Keywords: Shark island flap, facial skin defect, BCC, nasal skin cancer, nasal reconstruction, reconstructive surgery
Authors: Mickie Bang Christensen (MD), Magnus Avnstorp (MD), Department of Plastic- & Breast Surgery, Zealand University Hospital Roskilde, Denmark
Abstract
This case presents the use of a modified shark island flap for reconstruction of a defect on the ala nasi following excision of a basal cell carcinoma in a 85-year old male. Due to the tumor size and location, direct closure was not feasible. The shark island flap was chosen as the reconstructive approach. Surgery was done under local anesthesia. Excision of the tumor was done with a 3 mm margin. Histology from frozen sections showed clear margins without malignancy. Postoperative follow up at both one week and two months demonstrated a satisfactory cosmetic outcome and no signs of recurrence.
Patient medical history
85-year old male with a medical history of atoxic goiter, hypertension, Parkinson’s disease, melanoma and multiple skin carcinomas, was referred with 3 facial skin carcinomas (dorsum nasi, right ala nasi and left side of the upper lip). This case focuses on the carcinoma on the ala nasi. The biopsy showed basal cell carcinoma of nodular subtype. The patient had years prior been operated with a bilobed flap due to a skin carcinoma on the right dorsum nasi, which had resulted in bulging of the right side of the dorsum.
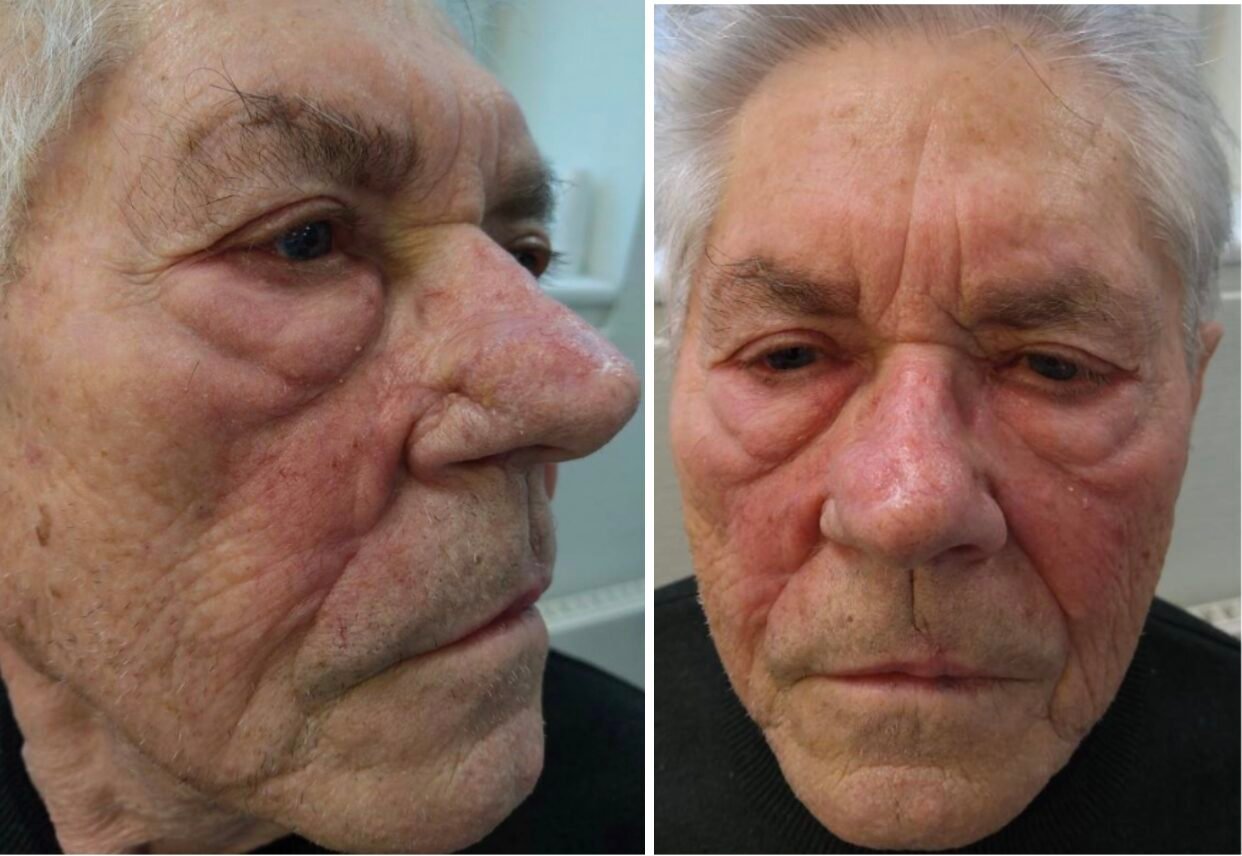
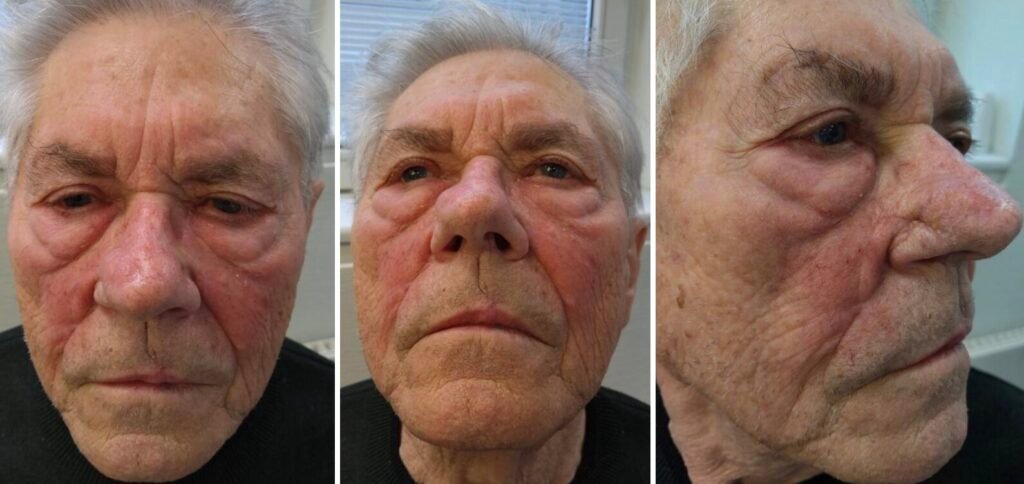
Before and After
Patient examination
