Keywords: Hemicorporectomy, Fillet flap, Spare-parts surgery, Sarcoma reconstruction, gluteal sarcoma, Complex pelvic reconstruction
Authors: Isha Joshi MD MBA, Zachary Erlichman MD, Nia Nikkhahmanesh MD, Christina Chopra MD, Jason Ganz MD Institution: Stony Brook University Hospital, Stony Brook, New York
Abstract
Background: Tissue from non-salvageable limbs may be used in reconstruction of complex defects and represent the principle of the “spare- parts” concept.[1] Fillet flaps advantages include soft tissue coverage of large defects, biocompatibility of an autologous donor, and donor tissue resembling native tissue due to proximity. Case: Fewer than 100 hemicorporectomies have been published in the literature.[2] We present the case of a 53-year-old male who underwent hemicorporectomy for recurrent gluteal sarcoma followed by reconstruction using a near-total thigh fillet flap. Conclusions: Fillet flaps provide soft-tissue coverage of large defects, biocompatible autologous tissue, and donor tissue resembling native anatomy.
Patient medical history
Primary Diagnosis: In 2015, the patient was diagnosed with a 15-cm high-grade (grade 3) spindle cell carcinoma thought to represent a fibrosarcoma with transformation to dermatofibrosarcoma protuberans, located superior to the buttock. The tumor was resected at an outside hospital (OSH) without perioperative complications. First Recurrence: In 2016, the patient presented to the OSH with recurrent mass in the tumor bed measuring 12.2 cm with erosion of lower coccyx, extension into posterior pelvis, and deviation of the anus. He underwent neoadjuvant radiation and systemic therapy. In 2017, he underwent tumor debulking and permanent diverting colostomy placement. After relocating to New York, he established care at our institution and subsequently underwent conversion of a loop colostomy to an end stoma with mucous fistula in 2020. Secondary Recurrence: In 2022, imaging demonstrated a recurrent tumor above the buttock. The patient underwent extensive oncologic resection including: abdominoperineal resection, sciatic nerve excision, and ischium excision by surgical oncology and orthopedic surgery. Plastic surgery reconstruction included a pedicled right vertical rectus abdominis muscle flap and a right vastus lateralis muscle flap. Following surgery, the patient’s functional status progressively declined from ambulating with a cane to becoming bedbound. Between 2022 and 2024, he developed chronic urinary retention requiring indwelling foley catheter and progressive back pain requiring cordotomy and midline myelotomy Tertiary recurrence: In 2025, imaging demonstrated a large recurrent mass measuring 18 × 16 cm. After multidisciplinary evaluation, the patient elected to proceed with curative resection via hemicorporectomy. Plastic surgery was consulted for definitive soft-tissue reconstruction.
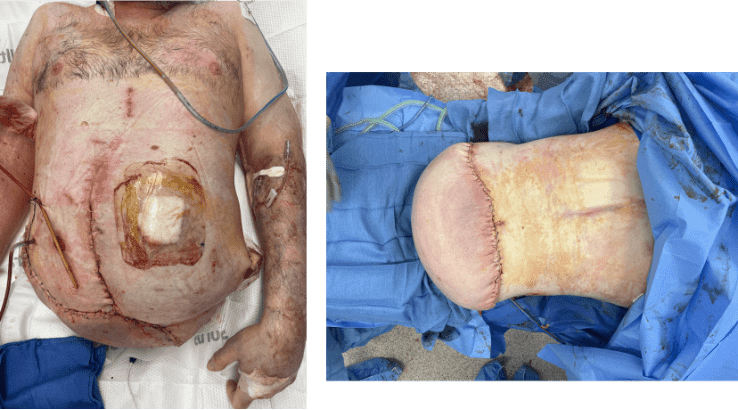
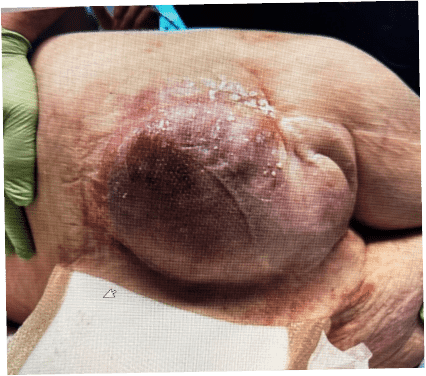
Before and After
Patient examination
At presentation, the patient was bedbound with severe functional limitations following prior surgeries and radiation therapy. Examination demonstrated a large recurrent gluteal mass involving previously reconstructed tissue. There existed significant radiation-associated fibrosis and chronic pressure injuries over the trochanteric and ischial regions. The patient was noted to have limited mobility with dependence on wheelchair and bed positioning. Given the extent of disease and compromised surrounding tissue, reconstruction using local or regional flaps alone was not feasible. A fillet flap using tissue from the non-salvageable lower extremity was therefore planned.
