Keywords: SCC, Flap, Reconstruction, Nose, Novel, Hybrid
Authors: Lukas Kure-Rosenberg, Magnus Balslev Avnstorp. Dept Plastic & Breast Surgery, Zealand University Hospital, Denmark.
Abstract
Background: Proximal dorsal nasal defects are commonly reconstructed with glabellar advancement flaps. However, in selected patients with favorable distal tissue mobility, alternative local strategies may provide equivalent reconstruction while preserving aesthetic subunits thus minimizing scar burden. Case Presentation: An 84-year-old male underwent oncologic excision of a 13-mm moderately differentiated squamous cell carcinoma of the proximal nasal dorsum. The resulting full-thickness defect extended toward the nasal bulb. Preoperative assessment showed significant bulbous skin mobility and distal redundancy without prior surgical scarring. Methods: Instead of glabellar recruitment, reconstruction was performed with a hybrid local advancement strategy combining Peng-inspired medialization with a limited Rintala/H-type advancement component. Tissue was mobilized in the subcutaneous plane to preserve the subdermal plexus, and distal advancement was maintained lateral to the midline to protect dorsal contour symmetry. Results: Flap perfusion remained stable, with no ischemia or venous congestion. At the two-month follow-up, the patient showed a preserved dorsal contour, symmetrical nasal lines, and satisfactory scar placement, without trapdoor deformity or tip distortion. Conclusion: Selected proximal dorsal nasal defects can be reconstructed with hybrid local advancement techniques that strategically exploit distal tissue redundancy. Context-driven modification of established flap principles may allow avoidance of glabellar flaps while maintaining excellent functional and aesthetic outcomes.
Patient medical history
An 84-year-old male was referred to the Department of Plastic Surgery at Roskilde Sealand University Hospital, Denmark, in winter 2025 by a dermatologist for evaluation of a lesion on the dorsal nose. Following the establishment of a middle-differentiated squamous cell carcinoma (SCC) diagnosis via biopsy, it was deemed necessary for surgical hospital-based treatment. The patient had no history of tobacco use or alcohol abuse.
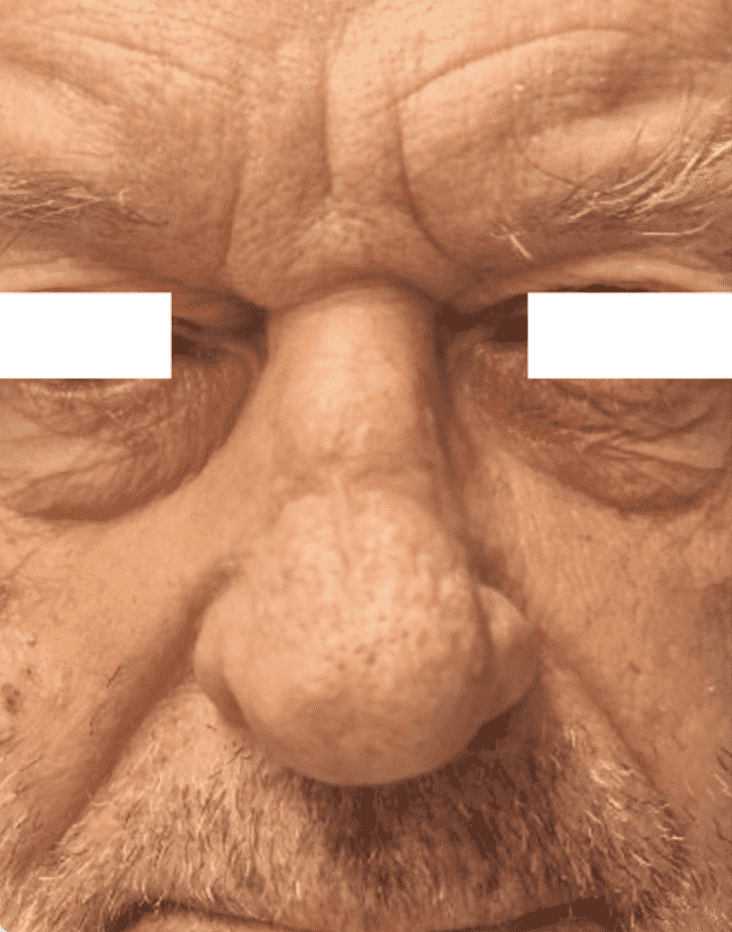
Before and After
Patient examination
The SCC of the nasal dorsum measured 12 mm in diameter. Preoperative assessment demonstrated tumor mobility, significant skin redundancy, and mobility of the nasal bulb, with preserved tissue quality and laxity lateral to the distal portion of the defect. The surrounding skin was free of prior surgical scars (Figure 1).