Well preserved male with poor skin quality. On clinical examination, a tumor measuring 6 x 5 mm and 2 mm elevation from the surface of the skin was found on the right ala nasi, involving the nasal sulcus. Clinically not adherent to underlying tissue. There were no palpable regional lymph nodes.
Pre-operative considerations
Surgery and radiation were discussed with the patient. The patient preferred surgery. Due to the tumor size and location, direct closure was not feasible. FTSG would delete the alar-facial sulcus, create a big, visible scar and result in an unsatisfactory cosmetic outcome. The location of the tumor and the size and depth of the nasolabial crease made a local flap the optimal solution for reconstruction. The shark island flap is a reliable myocutaneus flap perfectly fitted for reconstruction in the area close to the lateral/upper border of the ala nasi and can help create excellent aesthetic outcomes, recreate the ala nasi crease and create little visibility of the scar. Its pedicle provides excellent blood supply and minimal risk of necrosis. Alternatively, a nasolabial flap was considered too, but due to the location and size of the tumor, the shark island flap was chosen.
Patient information:
At the outpatient clinic and later pre-operatively on the day of surgery, the patient was informed about the risks of infection, bleeding, hematoma, flap necrosis, asymmetry of the nose, nerve damage, changed sensation and possibly a second surgery if final histology would show unclear margins.