Pre-operative considerations
Multidisciplinary Planning. This operation required coordination among:
Surgical oncology
General Surgery
Orthopedic Surgery
Neuro- spine surgery
Plastic surgery
Anesthesia
Surgical ICU teams
Intraoperative Planning
Operative Timing.
The procedure was scheduled for 36 hours with an anticipated time of 20-30 hours. (Total operative time yielded 20 hours.)
Prone to Supine Positioning.
Typically, ligation of the inferior vena cava leads to engorgement of Batson’s plexus, which can significantly increase bleeding during spinal division. To minimize blood loss and neurogenic hypotension, the vertebral structures and spinal cord were transected early prior to major venous congestion.
Consideration of Prior Pressure Ulcers.
The patient had trochanteric and ischial pressure injuries, which limited the usable skin envelope of the thigh. Flap design therefore preserved viable skin while excluding compromised tissue.
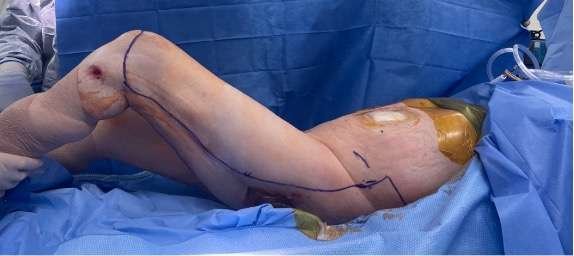
Step 1: Pre-Operative Markings
The flap was designed as a near-total fillet of thigh flap. The patient had a trochanteric and ischial pressure injury on his left leg posteriorly, which limited the use of the entire skin envelope, though the majority of the envelope was included with the flap. The longitudinal markings were made at the interval between the adductor magnus and biceps femoris while the lateral incision was made between the vastus lateralis and hamstrings.
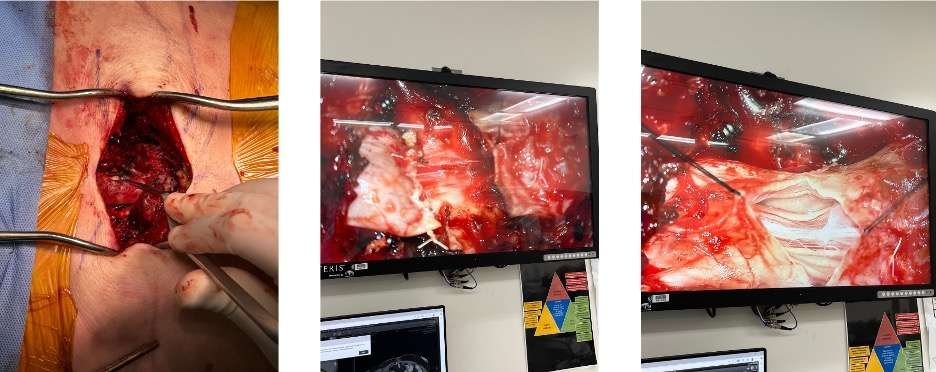
2: Posterior Approach and Cord Transection
A posterior to anterior approach was implemented with spinal surgery after marking the patient at the beginning of the case. Typically, after ligation of the inferior vena cava, Batson’s plexus becomes engorged, leading to a more challenging dissection and marked blood loss during division of the vertebral structures and spinal cord. Having experienced this problem in prior cases, a back-to-front approach was utilized with early division of the vertebral structures and spinal cord, pre-empting engorgement of Batson’s plexus, thus minimizing blood loss and neurogenic hypotension.
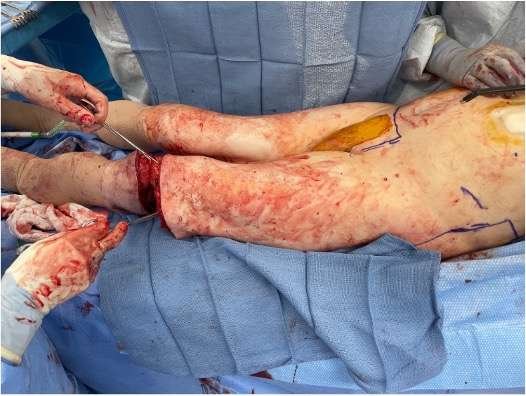
Distal Incisions and Vascular Identification
An incision was made just superior to the patella. After division of the quadriceps tendon, dissection proceeded distally to the femur. Medial dissection followed the interval between the adductor magnus and biceps femoris until the medial and lateral incisions were connected. The femoral artery entering the popliteal fossa was identified and controlled. The popliteal vessels were suture-ligated prior to transection.
