Keywords: Degloving injury, (decollement), foot trauma, limb salvage, fluorescence angiography, negative pressure wound therapy.
Authors: Cecilie Jansen, Emil Villiam Holm-Rasmussen, Mette Stueland Wolthers. Copenhagen University Hospital, Rigshospitalet, Denmark.
Abstract
A 30-year-old previously healthy man was admitted to The Trauma Centre at Copenhagen University Hospital, Rigshospitalet after his left foot was crushed by a 1.5-ton forklift at work. He sustained a large open fracture and an extensive circumferential degloving injury involving the foot and ankle, while distal perfusion remained intact. Computed Tomography (CT) demonstrated multiple intra-articular fractures with suspected Lisfranc injury and no vascular injury on CT angiography. Following orthopedic stabilization, plastic surgical management focused on debridement, tissue viability assessment, skin and heel-pad preservation, and limb salvage. This case highlights the challenges of severe foot degloving and multidisciplinary limb-salvage management.
Patient medical history
The patient was previously healthy, had no significant past medical history, and was a non-smoker.
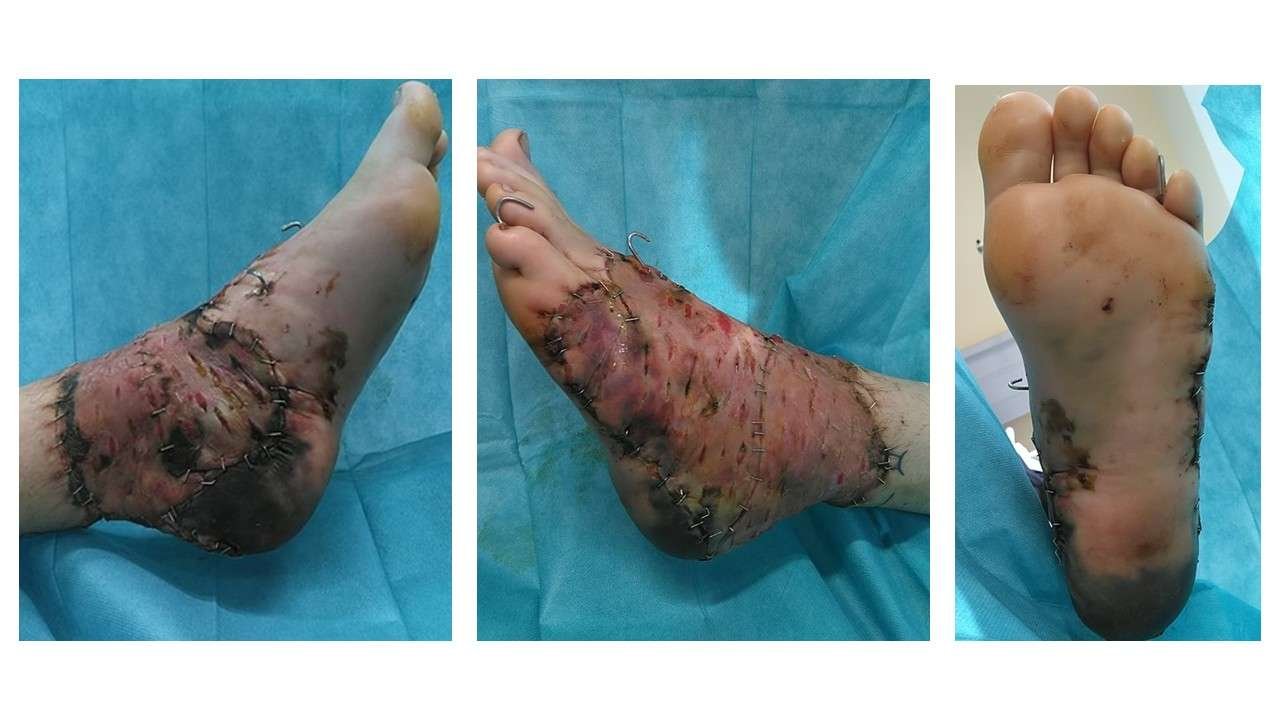
Before and After
Patient examination
On arrival at The Trauma Centre at Copenhagen University Hospital, Rigshospitalet, the patient was hemodynamically stable but slightly pale. He reported paresthesia in the left foot, but gross sensation was preserved.