Pre-operative considerations
Introduction:
Reconstruction of proximal dorsal nasal defects remains technically demanding because of limited tissue availability, competing tension vectors, and the risk of contour distortion across aesthetic subunits. The glabellar advancement flap has long been considered a reliable workhorse for upper dorsal defects, offering robust vascularity and predictable advancement. However, glabellar recruitment inevitably violates the glabellar subunit and may introduce vertical scarring, brow distortion, or altered dorsal contour in selected patients.
The Rintala flap, originally described as a midline dorsal advancement flap for upper nasal defects, represents a transverse advancement concept that utilizes laxity of the nasal dorsum while preserving subunit integrity (ref 1). The technique allows recruitment of tissue from the proximal dorsum through wide subcutaneous undermining. Despite its conceptual simplicity and reliable outcomes in appropriately selected cases, the Rintala is less frequently reported in contemporary series. This decline may reflect the increasing popularity of bilobed and transposition flaps, as well as concerns about limited potential for advancement and the risk of tension-related dorsal flattening in larger defects.
More recently, the Peng flap has gained recognition as a versatile advancement-rotation concept for distal and mid-dorsal defects (ref 2). By combining bilateral advancement with medial rotation, the Peng flap redistributes tension vectors while preserving the dorsal aesthetic lines. Its strength lies in controlled medialization without central distortion, particularly in patients with bulbous or redundant distal nasal skin.
Both Rintala and Peng concepts share a fundamental principle: tension redistribution through strategic local advancement rather than distant tissue recruitment. However, their application to proximal dorsal defects remains selectively described. In patients with favorable distal tissue mobility, hybridization of these established principles may provide an alternative to glabellar advancement while preserving midline symmetry and dorsal contour (ref 3).
The present case illustrates how context-driven recombination of Rintala-type transverse advancement with 180-degree Peng-inspired medialization can facilitate reconstruction of a proximal dorsal defect without glabellar recruitment.
Pre-Operative Considerations:
Perioperative frozen-guided excision with a 7-mm margin resulted in a relatively large full-thickness defect on the proximal dorsum nasi, extending toward the nasal bulb. The defect reached the perichondrium of the upper lateral cartilage, with no evidence of residual disease in any of the frozen histology sections (Figure 2). The patient was scheduled for flap reconstruction in the same session.
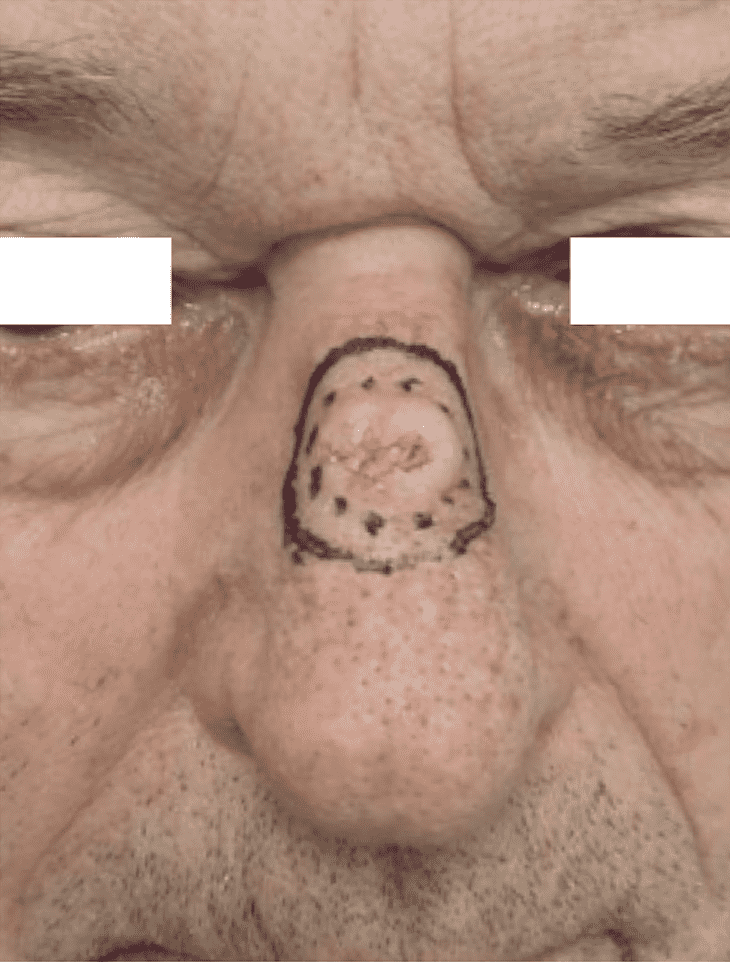
Step 1: Preoperative Assessment
Preoperative marking of the 12mm diameter middle-differentiated SCC of the nasal dorsum.