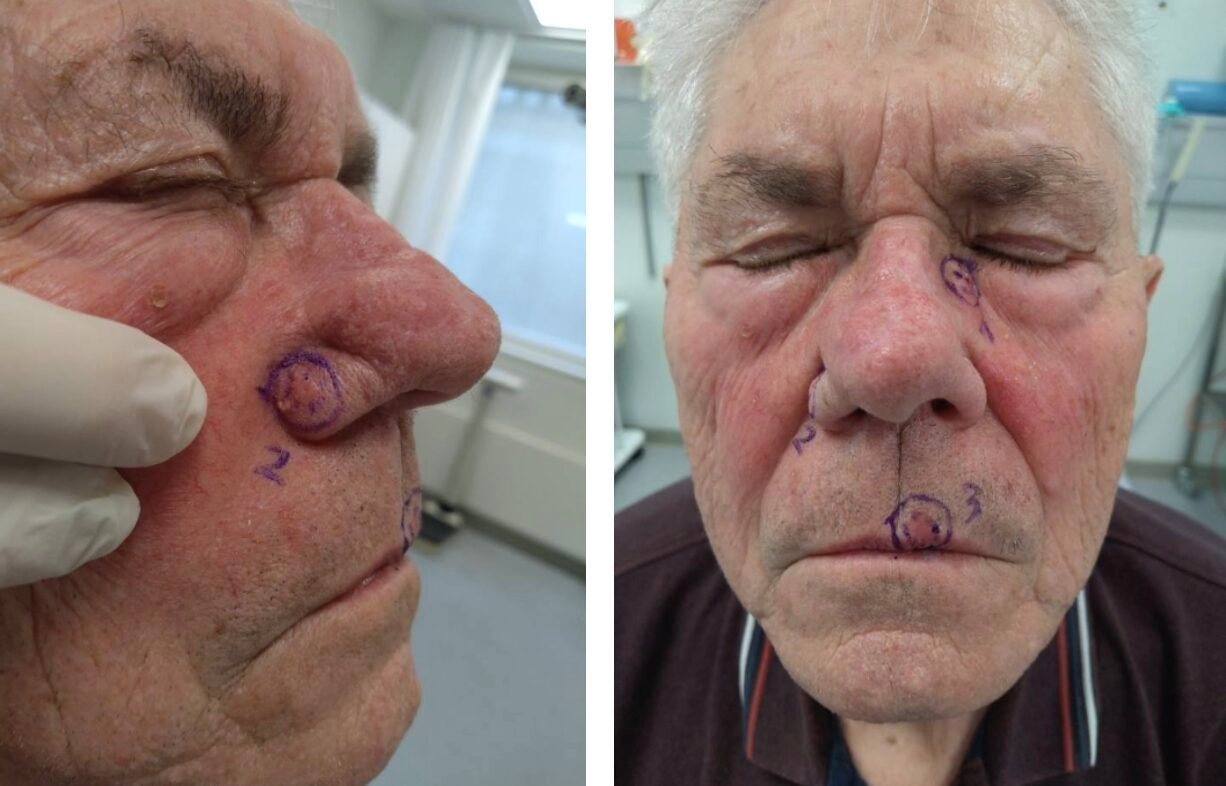
BCC excision and flap design
Excision with frozen sections and a 3 mm safety margin resulted in a defect measuring 9 x 8 mm. The tumour was marked by needle at 12’o clock, superiorly. Frozen sections showed clear margins.
The shark island flap is a myocutaneus flap first described by Cvancara and Wentzell in 2006 and obtained the name due to its shark-like shape. It is indicated for reconstruction of the alar and perialar defects, since it involves a rotation that gives rise to the formation of an inverted cone that recreates the alar sulcus. The flap derives its blood supply from the levator labii superioris muscle and requires careful dissection to preserve the vascular pedicle.