Clinical examination revealed an approximately 15 cm open wound laterally on the left foot with exposed bone and tendon. A palpable pulse was present in the dorsalis pedis artery, whereas the posterior tibial artery pulse was not palpable. Capillary refill and sensation were preserved.
A trauma CT scan with intravenous contrast, including CT angiography of the lower leg was performed. Imaging demonstrated multiple intra-articular fractures distal to the talus with widening between the second metatarsal and medial cuneiform, raising suspicion of a Lisfranc injury. Air was present in the surrounding soft tissues. CT angiography showed no vascular injury, with normal contrast opacification of both the dorsalis pedis and posterior tibial arteries.
Pre-operative considerations
Given the high-energy crush mechanism and the extensive open soft-tissue injury, urgent surgical intervention was indicated. The main preoperative priorities were skeletal stabilization, thorough debridement of devitalized tissue, assessment of soft-tissue viability, preservation of the skin and the heel pad and multidisciplinary planning for limb salvage involving both orthopedic and plastic surgeons. The visible skin injury was considered likely to underestimate the full extent of soft tissue devascularization, making intraoperative reassessment essential.
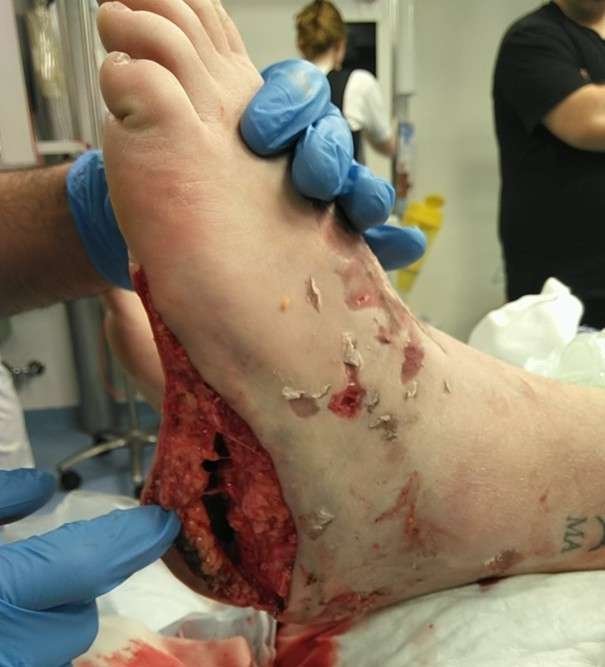
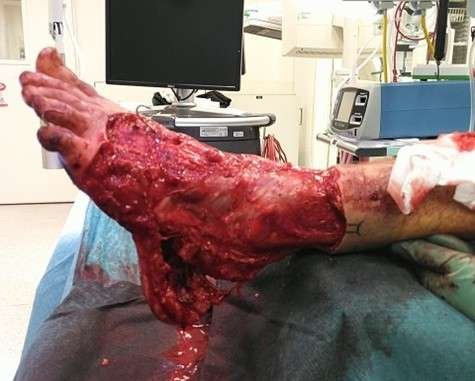
Intraoperative examination
Intraoperative examination revealed a large open degloving injury, predominantly circumferential around the ankle, extending approximately one handbreadth proximally. The injury continued distally over the dorsum of the foot and around both malleoli. The plantar surface showed partial avulsion involving the heel pad and the medial and lateral borders of the foot. Communication between the open wound and the degloving cavity was noted at the posteromedial heel and ankle region. Areas of crush injury and skin discoloration were present, particularly on the dorsum and medial aspect of the heel, indicating a risk of secondary necrosis. Palpable dorsalis pedis artery pulse was present, whereas the posterior tibial artery pulse was uncertain.