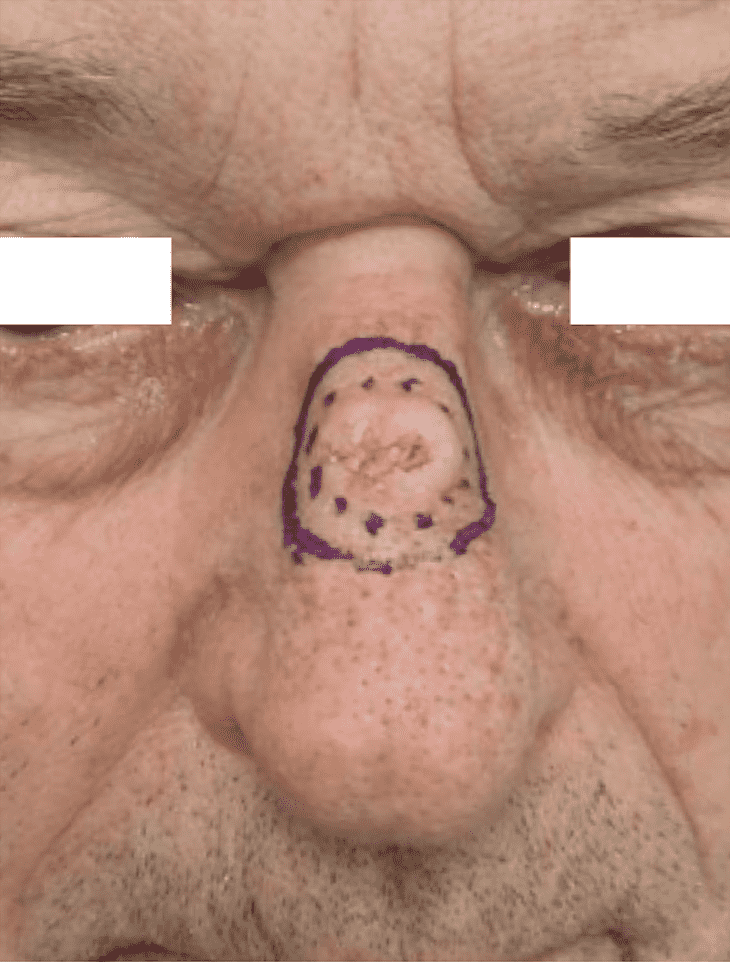
Step 2: Excision of tumor and marking of the the Dual-Hybrid flap design.
Perioperative frozen-guided excision with a 7-mm margin resulted in a relatively large full-thickness defect on the proximal dorsum nasi, extending toward the nasal bulb. The defect reached the perichondrium of the upper lateral cartilage, with no evidence of residual disease in any of the frozen histology sections (Figure 2). The patient was scheduled for flap reconstruction in the same session.
Various surgical options were evaluated based on the defect’s size, and it was determined that the abundance of surrounding skin, both proximal and distal to the defect, was sufficient for closure if mobilized carefully. Distal Backcuts for flap elevation is marked.