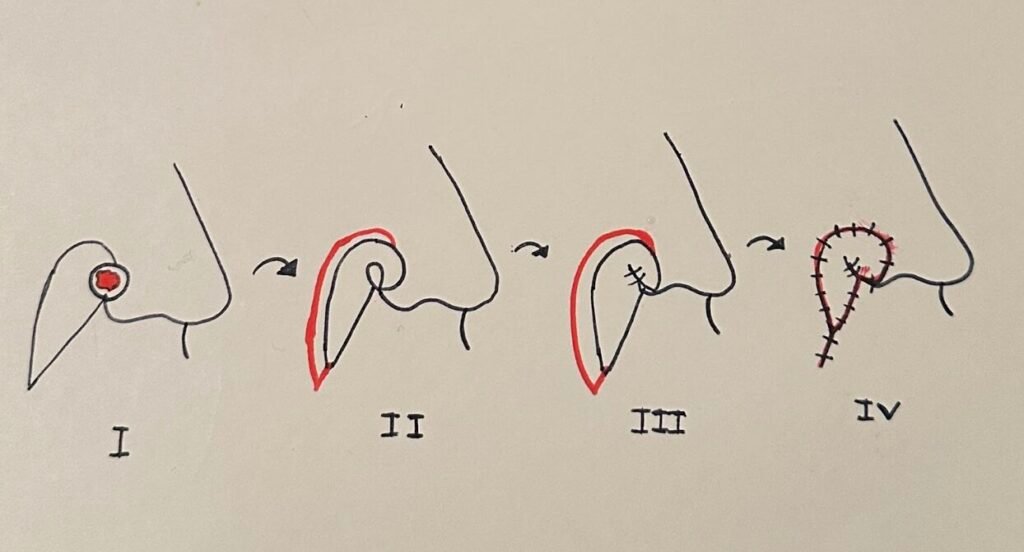
I. The flap is drawn by measuring the width of the defect from the lateral alar sulcus to the medial edge of the defect. A matching width of a short limb of the flap is measured. The long limp of the flap goes down the cheek with the inferior portion of the island pedicle. Then the medial edge of the flap is drawn on the nasolabial fold.
II. Then the subcutaneous pedicled flap is incised. Carefully undermining is done in order to preserve musculature at the base of the pedicle on the short limb.
III. The short limb is rotated 90 degrees, perpendicular to the melolabial part of the flap, thereby recreating the alar sulcus. The first deep suture pulls the upper lateral part towards the nasofacial sulcus, allowing the short limb to drape down into the defect. The second deep suture pulls the short limb down to the inferior border of the defect..
IV. The remainder of the flap is carefully sutured deeply and superficially, avoiding too many deep sutures to minimize the risk of necrosis. (1)
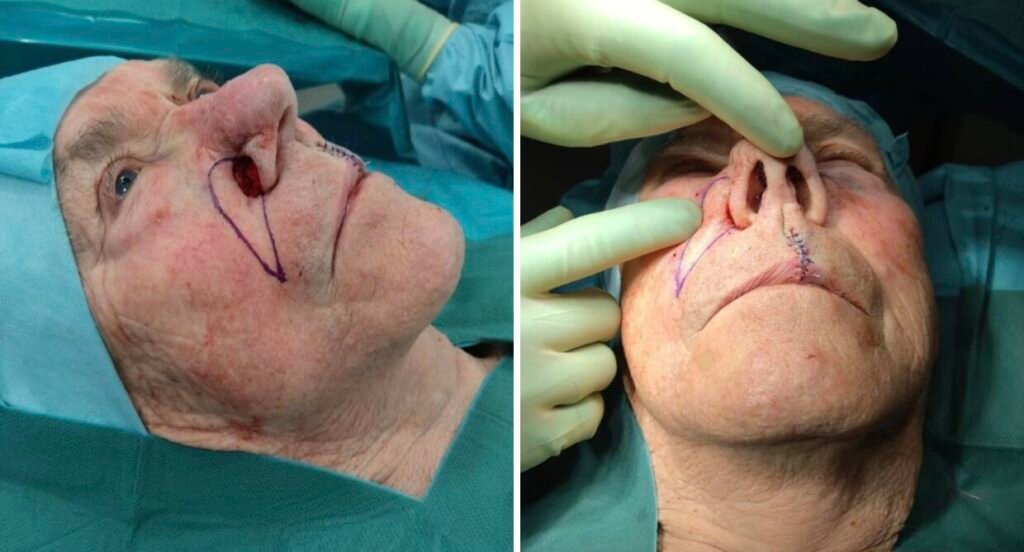
Drawing of the flap
The flap was drawn on the patient as shown on the drawing from step 1.