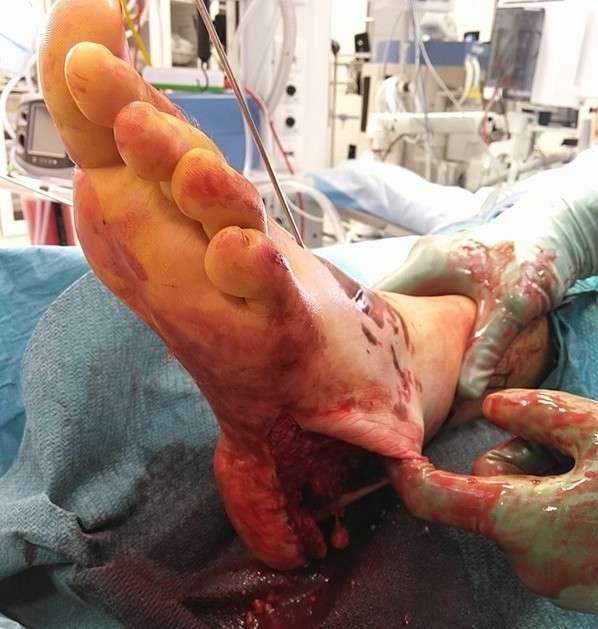
Systematic revision guided by intraoperative fluorescence angiography
Intraoperative fluorescence angiography with intravenous administration of Indocyanine green
(ICG) dye demonstrated reduced or absent perfusion in a circumferential zone around the ancle, approximately 10 cm wide, extending from lateral to medial malleolus and distally over the dorsum of the foot. Perfusion was relatively preserved on the plantar aspect, including the heel pad. Clearly non-viable and undermined skin was marked and excised, leaving a 1 cm border, which was harvested as full-thickness. Systematic revision ensured complete removal of devitalized tissue while preserving viable structures.
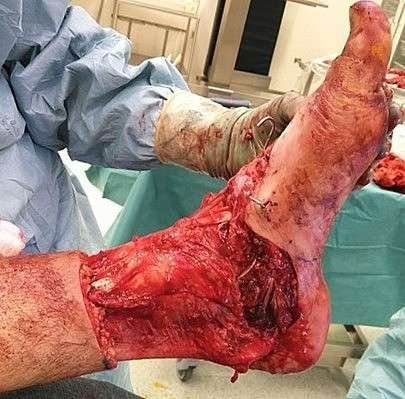
Repositioned heel pad
Hemostasis was obtained. The plantar surface and heel pad were repositioned and anchored to the deep fascia and plantar structures using 2-0 Vicryl to reduce dead space and optimize the chance for tissue survival.
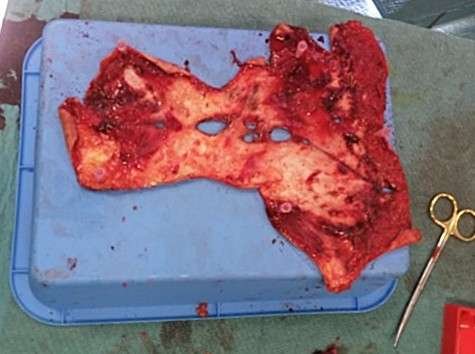
Full-thickness skin graft.
The avulsed tissue was harvested, trimmed/defatted, and meshed to a large full-thickness skin graft.
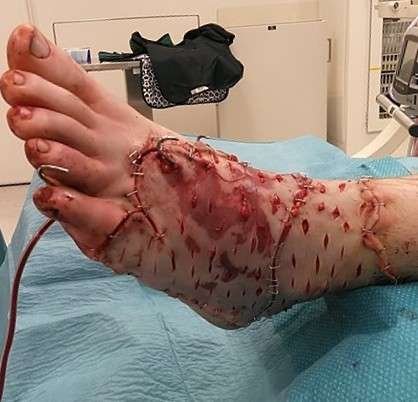
The full-thickness skin graft was applied over the foot and ancle.
The full-thickness skin graft was applied over the foot and ancle and secured with staples. A 14-F suction drain was placed.
