with Gorlin–Goltz syndrome.
Careful operative planning and multidisciplinary management are essential to minimise these risks.
Post-operative plan
Short-Term Management (First 1–2 Weeks):
1) Flap Monitoring – Regular free flap observations (colour, capillary refill, temperature, turgor, Doppler).
2) Haemodynamic Support – Maintain systolic BP >100 mmHg, monitor urine output and ensure adequate hydration.
3) Medications – LMWH 40 mg daily for VTE prophylaxis, broad-spectrum antibiotics for 5–7 days.
4) Ocular Care – Lubricating eye drops and ointment to prevent corneal exposure. Ophthalmology review if needed.
5) Wound Care – Topical antibiotic ointment to eyelid reconstruction site, monitor radial forearm donor site and skin graft.
6) Oral Donor Site Care – Soft diet and antiseptic mouth rinses following hard palate graft harvest.
Long-Term Management:
1) Functional Assessment
2) Regular review of eyelid position, lid closure, and ocular protection.
3) Scar and Flap Monitoring – Assess flap contour, scar maturation, and need for revision procedures.
4) Donor Site Follow-up – Monitor radial forearm donor site healing and function.
5) Oncological Surveillance – Lifelong dermatologic follow-up due to risk of recurrent BCCs in Gorlin–Goltz syndrome.
6) Multidisciplinary Care – Ongoing follow-up with plastic surgery, dermatology, oncology, and ophthalmology.