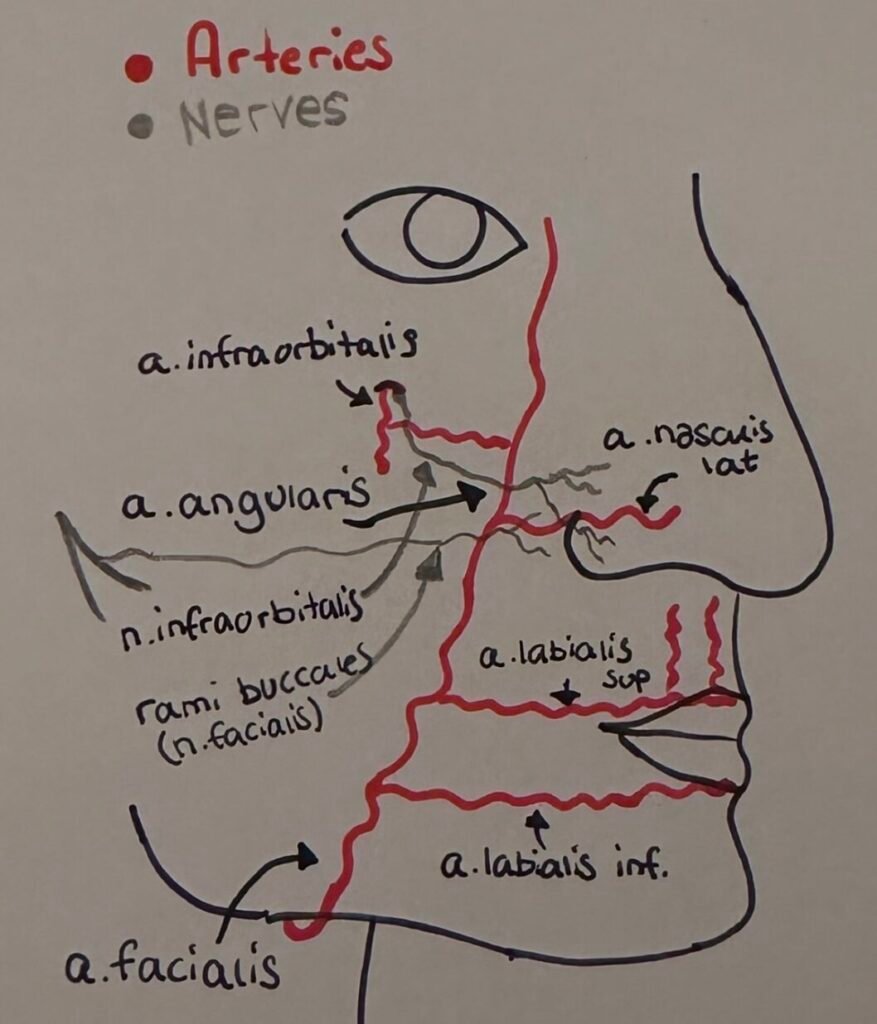
Anatomy
Subcutaneous dissection is carefully done in order not to damage the facial artery and its branches. The flap receives its nervous innervation from n. infraorbitalis and rami buccales. Adequate pedicle size is important in order to avoid necrosis. Furthermore, it’s crucial to identify the alar crease and the nasolabial fold and draw the flap according to those anatomical landmarks.