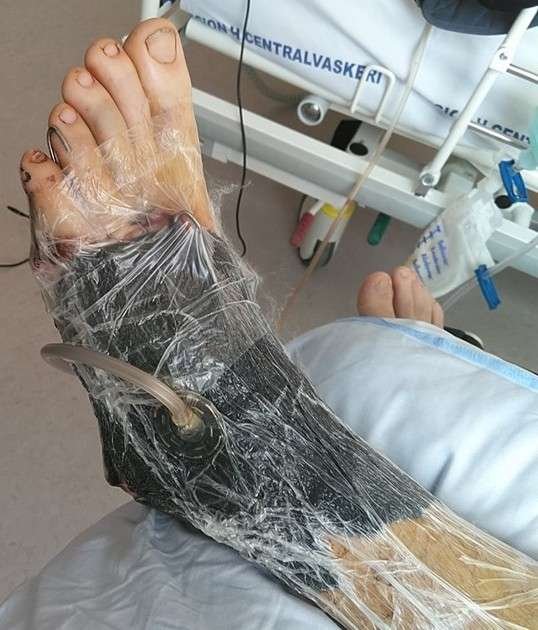
Negative-pressure wound therapy
The graft was dressed with Cuticerin, and surrounding skin was prepared with adhesive film. A black sponge was applied over the grafted area and connected to continuous negative pressure at 125 mmHg.
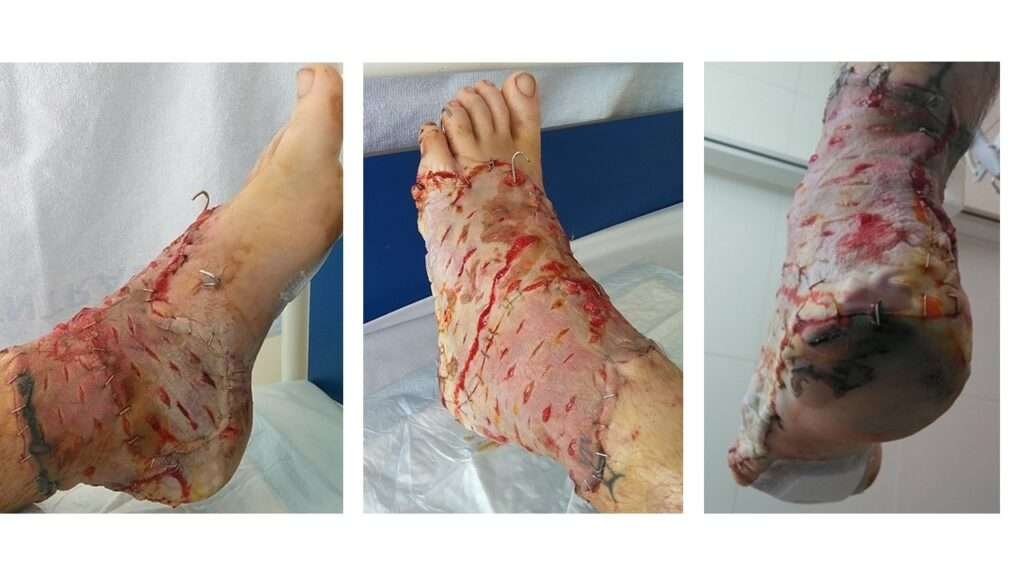
Post-operative Assessment (Day 5)
Five days postoperatively, the full-thickness skin graft, particularly in the caudal/posterior region, showed mild maceration with some open mesh interstices. Overall graft take is difficult to assess at this stage. Most of the plantar surface appears pink with good capillary refill and preserved sensation. The heel pad and surrounding area remain somewhat questionable; the skin appears slightly pale to bluish-purple but is warm to touch. Toe mobility is intact, with preserved capillary refill and sensation throughout.
The full-thickness skin graft was then re-covered with a Peel and Place Dressing and NPWT was continued. A transparent Tegaderm dressing was applied to the heel to allow monitoring of the underlying skin while providing gentle compression to help reapproximate the plantar skin and heel pad to the underlying tissue.