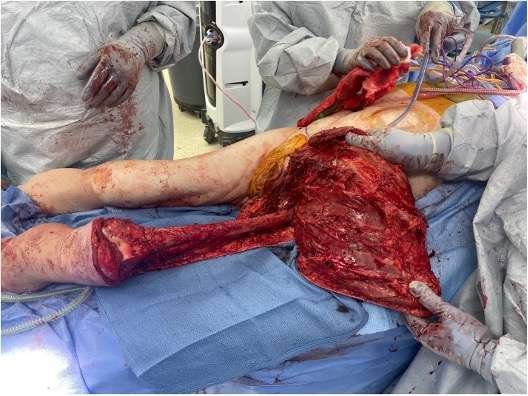
Muscle Dissection and Elevation
With the vascular pedicle identified, the flap was elevated while incorporating the adductor musculature for additional coverage. The muscle was dissected off the femur from all directions as the flap was elevated in the distal to proximal direction. Care was taken to maintain the integrity of the quadriceps muscles as well as the gracilis, sartorius, adductor longus and their vascular pedicles. The flap was then elevated up to the level of the iliac crest.
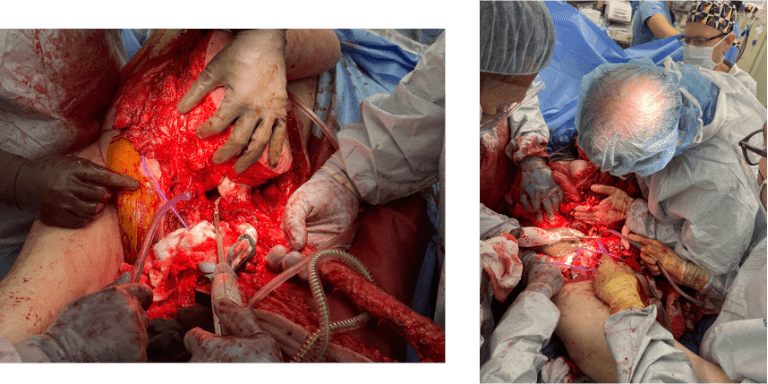
Pelvic Disarticulation
Orthopedic surgery completed the pelvic disarticulation. A midline abdominal incision was performed, and the common iliac vessels were transected using a vascular stapler. The tumor was dissected from the external iliac vessels, and the internal iliac artery was divided.
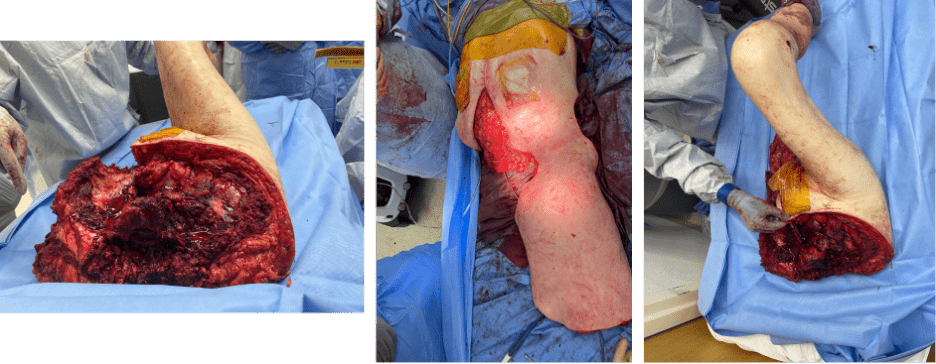
Completion of Posterior Dissection
The remaining posterior structures including psoas muscle, paraspinal muscles, and posterior soft tissue were divided, completing the hemicorporectomy specimen.
Postoperative Day 0
Early venous congestion of the flap was noted.
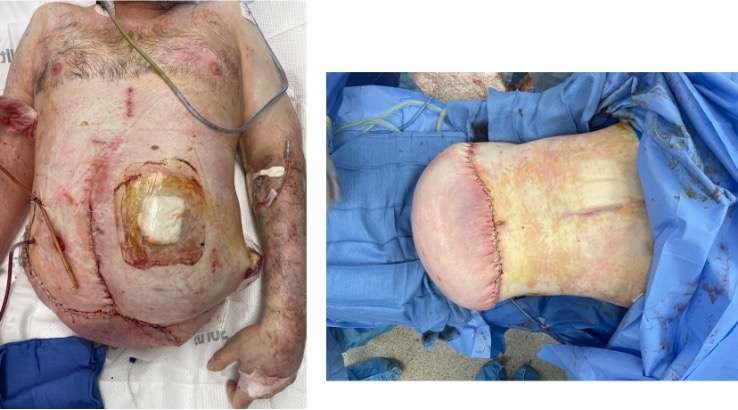
Postoperative Days 1–5
Leech therapy was used for approximately 5 days postoperatively when the flap was noted to be hyperemic and slightly tense. The team used a low threshold in deciding to initiate leech therapy given the significant change in habitus and somewhat unavoidable pressure to the flap. Gradual improvement of the hyperemia was noted over the course of the 5 days of leech therapy, with leeches aborted 24 hours after skin stability was noted.
