Keywords: Nipple reconstruction, plastic surgery, DIEP flap, C-V flap, Tennessee flap
Authors: Alaa Jady, MD, Pia Cajsa Leth Andersen, MD. Copenhagen University Hospital, Rigshospitalet. Denmark.
Abstract
Nipple reconstruction is an important final step in breast reconstruction after mastectomy. This case describes a 42-year-old woman with prior right-sided breast cancer who underwent successful breast reconstruction using a DIEP flap followed by nipple reconstruction with the Tennessee technique. Pre-operative planning focused on achieving symmetry through detailed bilateral measurements and nipple–areola sizing. The procedure involved designing a flap with two arms and a rounded head, careful preservation of the subdermal plexus, and staged suturing. Postoperative follow-up showed good healing, maintained nipple projection, and satisfactory symmetry three months after surgery.
Patient medical history
A 42-year-old woman with a known history of Hashimoto’s thyroiditis was diagnosed with right-sided breast cancer in June 2022. She received neoadjuvant therapy followed by a right-sided mastectomy in December 2022 and adjuvant radiotherapy. Following completion of these treatments, the patient was deemed cancer-free. In November 2024, she underwent uncomplicated right-sided breast reconstruction using a deep inferior epigastric perforator (DIEP) flap and a contralateral mastopexy for symmetry. Subsequently, right-sided nipple reconstruction was performed in December 2025.
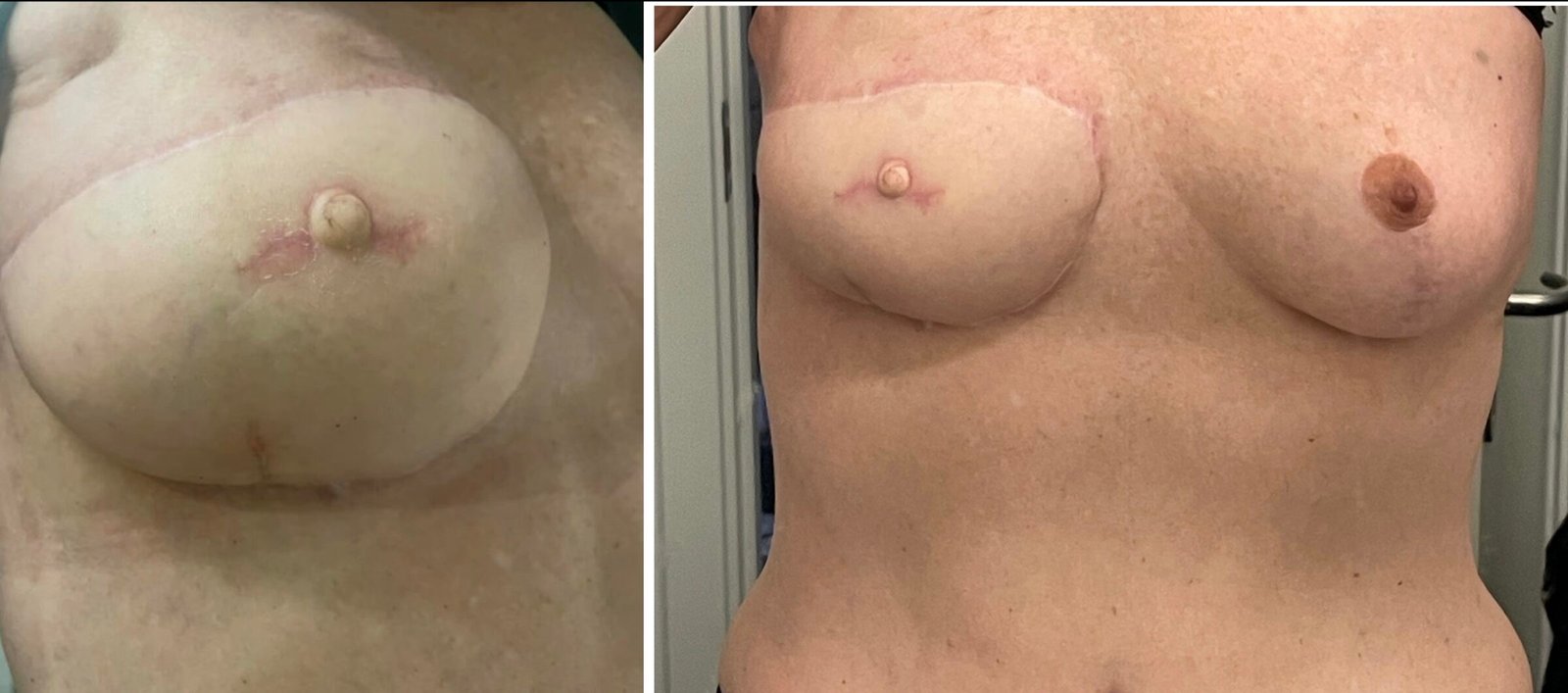

Before and After
Patient examination
Physical examination revealed well-healed scars on both breasts that appeared soft and symmetrical. At the site of the DIEP flap on the right breast, the nipple was absent.