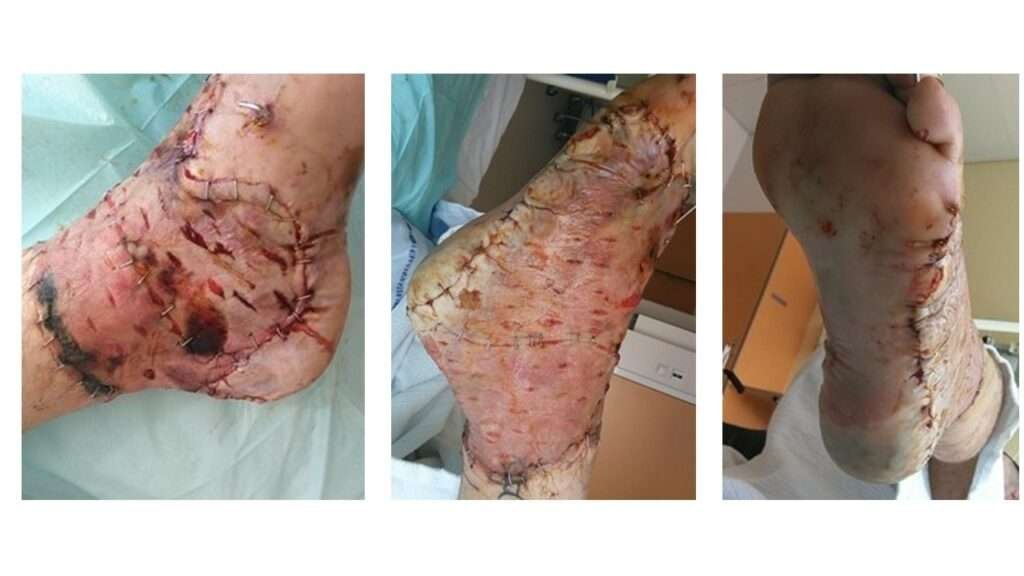
Post-operative Assessment (Day 10)
Ten days postoperatively, the full-thickness skin graft, particularly in the caudal/posterior region, showed signs of mild maceration. Overall graft take was estimated at approximately 90%. Most of the plantar surface still appears pink with good capillary refill and preserved sensation. The heel pad and surrounding area appears pink and warm.
The full-thickness skin graft and heel pad was then covered with nitrofurantoin impregnated gauze, Jelonet dressing and a compression bandage with daily dressing changes and air dry to prevent the development of maceration.
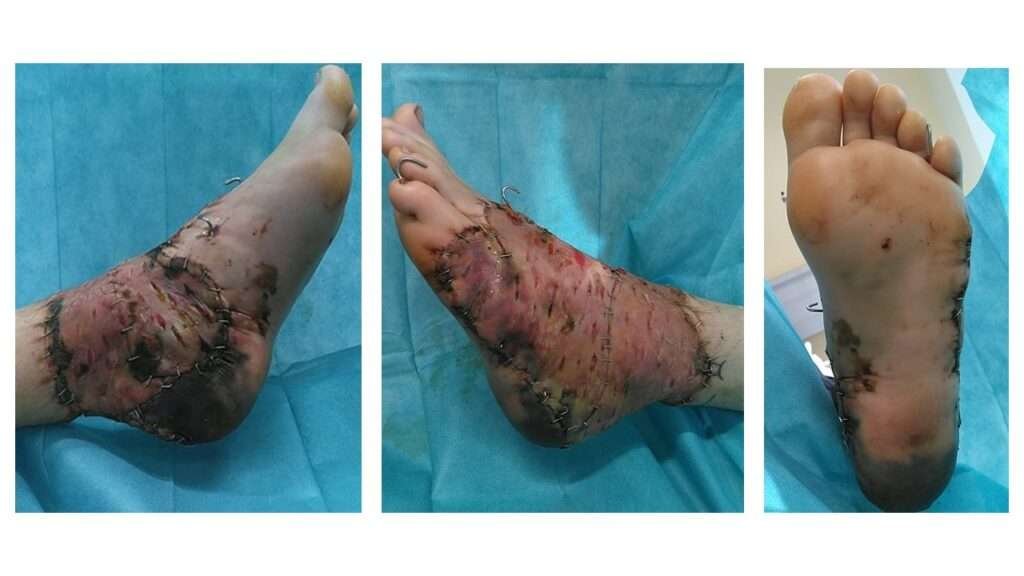
Post-operative Assessment (Day 14)
Fourteen days postoperatively a line of demarcation is slowly beginning to appear at the heel pad. There are early signs of marginal necrosis at the site of the full-thickness skin graft. Overall graft take was estimated at approximately 90%. Most of the plantar surface still appears pink with good capillary refill and preserved sensation. The demarcation will be monitored for the next months, with a conservative approach.