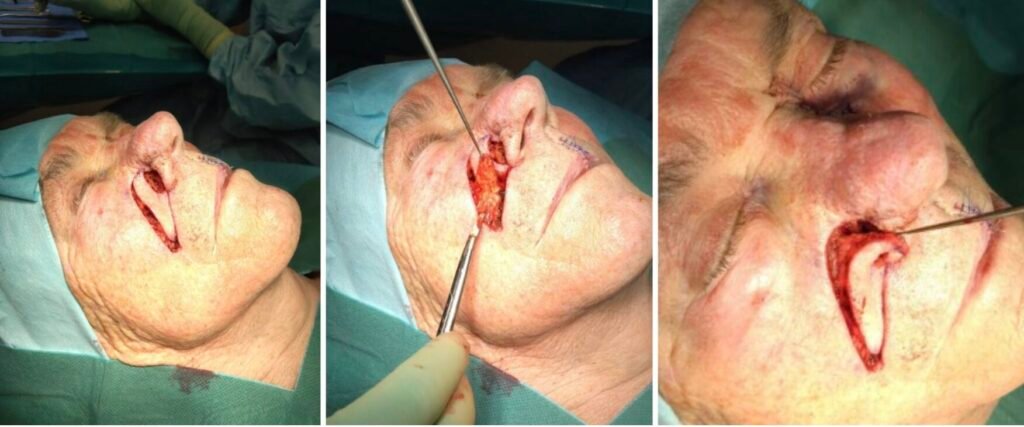
Step 5. Flap elevation and subcutaneous dissection
The flap was carefully incised and subcutaneously dissected in order to preserve the musculature at the base of the pedicle.
Step 6. Modification and folding of the flap
The short limb of the flap is lifted towards the nose, folded and then sutured with 5-0 absorbable polyfilament sutures. The inferior part of the flap-defect is closed, also with 5-0 sutures, successfully re-creating the nasolabial fold. The long limb of the flap is trimmed/shortened, making it more well-fitted for the defect.
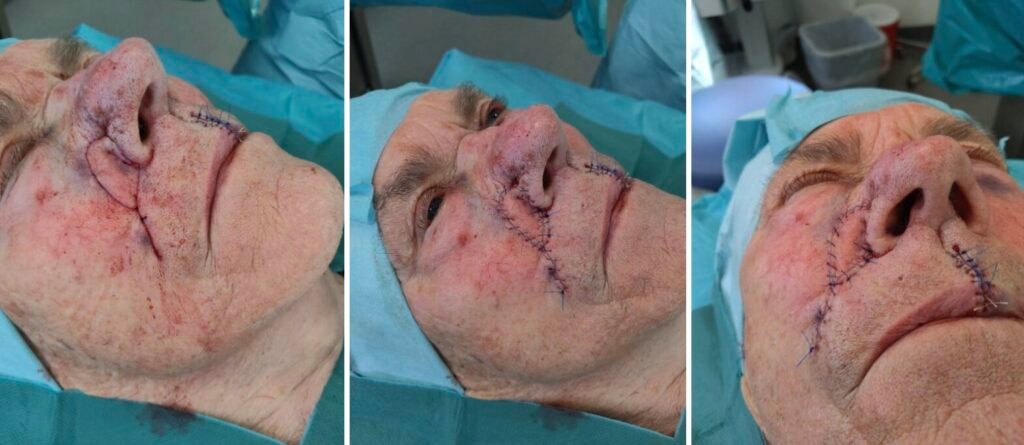
step 7. Sutures
The remaining part is sutured with a few 5-0 absorbable polyfilament sutures. Finally, the skin is sutured with 5-0 continuous non-absorbable monofilament sutures, ensuring precise adaptation of the skin edges.