Pre-operative considerations
Since the patient planned to undergo subsequent nipple–areola complex (NAC) tattooing following our reconstruction, a nipple reconstruction using the “Tennessee” technique was chosen.
To achieve symmetry, bilateral measurements were obtained with the patient in the upright position, including the distance from the nipple to the sternal notch, the inframammary fold, and the midline of the sternum, as well as the areolar diameter.
The size of the NAC on the right breast was also taken into consideration. Preoperatively, NAC prostheses/stickers of varying sizes were applied to the left breast to ensure bilateral symmetry, and a medium-sized NAC was ultimately selected for our patient. This process ensured that the reconstructed nipple on the left breast was positioned at the same vertical level as the nipple on the right breast (Jalini et al., 2017).

Step 1: pre-operative nipple design
The basic concept of the “Tennessee” nipple reconstruction is that the nipple design is composed of two ‘arms’ and one round ‘head’. The diameter of the head will be similar to that of the final nipple diameter, and the overall circumference of the two arms will approximate the circumference of the new nipple (Bermudez et al., 2025).
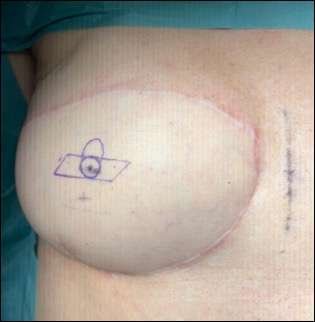
Step 2: pre-operative markings
The measurements for our patient’s nipple were as follows: each arm had a short side on 7 mm (green line on the illustration) and a long side at 12 mm (orange line on the illustration), while the circumference of the head was the same as the height as the nipple (blue line on the illustration). These markings are illustrated on the patient in the above picture.
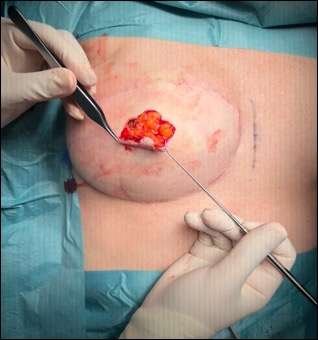
Step 3: incisions
Incisions are made to define the two arms and the head. Care should be taken not to divide the base of the flap or the attachment of the head to the vertical wall. The blood supply to this flap comes from the underlying subcutaneous tissue, and thus it is important to leave the subdermal plexus in those subcutaneous tissues intact.
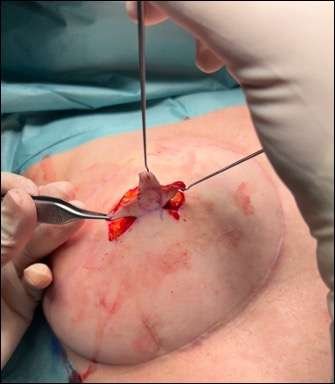
Step 4: flap mobilization
The two arms are then elevated from the underlying subcutaneous tissue (see picture 4). The subdermal plexus is left on these as well as some fatty tissue, depending on the requirements for the fullness of the nipple. The flaps are thinned more toward their periphery than centrally to avoid devascularizing the tip of the flaps.
The head is also thinned, and the subcutaneous tissue preserved in the central area of the proposed new nipple. This central tissue will provide blood supply as well as central bulk for the nipple.
The flap is gradually lifted by elevating the flap and releasing some of the tightness while preserving the blood supply to the base of the flap, which also supplies the two arms and the head flaps.
