Keywords: Nasal reconstruction following NMSC, Transposition flaps, Utilizing existing flap as design solution
Authors: Frederik Penzien Wainer Mamsen & Lukas Kure-Rosenberg. Dept Plastic & Breast Surgery, Zealand University Hospital, Denmark.
Abstract
Background: Secondary nasal reconstruction adjacent to prior local flaps poses unique challenges due to scarring, altered tissue mobility, and potentially unpredictable vascular territories. Although bilobed flaps are considered workhorse techniques in nasal reconstruction, their presence may limit options in recurrent malignancy. Strategic flap planning that respects vascular integrity and aesthetic subunits is therefore essential. Case Presentation: A 74-year-old male patient presented with biopsy-proven recurrent basal cell carcinoma of the right nasal sidewall within a previously reconstructed area using a 180-degree bilobed flap. Tumor excision created an 8 × 11 mm defect abutting the prior reconstruction. Direct closure, secondary intention healing, and skin grafting were deemed unsuitable because of the risk of nasal distortion and alar contracture. Methods: A lateral-based trilobed transposition flap was designed to encircle the prior bilobed flap while preserving its vascular pedicle and redirecting perfusion toward unscarred tissue. The first lobe closed the primary defect, and subsequent lobes redistributed tension vectors. Subcutaneous undermining was performed to preserve the subdermal plexus. Results: The flap demonstrated stable perfusion without ischemia or venous congestion. Healing was uneventful. At 1.5-month follow-up, the patient showed great contour with slight pincushion, preserved nasal symmetry, and a favorable color match. Conclusion: In nasal reconstruction adjacent to prior flap surgery, a lateral-based trilobed flap is a safe and effective single-stage option. Careful vascular planning and tension redistribution enable reliable secondary reconstruction with excellent functional and aesthetic outcomes.
Patient medical history
Introduction Bilobed flap designs are considered a versatile workhorse in nasal reconstruction because excess skin from the upper and lateral nasal units can be transposed to more distal parts of the nose, where little to no excess skin is available for defect closure [1,2]. Reconstructing nasal defects in previously operated areas poses unique challenges due to altered tissue mobility, scarring, and potentially compromised vascular territories [3–5]. Although neovascularization develops over time after flap surgery, the predictability of the blood supply in secondary reconstructions remains variable [6,7]. Strategic flap design is therefore essential when operating adjacent to prior local flaps. Bilobed flaps were originally designed with a 180-degree rotation (90 degrees per lobe), but a modified 90-degree rotation (45 degrees per lobe) has gained popularity because it thereby decreases pivotal tension, minimizing “cone” formation [4,8,9]. Trilobed flap design follows the same principle as the bilobed flap and can be performed with a 135-degree rotational axis, which allows for larger defect closure or addressing defects at the most distal parts of the nose [10], hence utilizing an angle of rotation somewhere between the original and the later modified bilobed flap design. Medical history A 74-year-old male patient presented with biopsy-proven mixed invasive subtype of basal cell carcinoma located on the right lateral nasal sidewall. The patient presents without the use of blood thinners, has no case relevant medical history, and takes no regular medication. No history of tobacco or alcohol abuse.
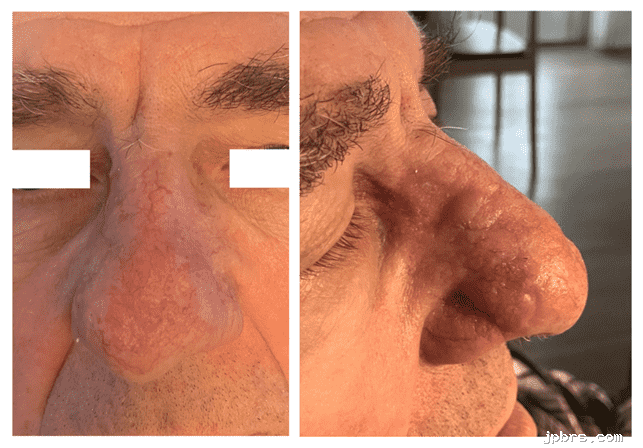
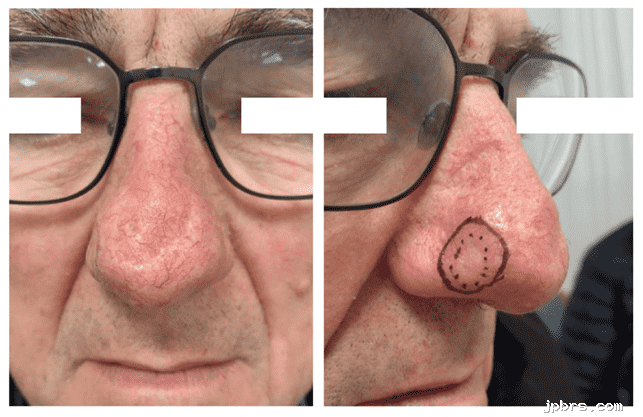
Before and After
Patient examination
Patient examination
The patient had a history of nasal carcinoma and prior nasal reconstruction with a 180-degree bilobed flap following skin cancer excision (Figure 1). On examination, the nose showed an intact contour but limited local tissue recruitment in the region of the prior flap and in relation to the new surgical site.