Step 8. One week follow-up
The patient presented with discrete hematoma on the cheek. The flap, fully healed, with a small amount of central bulging. Normal capillary response. The patient had no complaints
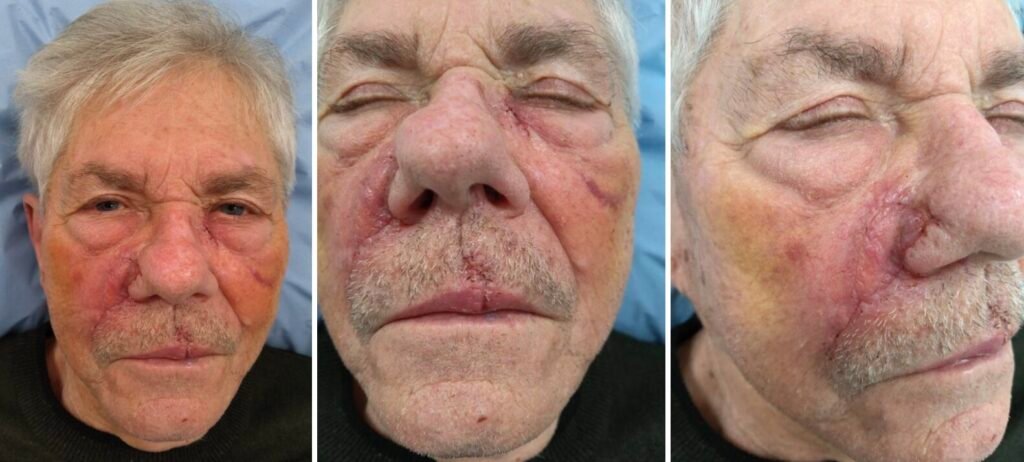
Step 9. Two months follow-up
The flap was seen fully healed and the central bulging gone. The alar crease and the nasolabial fold had been recreated due to the flap design, blending well with the contralateral side. No signs of recurrence. The patient was satisfied with the cosmetic outcome.
Pearls
– Ideal for reconstruction of smaller defects on the ala nasi/alar sulcus.
– Thinning of the flap: avoid trap door effect/too voluminous flap on the ala nasi.
– Preservation of the subunits of the nose: the rotational movement of the flap forms an inverted cone that effectively recreates the alar sulcus. The linear scarring at the base of the flap follows and imitates the nasolabial fold, making it almost unnoticeable.
– Single-stage procedure
Pitfalls
– Flap necrosis: loss of blood supply, often due to improper dissection or failure to preserve the feeding vessel (angular artery/pedicle). Can be avoided by careful subcutaneous dissection, especially in the short limb of the flap.
– Alar retraction or obvious scarring: improper tension during closure or inaccurate design lead to alar retraction. Failure to properly identify the nasolabial fold and the alar-facial sulcus can lead to obvious scarring rather than hidden along the natural lines.
– “Trap door” effect: occurs if the tissue thickness discrepancies between the flap and the surrounding skin of the nose. Can be avoided by careful thinning of the flap or slightly over-correcting the defect for swelling.
– Poor patient selection: the flap is unsuitable for larger defects of the ala nasi and perialar region. Here, consider a nasolabial flap instead. If the excision of the tumor results in a full thickness defect, consider a spear lap.
Post-operative plan
The patient was advised to keep the head elevated and refrain from consuming hot beverages and food 1-2 days after surgery. Additionally, no strenuous physical activities or swimming until removal of the sutures 7 days post-operatively.
References
B.M.G. Perez-Paredes et al. Colgajo «en tiburón» para la reconstrucción de defectos de la región alar nasal. Actas Dermosifiliog. (2014)
Saraiva LPPG, Guimarães RV, Loda G, Benez M. Surg Cosmet Dermatol. Rio de Janeiro v.12 (S1); out-dez. 2020 p. 11-4.