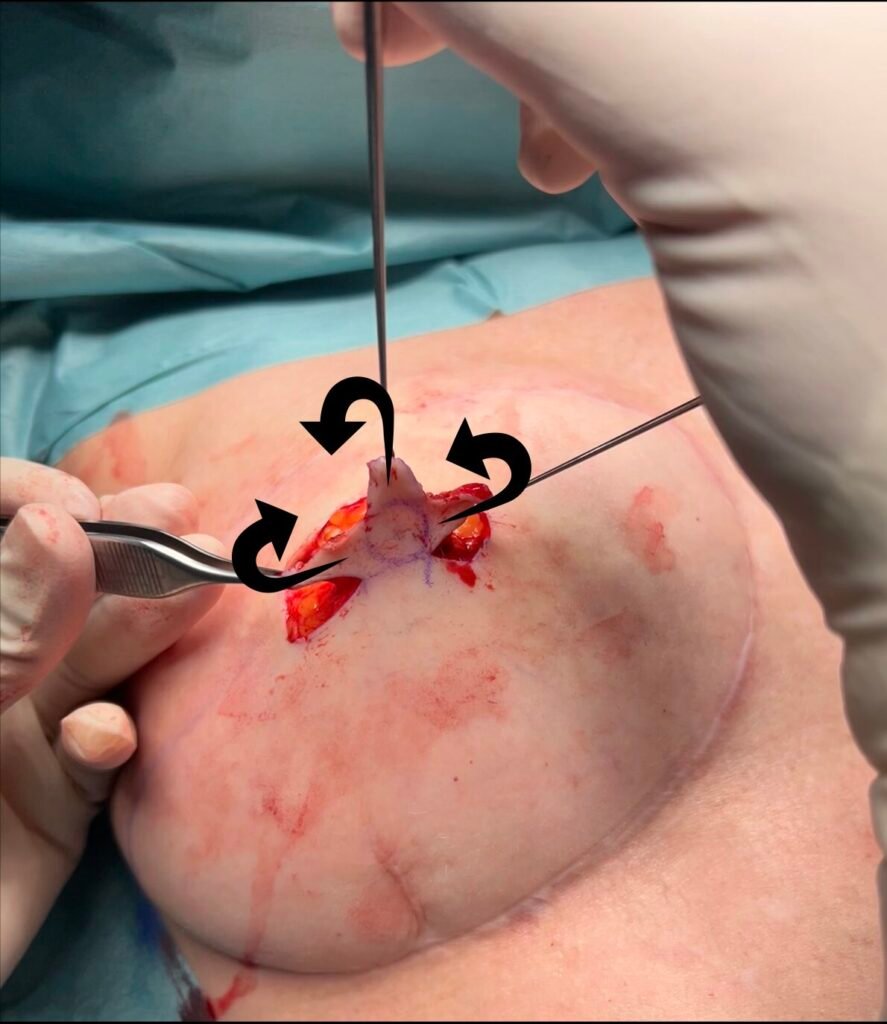
Step 5: suturing
The initial flap closure involves suturing the donor base of the head flap to the base of the arm flap on both sides with an absorbable suture. We used Vicryl 4-0 for inverted subcuticular stitches. This effectively closes the donor site and brings the site of the head flap in as a circle to define placement of the nipple reconstruction.
After the donor sites are closed, the two arm flaps and the head flap are trapped outside with a non-absorbable suture. We used Prolene 4-0 for simple interrupted stitches. When these flaps are positioned, it can be seen that the width of the arm flaps determines the vertical height of the nipple, and the head flap is the top of the nipple reconstruction.
The area was dressed with Jellonet, a donut-shaped foam dressing, and a large Tegaderm dressing.
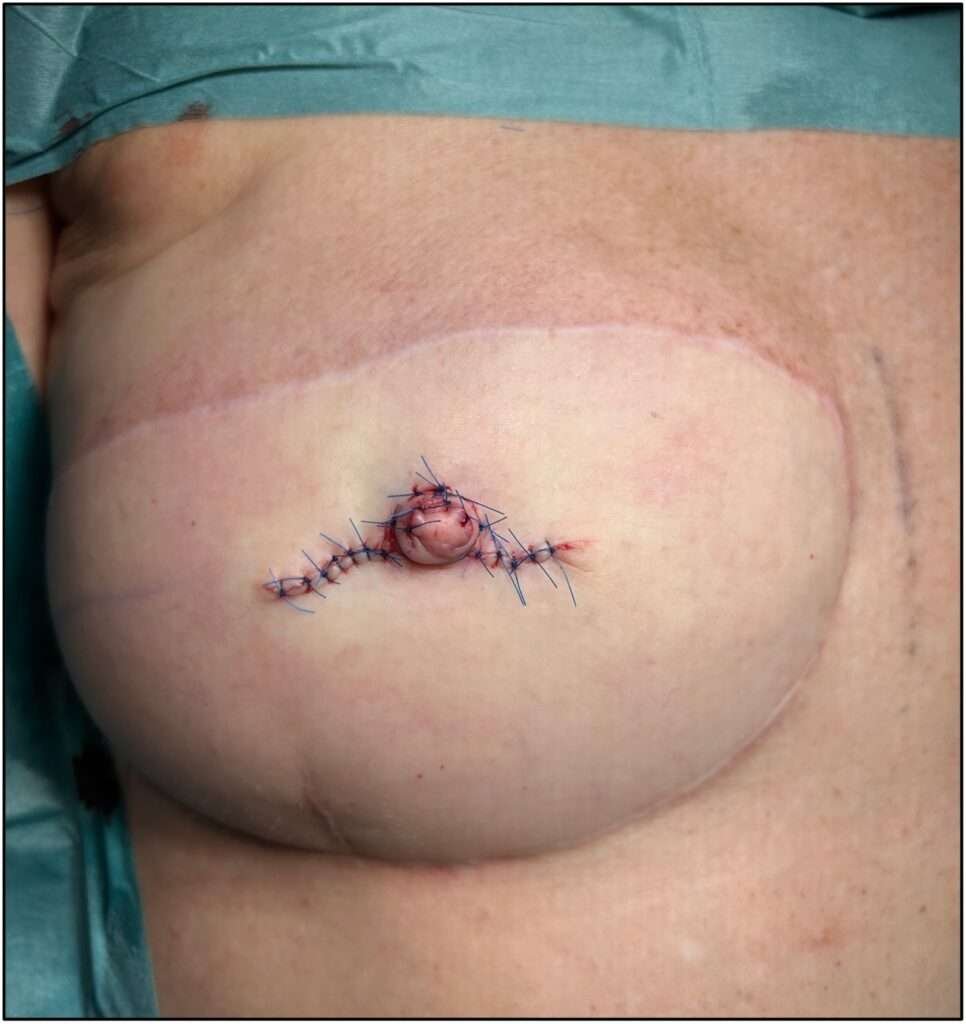
(continued step 5: suturing)
The immediate postoperative result is as seen on the picture.
Step 6: stitch removal
The patient returned to our clinic 14 days postoperatively for suture removal. The procedure was performed without complications; there were no signs of infection and the cicatrice appeared well healed. The patient additionally stated that she would independently seek a medical tattoo artist for NAC-tattooing.
Follow up
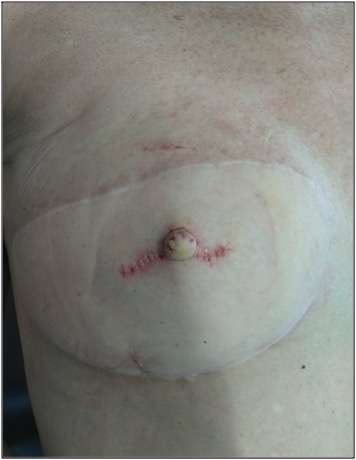
Patient sent in a picture of her breast as a 3 month follow up (see picture 8). Here can be seen a good nipple symmetry and projection.
Pearls