Pre-operative considerations
Pre-operative considerations
When planning reconstruction in an area with a history of prior flap surgery, several principles guided by decision-making and reconstruction were planned with the following principles:
u0026#8226; Vascular memory is incomplete: Although neovascularization occurs over months to years, axial and perforator reliability may remain unpredictable in scarred tissue [6,7]
u0026#8226; Flap pedicles should be based in virgin territory whenever possible [3,5,11]
u0026#8226; Tension vectors must be redistributed to avoid distortion of the alar rim or nasal tip [12]
u0026#8226; Subunit preservation is essential for optimal aesthetic outcome [13]
The two-stage nasolabial flap was considered but deemed suboptimal given the patient’s preference for a single-stage approach. A lateral-based trilobed flap was designed to encircle the prior 180-degree bilobed flap while preserving its vascular pedicle within the intact lateral nasal skin. Importantly, flap perfusion was oriented away from the region potentially compromised by prior surgery.
The first lobe was used to close the primary defect, while the additional lobes redistributed tensional forces. The final donor site was closed without distortion. Subcutaneous undermining was performed to preserve the subdermal plexus and improve flap mobility. The flap was inset without undue tension, resulting in stable immediate perfusion.

Figure 1: Preoperative tumor view
Preoperative view showing recurrent BCC on the right nasal sidewall in conjunction with a previously bilobed flap reconstruction.
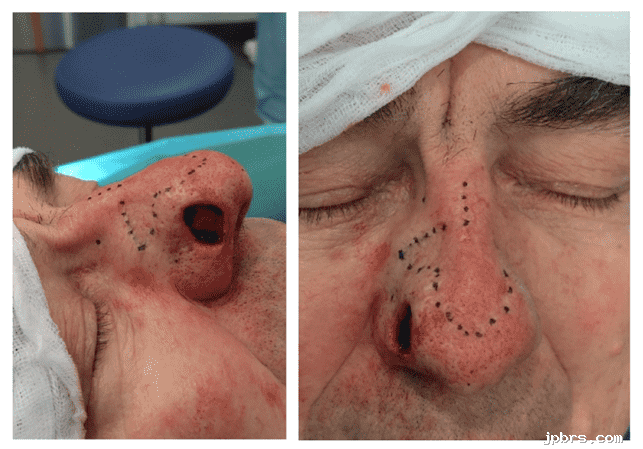
Figure 2: Tumor excision – including freeze section biopsies
Intraoperative defect after oncologic excision, with markings of the prior bilobed flap utilizing a 180-degree flap design. The tumor was excised with a 3-mm clinical margin. Intraoperatively, five representative samples were sent for frozen-section histopathological analysis and came back showing clear margins.
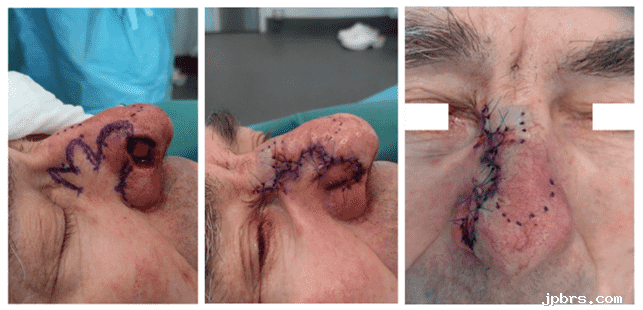
Figure 3: Flap incision, mobilization suturing
Markings of the new reconstruction before and after the flaps were raised, demonstrating a lateral-based trilobed flap encircling the previous flap. The trilobed flap design was tested using cotton-gaze from the pivotal point to flap outlines before excision and flap elevation. Undermining of the surrounding tissue was performed to improve tissue mobility with respect to the previous flap design. The most distal flap was transposed into the defect and secured with Vicryl 5.0 sutures. Likewise, the second and third flaps were transposed and secured. The remaining defect was closed with direct suture. Prolene 5.0 single sutures were used to close the skin. Capillary refill was assessed with no signs of venous congestion or ischemia.