Pearls
- Early recognition of degloving injuries is crucial for optimal planning and limb salvage.
- Fluorescence angiography provides an objective assessment of tissue perfusion and may help guide debridement and graft planning.
- Staged reconstruction with temporary negative-pressure wound therapy (NPWT) allows repeated assessment of tissue viability and graft adherence.
- Preservation and reattachment of the heel pad, when feasible, are essential for later function and weight bearing because the heel pad consists of specialized tissue that cannot be replaced by ordinary soft tissue
Pitfalls
- The extent of degloving and devascularization may be underestimated at initial presentation leading to delayed management.
- Overly conservative debridement risk secondary necrosis and infection, whereas overaggressive debridement may sacrifice viable plantar structures including the heel pad.
- Meticulous hemostasis and adequate drainage are essential to reduce the risk of hematoma beneath the graft and compromised graft take.
Post-operative plan
The post-operative plan included NPWT dressing changes every 5–7 days. The left foot and lower limb were kept elevated at all times, with pressure avoided over the heel, and were kept warm using padding and gauze with additional covering as needed. The patient remained on strict bed rest for the first three days, followed by wheelchair mobilization with the leg elevated until the first dressing change. Weight-bearing on the affected foot was restricted for six weeks according to orthopedic guidelines. Continuous suction drainage was maintained until NPWT removal.
Once the skin graft is considered well healed, or near complete healed, the patient can be discharged home with daily dressing changes at home and a follow-up every 14th day at the department of plastic surgery, to assess healing, function, and any need for secondary revision. The expectation is that the heel will progress toward spontaneous healing after demarcation.
References
Hakim S, Ahmed K, El-Menyar A, Jabbour G, Peralta R, Nabir S, Mekkodathil A, Abdelrahman H, Al-Hassani A, Al-Thani H. Patterns and management of degloving injuries: a single national level 1 trauma center experience. World J Emerg Surg. 2016 Jul 27;11:35. doi: 10.1186/s13017-016-0093-2. PMID: 27468300; PMCID: PMC4962500.
Velazquez C, Whitaker L, Pestana IA. Degloving Soft Tissue Injuries of the Extremity: Characterization, Categorization, Outcomes, and Management. Plast Reconstr Surg Glob Open. 2020 Nov 23;8(11):e3277. doi: 10.1097/GOX.0000000000003277. PMID: 33299726; PMCID: PMC7722549.
Kristiansen CS, Norling AL, Nielsen AE, Holmgaard R, Lang CL. Décollement [Décollement]. Ugeskr Laeger. 2025 Nov 24;187(48):V05250357. Danish. doi: 10.61409/V05250357. PMID: 41311131.
Lauritzen E, Lang CL, Jensen LT. Vellykket behandling af décollement-læsion med fuldhudstransplantat på overekstremitet. Ugeskr Laeger. 2019 Jan 14;181(3):V70021. Danish. PMID: 30686278.
Vasella M, Guidi M, Waldner M, Calcagni M, Giovanoli P, Frueh FS. Fluorescence angiography-assisted debridement of critically perfused glabrous skin in degloving foot injuries: two case reports. Medicine (Baltimore). 2021;100(22):e26235. doi:10.1097/MD.0000000000026235.