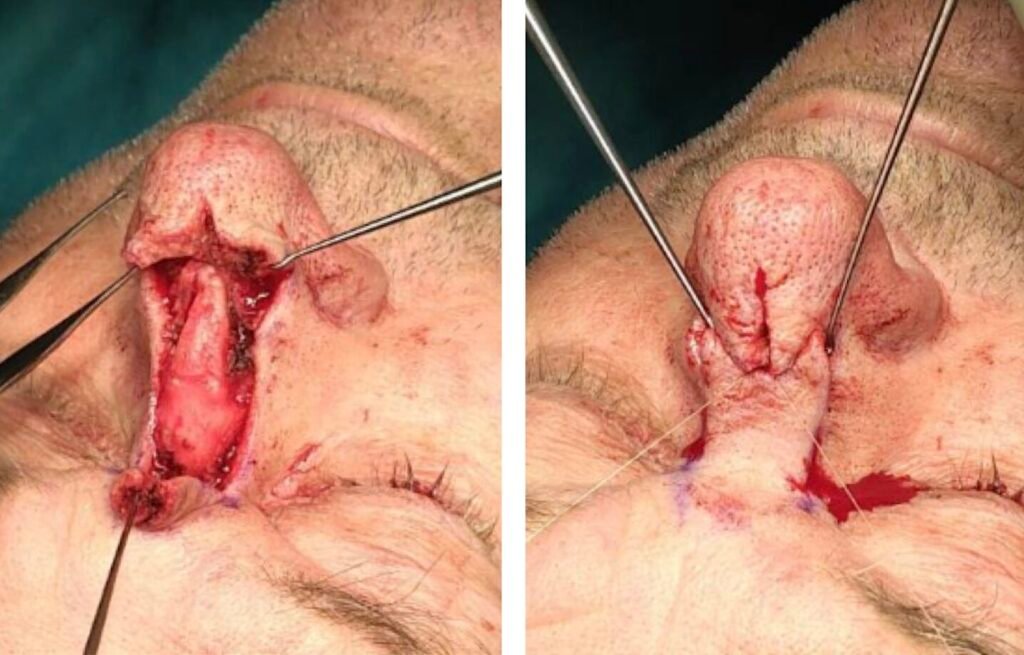
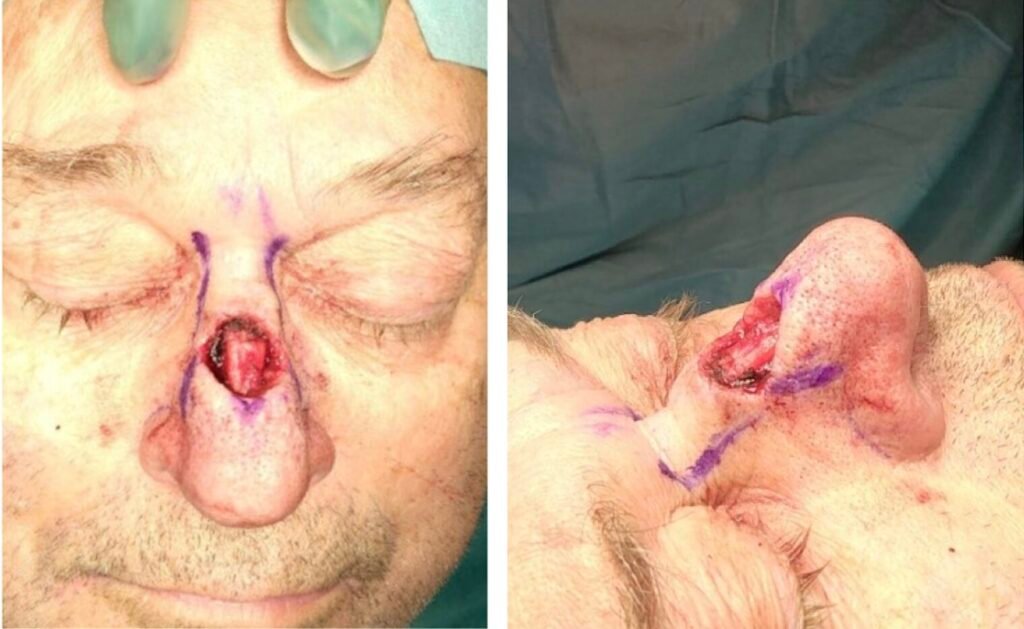
Step 3: Flap incision and mobilization
The lateral skin adjacent to the distal aspect of the defect’s lateral sides was mobilized and advanced medially in a modified, opposite Peng-flap-inspired fashion. This was combined with a proximal limited H-flap advancement, a minor Rintala-type concept, allowing recruitment of excess peri-defect skin with optimal fit and coverage of the remaining defect without involving other subunits of the nose. Undermining was performed in the subcutaneous plane to preserve the subdermal plexus and improve flap mobility. The combined advancement allowed for a tension-free closure without (supra)tip distortion.