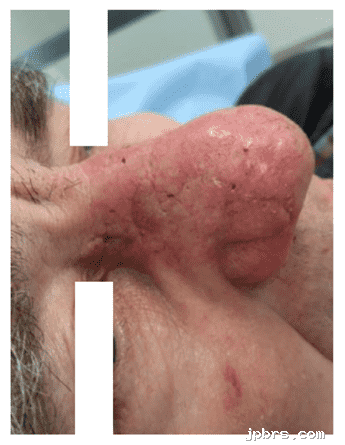
Figure 4: Suture removal 7 days post operation
Postoperative healing was uneventful, with no evidence of ischemia or venous congestion. Seven days after surgery, the flap demonstrated good viability and contour, with minimal edema.

Figure 5: Result at 1.5-month follow-up.
At 1.5-month follow-up, the reconstruction showed excellent color match, preserved nasal symmetry, and inconspicuous scarring
Pearls
u0026#8226; Vascular memory is incomplete: Although neovascularization occurs over months to years, axial and perforator reliability may remain unpredictable in scarred tissue [6,7]
u0026#8226; Flap pedicles should be based in virgin territory whenever possible [3,5,11]
u0026#8226; Tension vectors must be redistributed to avoid distortion of the alar rim or nasal tip [12]
u0026#8226; Subunit preservation is essential for optimal aesthetic outcome [13]
Pitfalls
u0026#8226; Alteration of original flap designs must be performed with great care to prevent distortion of the alar rim and nasal tip [12]
u0026#8226; Not respecting existing cicatrice lines can increase risk of tissue necrosis [3,5,11]
u0026#8226; Not testing the pivotal transposition of each drawn flap to ensure tensionless closure.
Post-operative plan
Postoperative plan
Postoperatively, a micropore bandage was applied over the cicatrice. The patient was instructed to rest for the first 2 days, avoiding hot or spicy foods or drinks, keeping his head elevated during sleep and avoiding exercise. For the following 5 days, normal rest was recommended. The patient was advised not to shower for 24 hours and keep the plaster on until suture removal 7 days postoperatively.
Discussion
This case illustrates the importance of strategic vascular planning in secondary nasal reconstruction. Surgery following prior flap surgery requires careful consideration of vascular reliability and flap geometry. Although vascular remodeling and neovascularization may occur over time, reliance on previously manipulated tissue potentially remains unpredictable [6,7].
The trilobed flap, though less commonly used than bilobed designs, offers increased control of tension vectors and allows greater flexibility in pedicle placement, as demonstrated here by deliberate placement within unscarred tissue. In the context of prior flap surgery, this adaptability becomes a significant advantage.
References
1. Pathan I. The Bilobed Flap – Critical Analysis and New Mathematically Precise Design. Eplasty. 2024;24:e42.
2. Tan E, Mortimer NJ, Hussain W, Salmon PJ. The Nasal Sidewall Rotation Flap: A Workhorse Flap for Small Defects of the Distal Nose. Dermatol Surg. 2010 Oct;36(10):1563–7.
3. Nasal Reconstruction [Internet]. Elsevier; 2009 [cited 2026 Feb 9]. Available from: https://linkinghub.elsevier.com/retrieve/pii/C20090375169
4. Zitelli JA. The Bilobed Flap for Nasal Reconstruction. Arch Dermatol. 1989 Jul 1;125(7):957.
5. Spataro E, Branham G. Principles of Nasal Reconstruction. Facial Plast Surg. 2017 Feb;33(01):009–16.
6. Taylor GI, Palmer JH. The vascular territories (angiosomes) of the body: experimental study and clinical applications. Br J Plast Surg. 1987 Mar;40(2):113–41.
7. Sloan GM, Reinisch JF. Flap physiology and the prediction of flap viability. Hand Clin. 1985 Nov;1(4):609–19.
8. Mole RJ, Hohman MH, Sebes N. Bilobed Flaps. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2025 [cited 2026 Feb 9]. Available from: http://www.ncbi.nlm.nih.gov/books/NBK470355/
9. Esser J. Gestielte lokale Nasenplastik mit zweizipfligem Lappen, Deckung des sekundären Defektes vom ersten Zipfel durch den zweiten. Dtsch Z Für Chir. 1918;
10. Iida N, Ohsumi N, Sakai M. A Trilobed Flap for Reconstruction of Nasal Skin Defects: Plast Amp Reconstr Surg. 1997 Sep;100(Supplement 1):991–5.
11. Zitelli JA, Fazio MJ. Reconstruction of the nose with local flaps. J Dermatol Surg Oncol. 1991 Feb;17(2):184–9.
12. Cook JL. The reconstruction of the nasal ala with interpolated flaps from the cheek and forehead: design and execution modifications to improve surgical outcomes. Br J Dermatol. 2014 Sep;171:29–36.
13. Burget GC, Menick FJ. The Subunit Principle in Nasal Reconstruction: Plast Reconstr Surg. 1985 Aug;76(2):239–47.