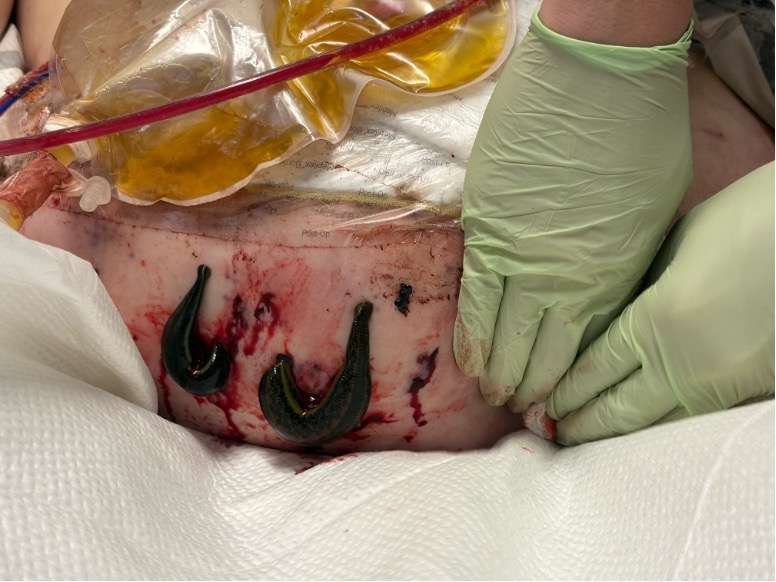
Postoperative Weeks 1-4
Patient underwent minor serial debridements intraoperatively to heal superficial dehiscences at the flap edges. Debridements were managed with wound vacs until good wound edge approximation was observed, at which point dressings were changed to mepilex. During this time the patient was downgraded from the Surgical ICU to the step down unit, transitioned to a pressure-offloading air mattress, and initiated physical therapy with a bedside trapeze to improve independence and activities of daily living.
Months 2-5
The patient was medically optimized by the multidisciplinary team over the subsequent month and was discharged home with home health care at approximately 2 months postoperatively. At this point the patient was functional with most activities of daily living, including using a wheelchair. He was subsequently followed in the plastic surgery clinic on an outpatient basis with continued wound care to his fillet flap and no major sequelae to date.
Pearls
- Pre-operative Planning: Hemicorporectomy reconstruction requires extensive multidisciplinary coordination.
- Careful operative sequencing is necessary to minimize blood loss and maintain hemodynamic stability.
- Flap Design: The thigh fillet flap functions as an axial-pattern flap capable of providing extensive soft-tissue coverage without creating additional donor-site morbidity.
- Postoperative Support: Patients require extensive psychological evaluation and counseling regarding:
- perioperative mortality risk
- lifelong functional limitations
- need for prolonged postoperative care and rehabilitation.
Pitfalls
- Early Venous Congestion
- Fillet flaps are susceptible to venous congestion, which may require early intervention such as medicinal leech therapy.
- Pressure Offloading
- Failure to offload pressure on the flap may lead to wound dehiscence and flap necrosis. This risk is increased in patients with:
- prior radiation therapy
- chronic pressure injuries
- prolonged immobility.
- Use of air-fluidized beds and strict repositioning protocols is essential.
Post-operative plan
- Strict bedrest
- Pressure offloading using air-fluidized mattress
- Trapeze for upper-body repositioning
- Physical therapy for activities of daily living
- Bedside psychotherapy offered
- Labs discontinued as soon as normalized
- Close monitoring for wound dehiscence
References
cher MV, Erdmann D, Homann HH, Steinau HU, Levin SL, Germann G. The concept of fillet flaps: classification, indications, and analysis of their clinical value. Plast Reconstr Surg. 2001;108(4):885-896. doi:10.1097/00006534-200109150-00011
Greendyk JD, Haider SF, Allen WE, Prasath V, Chokshi RJ. Redefining the Role of Hemicorporectomy in the Modern Era and Shifting Trends Toward Non-Malignant Indications. Am Surg. 2025;91(9):1526-1533. doi:10.1177/00031348251346533