This flap is a versatile and reliable method for breast reconstruction. It uses local tissue and is most applicable and predictable after autologous tissue reconstructions with thicker subcutaneous tissues. The volume of the flap is dependent on the volume of the underlying subcutaneous tissues as well as the tension of the skin.
This reconstruction can easily be done under local anesthesia.
When deciding the placement of the flap, the appearance of the nipples while wearing clothing such as a shirt or bra is of primary importance for some patients, whereas for others, the appearance in the absence of clothing is more significant. We advise to involve the patient in the decision of the nipple placement.
Pitfalls
The limits of this procedure are most obvious in patients with a very tight implant-based breast reconstruction. In these cases, the sparse subcutaneous tissue, along with the tight skin, most often results in the new nipple significantly reducing height and ending up absent.
When designing the flap, it is important to avoid placing the base of the flap in close proximity to a scar, as adequate vascular supply must be ensured to maintain flap viability.
Post-operative plan
No indication for further follow up or surgery postoperatively.
References
Bermudez, U. S., Velázaquez, M. G. M., Sampayo, K. L. L., Tijerina, S. F. E., Rodríguez, J. E. T., Lopez, M. A. R., Graciano, E. P., u0026 Martinez, O. U. R. (2025). Modified C-V Flap for Nipple Reconstruction. Cureus, 17(3), e80256. https://doi.org/10.7759/cureus.80256
Jalini, L., Lund, J., u0026 Kurup, V. (2017). Nipple Reconstruction Using the C-V Flap Technique: Long-Term Outcomes and Patient Satisfaction. World Journal of Plastic Surgery, 6(1), 68. https://pmc.ncbi.nlm.nih.gov/articles/PMC5339612/