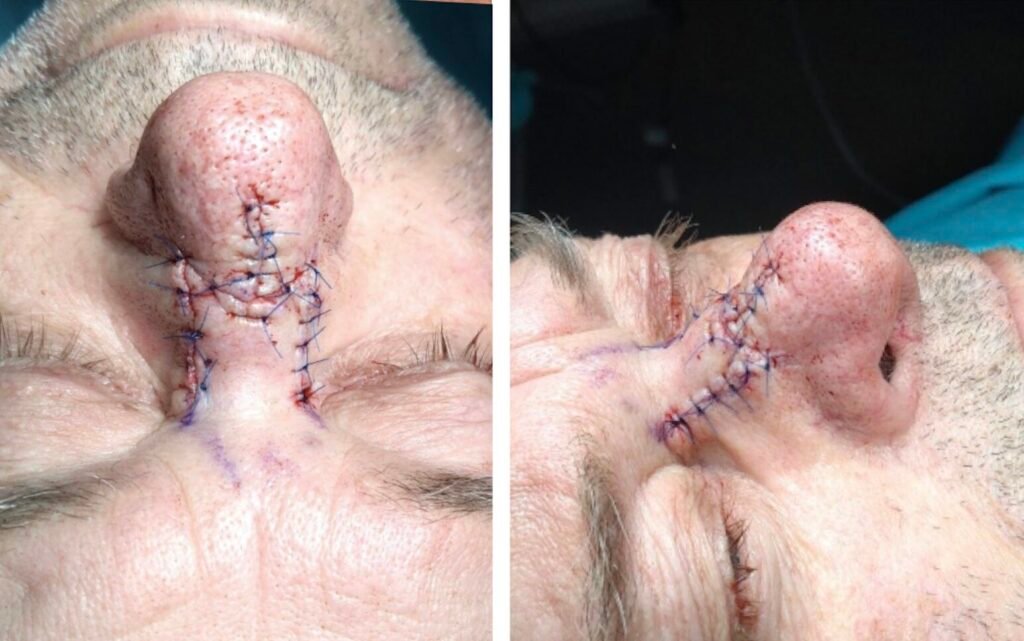
Step 4: Flap suturing
The flaps were transposed into the defect and secured with Vicryl 5.0 sutures. Prolene 5.0 single sutures were used to close the skin. Capillary refill was assessed, with no signs of venous congestion or ischemia.
The flaps were transposed into the defect and secured with Vicryl 5.0 sutures. Prolene 5.0 single sutures were used to close the skin. Capillary refill was assessed, with no signs of venous congestion or ischemia.
The flaps were transposed into the defect and secured with Vicryl 5.0 sutures. Prolene 5.0 single sutures were used to close the skin. Capillary refill was assessed, with no signs of venous congestion or ischemia.
The flaps were transposed into the defect and secured with Vicryl 5.0 sutures. Prolene 5.0 single sutures were used to close the skin. Capillary refill was assessed, with no signs of venous congestion or ischemia.
Pearls
- Not all proximal dorsal nasal defects require glabellar recruitment. Assess distal mobility before defaulting to glabellar recruitment (ref 5)
- Bulbous nasal skin may offer underutilized advancement potential (ref 6, 7)
- Combining Peng-type medialization with limited Rintala/H-flap advancement allows precise tension control and modulates tension distribution (ref 8, 9)
- Maintaining distal advancement lateral to the midline helps preserve dorsal aesthetic lines (ref 10)
- Novelty in nasal reconstruction often lies in strategic recombination, not in new flap invention (ref 11, 12)
Pitfalls
- Large defects and limited undermining when using a classic Rintala flap, can cause vertical tension vectors and subsequent tip elevation (ref 13)
- Limited advancement and secondary wound tension can lead to trapdoor deformity and hypertrophic scarring (ref 14)
Post-operative plan
The postoperative course was uneventful, with no signs of ischemia, venous congestion, or wound dehiscence. Suture removal was performed by the patient’s general practitioner on postoperative day 7. Early follow-up after 1.5 months showed satisfactory contour restoration and acceptable scar placement. The proximal nasal dorsum and distal bulb remained symmetric, with no clinical evidence of trapdoor deformity or tip elevation/distortion
The postoperative course was uneventful, with no signs of ischemia, venous congestion, or wound dehiscence. Suture removal was performed by the patient’s general practitioner on postoperative day 7. Early follow-up after 1.5 months showed satisfactory contour restoration and acceptable scar placement. The proximal nasal dorsum and distal bulb remained symmetric, with no clinical evidence of trapdoor deformity or tip elevation/distortion
The postoperative course was uneventful, with no signs of ischemia, venous congestion, or wound dehiscence. Suture removal was performed by the patient’s general practitioner on postoperative day 7. Early follow-up after 1.5 months showed satisfactory contour restoration and acceptable scar placement. The proximal nasal dorsum and distal bulb remained symmetric, with no clinical evidence of trapdoor deformity or tip elevation/distortion